Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Vanessa Ngan, Staff Writer, 2003. Updated by Dr Ebtisam Elghblawi, Dermatologist, Tripoli, Libya, and DermNet Editor in Chief, A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand, November 2017.
Introduction Demographics Clinical features Classification Complications Treatment
Aplasia cutis congenita describes the congenital absence of skin. The commonest form presents as a scalp defect at birth. Aplasia cutis is also a component of a number of genetic syndromes.
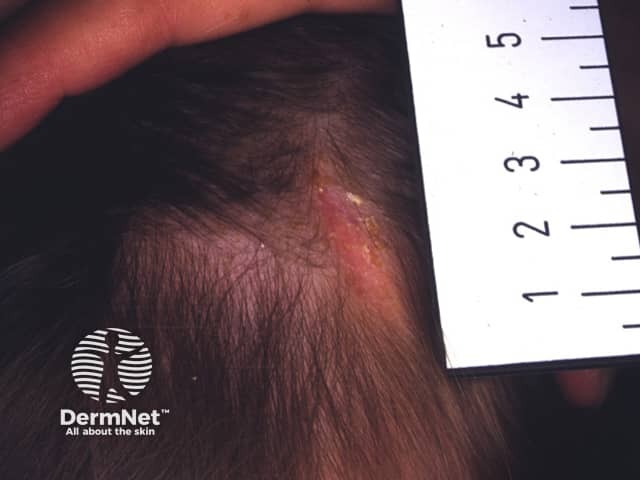
Aplasia cutis

Aplasia cutis
Factors contributing to aplasia cutis include:
Aplasia cutis is rare and no particular race or sex is at greater risk.
In 70–80% of cases, aplasia cutis affects the scalp lateral to the midline, but lesions may also occur on the face, trunk, or limbs, sometimes symmetrically.
The Frieden classification system for aplasia cutis has 9 groups based on the number and location of the lesions and associated malformations.
Scalp aplasia cutis congenita without other anomalies
Scalp aplasia cutis congenita with limb anomalies: includes Adams-Oliver syndrome
Scalp aplasia cutis congenita with solitary epidermal or sebaceous (organoid) naevus or an epidermal naevus syndrome
Aplasia cutis congenita overlying deep embryologic malformation
Stellate aplasia cutis congenita of trunk or limb associated with fetus papyraceous or placental infarct
Epidermolysis bullosa with congenital absence of skin (aplasia cutis congenita of lower limb associated with epidermolysis bullosa (Bart syndrome)
Aplasia cutis congenita of limb without epidermolysis bullosa
Aplasia cutis congenita due to teratogens such as intrauterine infection with herpes simplex or varicella or drugs such as methimazole or carbimazole
Aplasia cutis congenita associated with malformation syndromes including trisomy 13 with large membranous defect (Patau syndrome), Wolf-Hirschhorn syndrome (deletion of the short arm of chromosome 4) with midline scalp defects, Setleis syndrome with bitemporal aplasia cutis congenita and abnormal eyelashes; Johanson-Blizzard syndrome with stellate scalp defects; focal dermal hypoplasia (Goltz syndrome); and others.
Complications of aplasia cutis rarely occur but may include:
Small areas of aplasia cutis usually heal spontaneously over time, forming a hairless scar. To prevent infection gentle cleaning and bland ointments may be used. If infection occurs, antibiotics can be used.
Larger lesions or multiple scalp defects may require surgical repair; sometimes skin or bone grafting may be required. Tissue expanders may be employed.