Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Daniela Vanousova, Dermatologist, Czech Republic; Chief Editor: Dr Amanda Oakley, Dermatologist, Hamilton, New Zealand, July 2015. DermNet Revision October 2021
Introduction Causes Demographics Clinical features Differential diagnoses Diagnosis Treatment Outcome
Acrodermatitis chronica atrophicans (ACA) is the most common skin manifestation of the late stage of Lyme disease.
Acrodermatitis chronica atrophicans is caused by ongoing active skin infection by the bacteria Borrelia afzelii, found mostly in Europe. These bacteria are transmitted by a tick bite months or years before ACA develops.
Acrodermatitis chronica atrophicans mostly affects middle-aged and older people, especially women. However, it can develop in anyone with untreated borrelial infection, including children. It is estimated that it arises in about 1–10% of people in Europe that have been infected with Lyme disease bacteria.
Acrodermatitis chronica atrophicans typically presents as a unilateral violet discolouration of the extensor parts of the upper or lower limbs, especially the dorsum of the hand, elbow, instep, ankle, or knee. However, it can appear anywhere on the body and can be bilateral.
ACA develops in 2 stages. Initial inflammation is followed by progressive fibrosis and cutaneous atrophy over months or years.
Less common features of ACA include fibrous papules and plaques, and skin coloured nodules.
Most patients have a history of tick bite. Some of them may recall a rash consistent with erythema migrans some months or years earlier, often affecting the same limb. Erythema migrans is a ring-like rash that occurs around the site of a Borrelia-infected tick bite. [see Erythema migrans images]
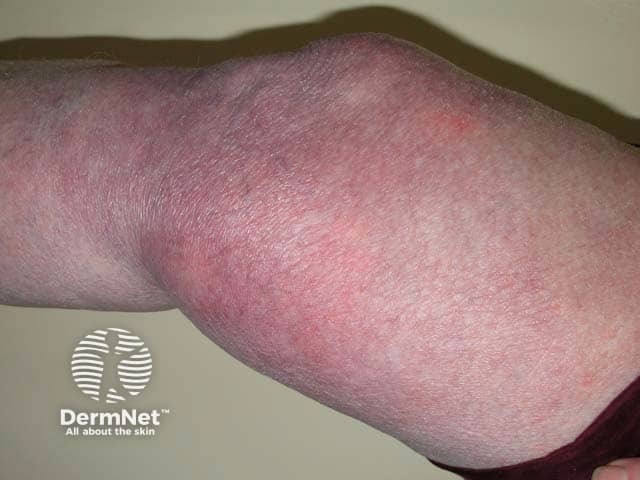
Inflammatory stage
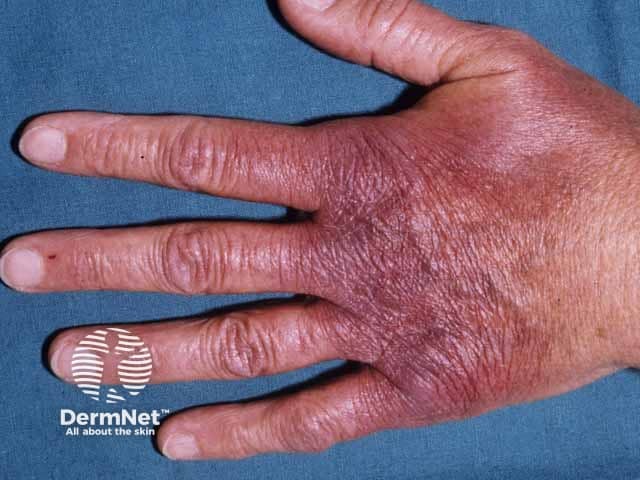
Inflammatory stage
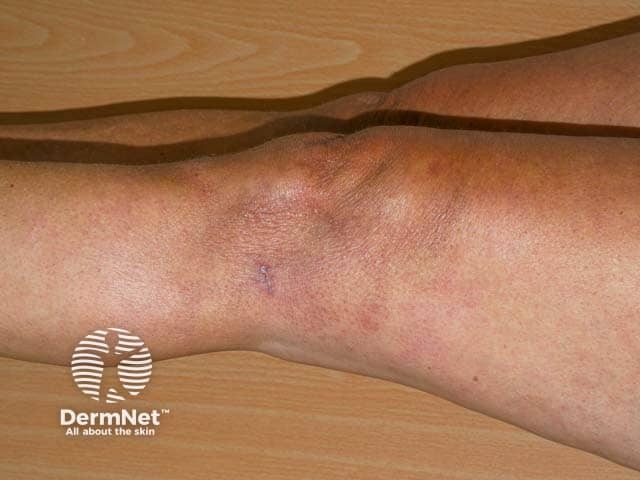
Atrophic stage
Acrodermatitis chronica migrans is a skin sign of the late stage of Lyme disease. Other features of late-stage Lyme disease in patients with ACA include:
Acrodermatitis chronica migrans is probably underdiagnosed. It is essential to obtain a detailed medical history and to determine whether there has been exposure to ticks (eg, being in grass or woodlands in endemic areas) or any previous manifestation of Lyme disease. When suspicious of ACA, a careful general skin examination should be carried out.
The diagnosis of ACA is confirmed on laboratory tests:
There is no vaccine against Borellia so prevention is aimed at avoiding a tick bite or prompt removal of a tick if acquired.
Acrodermatitis chronica atrophicans is treated with antibiotics. The choice of antibiotic and duration of treatment depends on which other organs are involved and the severity of symptoms. Antibiotics used for ACA may include:
Patients with ACA may require referral to other specialists if there is extracutaneous organ involvement.
Acrodermatitis chronica atrophicans is most effectively treated in the early inflammatory stage when the skin changes are reversible. In the later atrophic stage, the infection can be eradicated, but skin changes persist.