Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Peggy Chen, Dermatology Registrar, Middlemore Hospital, Auckland, New Zealand; Chief Editor: Dr Amanda Oakley, Dermatologist, Hamilton, New Zealand, March 2014.
Childhood bullous pemphigoid is a rare blistering disease affecting children under the age of 18. Unlike bullous pemphigoid in adults:
Childhood bullous pemphigoid has a favourable prognosis and results in minimal scarring.
Childhood bullous pemphigoid is an autoimmune disorder. This means that an individual’s immune system starts reacting against his or her own tissue. In childhood bullous pemphigoid, autoantibodies react with components of the basement membrane (this membrane separates the epidermal and dermal layers of the skin), particularly the skin cell adhesion plate hemidesmosome-associated proteins BP180 and less frequently BP230. These proteins are within the non-collagenous (NC) 16A domain of collagen XVII.
In many patients with childhood bullous pemphigoid, skin antibodies can be detected in their blood stream. This is known as a positive indirect immunofluorescence test, because the antibodies are detected using fluorescence.
The diagnosis of childhood bullous pemphigoid is based on the following features:
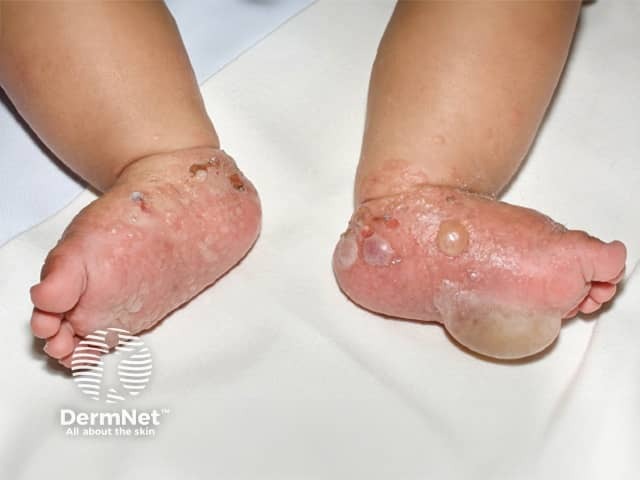
Childhood bullous pemphigoid
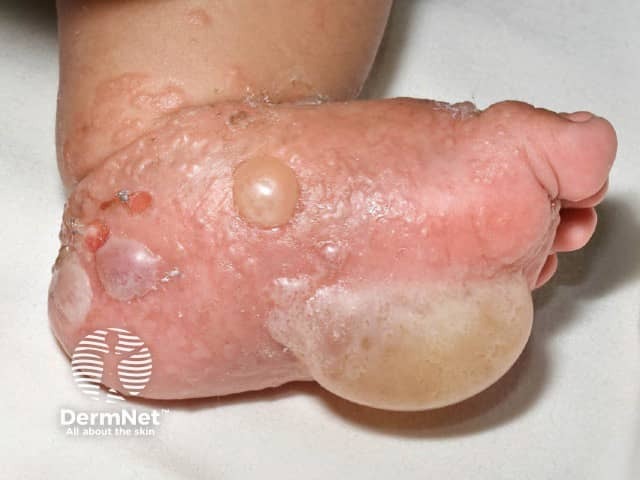
Childhood bullous pemphigoid
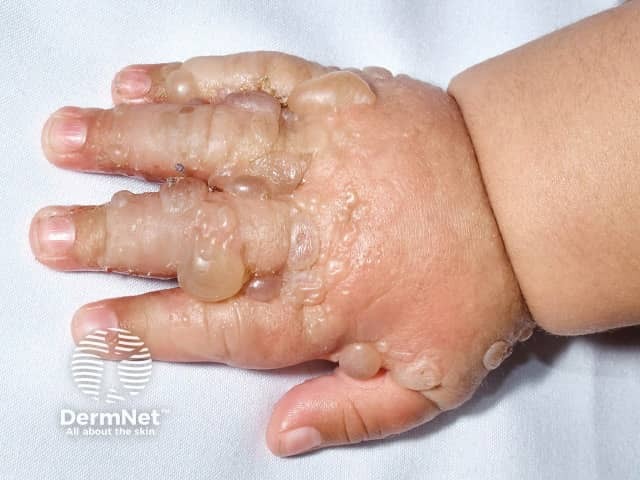
Childhood bullous pemphigoid
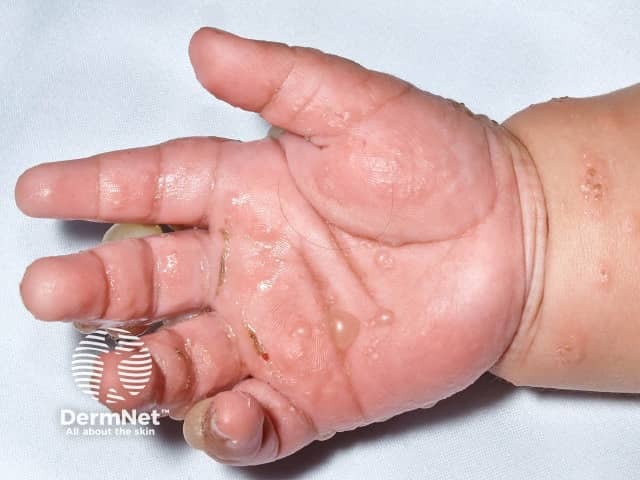
Childhood bullous pemphigoid
In most cases the diagnosis of childhood bullous pemphigoid is made by a combination of typical clinical features and the results of biopsy of a blister.
Under the microscope, the pathologist can see a split between the outside layer of the skin, the epidermis, and the inside layer, the dermis – which means it is a subepidermal blister. See pathology of bullous pemphigoid.
Direct immunofluorescence staining highlights linear antibodies along the basement membrane of the skin biopsy.
Treatment of childhood bullous pemphigoid is similar to that of adult bullous pemphigoid. The aim of treatment is to stop the formation of new blisters.
Ultra-potent topical steroids such as clobetasol propionate may be sufficient as a monotherapy, however many patients require systemic corticosteroids, with a starting dose of 1–2 mg/kg body weight each day of prednisone or prednisolone.
Other treatments that have been reported to be of benefit in childhood bullous pemphigoid are:
These are used either as monotherapy, or in combination with systemic corticosteroids.
In recalcitrant cases, the following medicines have been reported to be effective:
Overall, patients with childhood bullous pemphigoid have a favourable prognosis. The rash eventually clears up and treatment can be withdrawn.