Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Introduction
Demographics
Causes
Signs and symptoms
Diagnosis
Treatment
Granulomatous cheilitis refers to an uncommon condition in which there is lumpy swelling of the lips. It is also known as cheilitis granulomatosa or Miescher cheilitis. It is part of the spectrum of orofacial granulomatosis including Miescher-Melkersson-Rosenthal syndrome (granulomatous cheilitis, facial palsy and fissuring of the tongue).
Granulomatous cheilitis is rare. It may occur in people of any race, sex and age, although onset is usually in early adulthood.
The causes of granulomatous cheilitis include:
Granulomas in Miescher cheilitis are confined to the lip. In other cases of granulomatous cheilitis, granulomatous disease is more widespread.
The first symptom of granulomatous cheilitis is a sudden swelling of the upper lip. In most cases, this first episode goes away within hours or days. Swelling of the lower lip and one or both cheeks may follow in orofacial granulomatosis. Less commonly, the forehead, eyelids, or one side of the scalp may be involved. The swelling may feel soft, firm or nodular when touched.
Recurrent attacks of granulomatous cheilitis may occur within days or even years after the first episode. At each episode, the swelling may become larger, more persistent and eventually become permanent. At this time the lips may crack, bleed and heal leaving a reddish-brown colour with scaling. This can be painful. Eventually, the lip takes on the consistency of hard rubber.

Granulomatous cheilitis
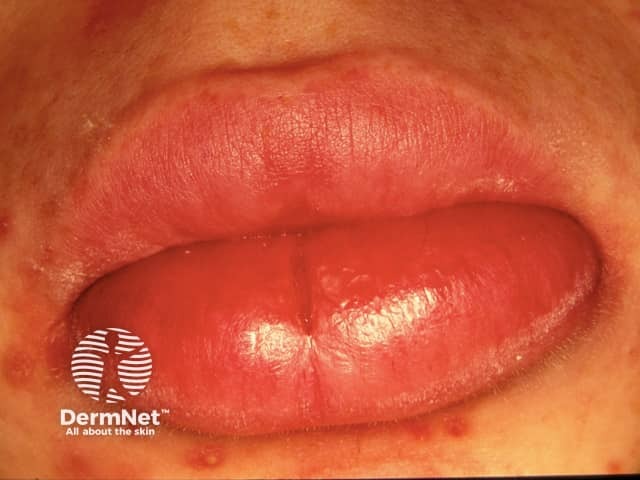
Granulomatous cheilitis
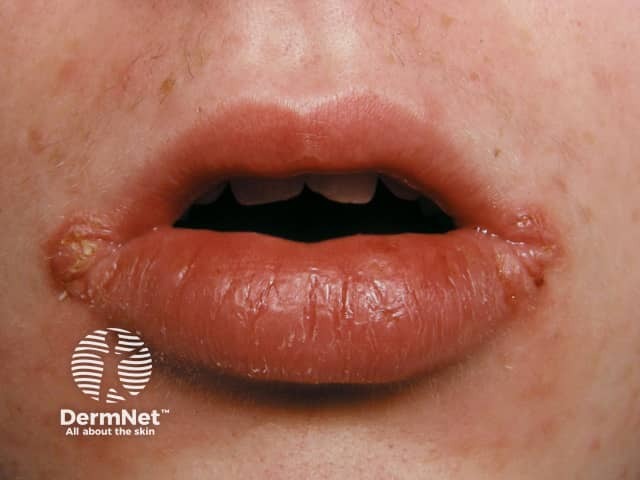
Granulomatous cheilitis
See more images of granulomatous cheilitis
Other symptoms that may accompany granulomatous cheilitis include:
The diagnosis is often suspected clinically. Skin biopsy of the affected tissue shows characteristic histopathology, in which there are granulomas, i.e. a mixed inflammatory cell infiltration, in the dermis (the deeper layer of the skin).
If it is related to an allergy, responsible dietary components or causative substances should be avoided longterm. If there is an underlying disease, systemic treatment for this may also reduce the swelling of the lips.
The following measures have been reported to reduce the severity of granulomatous cheilitis in at least some cases.