Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Samuel Der Sarkissian, General Practitioner, Shellharbour Medical Centre, NSW, Australia. DermNet Editor in Chief: Adjunct A/Prof. Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy edited by Gus Mitchell. March 2020.
Keratinocyte cancers Surgical margins Histological margins Importance of histological margins Adequate histological margins High-risk features Treatment if margins are inadequate Likelihood of reccurence Complications Treatment Follow-up
A keratinocyte cancer is a malignant neoplasm formed from the epidermal cells that produce keratin (keratinocytes). Keratinocyte cancers are classified as either squamous cell carcinomas (SCC) or basal cell carcinomas (BCC).
Keratinocyte cancers are considered low risk or high risk, depending on patient factors such as age and immune suppression status, and tumour factors including tumour site and histological subtype.
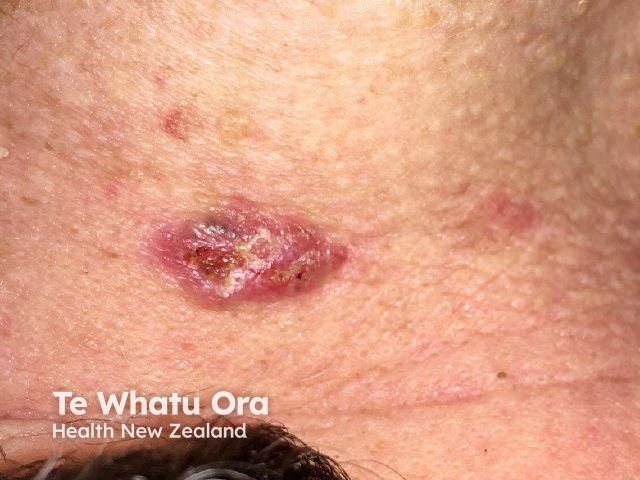
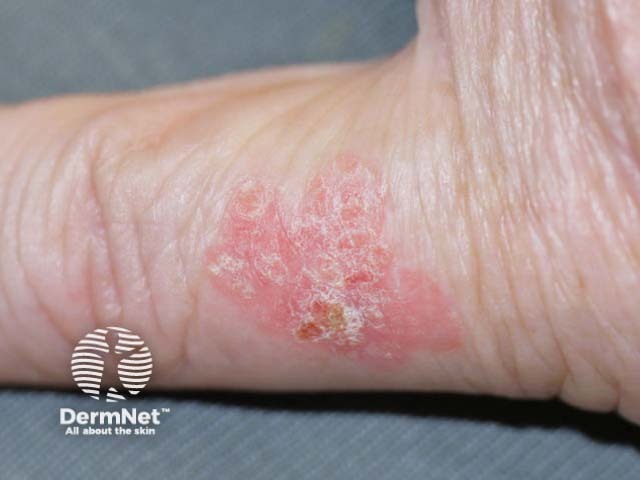
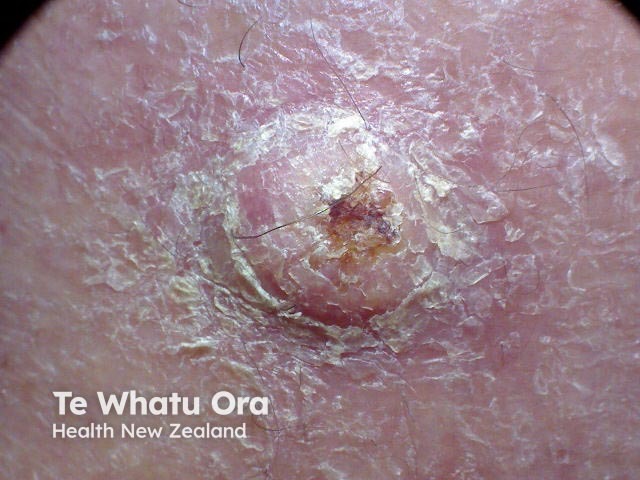
A surgical margin is a clinical measurement made just before a lesion is excised. The surgeon uses their naked eye or magnification (eg, a dermatoscope) to find the visible edge of the tumour, then measures the desired margin of normal skin to remove on either side of the tumour. A surgical marking pen is used to plan the excision site.
As a general guide, adequate surgical margins are 3–4 mm for a BCC and at least 4 mm for a low-risk SCC. There are no published guidelines for a high-risk SCC.

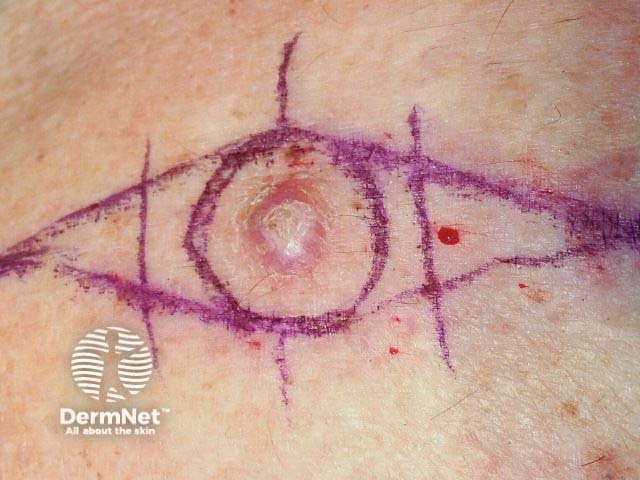
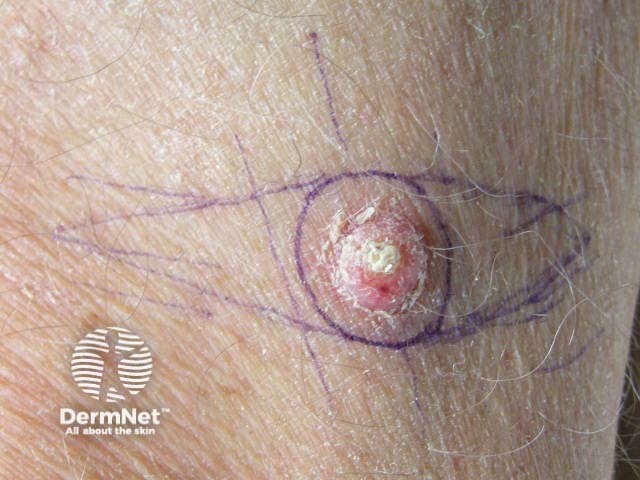
A histological margin is measured by a pathologist. It describes the amount of normal tissue bordering a tumour specimen.
Histological margins may be adequate, narrow, or inadequate.
An adequate histological margin is the acceptable distance of tumour cells from the histological margin, according to expert consensus and published research.
The desirable margin depends on the type of tumour and the technique used to remove it. Clinicopathological correlation and additional sections may be required, particularly when clinical margins have been difficult to assess or compromised by the anatomical location of the tumour (eg, a lesion close to the eye).
High-risk BCC may be defined by any of the following features:
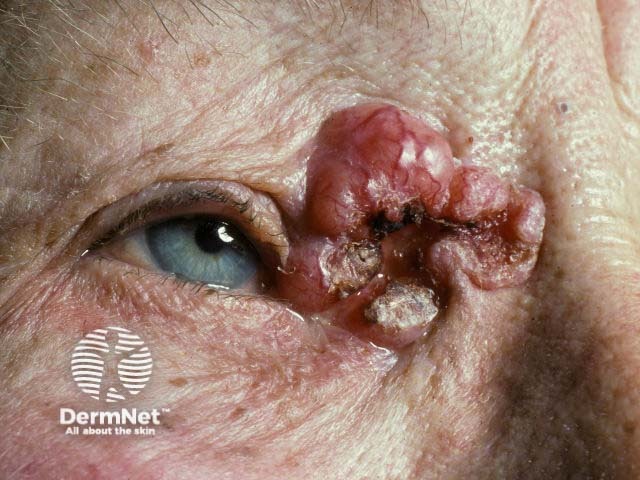
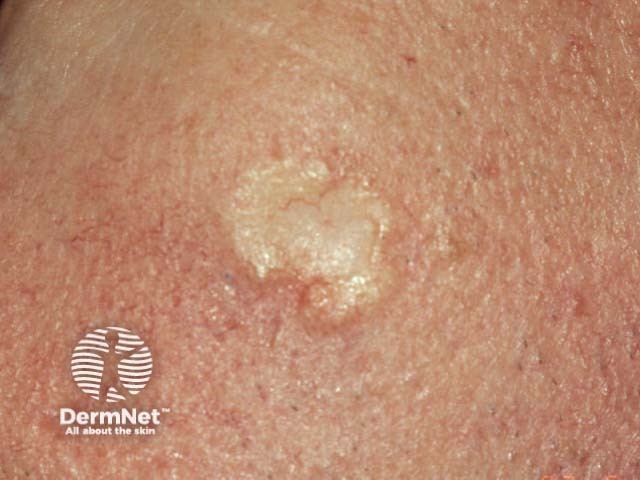
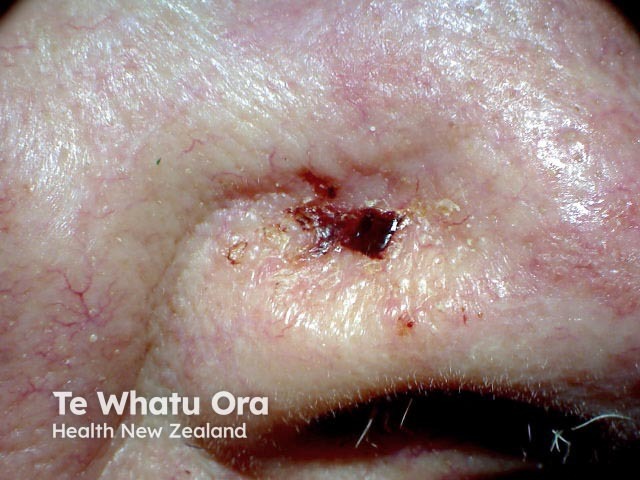
High-risk SCC may be defined by any of the following features:
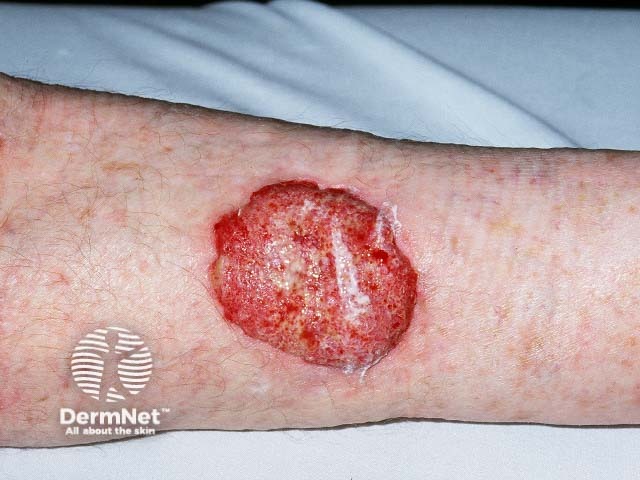
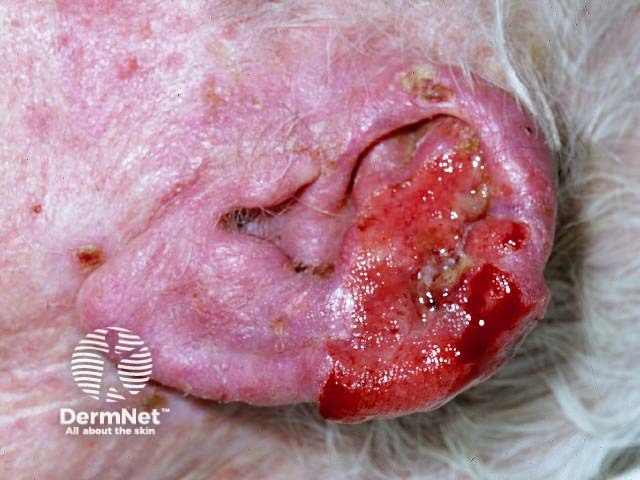
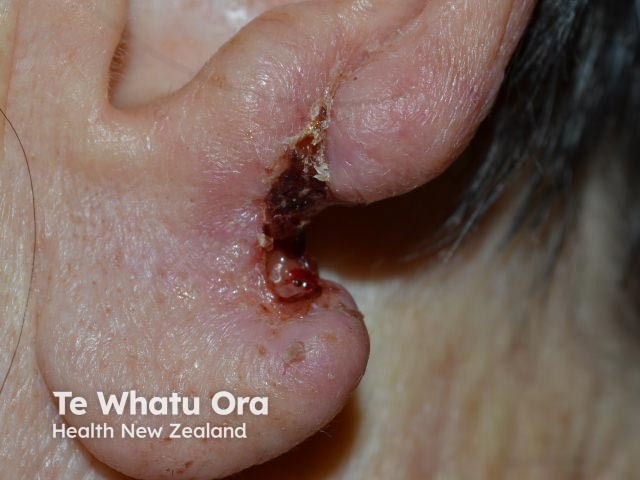
Perineural invasion may be seen on histology in up to 5% of keratinocyte cancers. Depending on the size of the nerves involved, it may pose a high-risk for local recurrence and, in SCC, for metastasis [6].
Tumours with perineural invasion should be referred to a specialist. Management may include:
If the histological margins are involved or inadequate, most low-risk BCCs should undergo re-excision to ensure clear margins. In select cases, radiotherapy may be a reasonable alternative. Persistent superficial BCC may occasionally be treated topically (eg, imiquimod cream).
Inadequately excised high-risk lesions should be referred to a specialist, depending on the clinician’s skill and tumour factors. To reduce unnecessary removal of healthy tissue, Mohs micrographic surgery may be considered, especially for lesions in high-risk areas.
Histological margins of less than 1 mm should lead to re-excision of an SCC. High-risk SCCs, especially on the head and neck, require referral to a specialist with expertise in this field.
Recurrence of a keratinocyte cancer depends on the type and risk category of the lesion, the type of treatment, the histological margins, and the clinician’s expertise.
For low-risk BCCs treated by surgical excision:
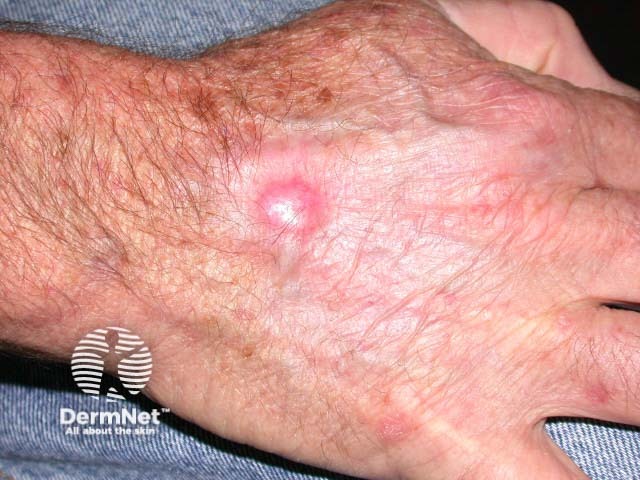
Nodular recurrent BCC
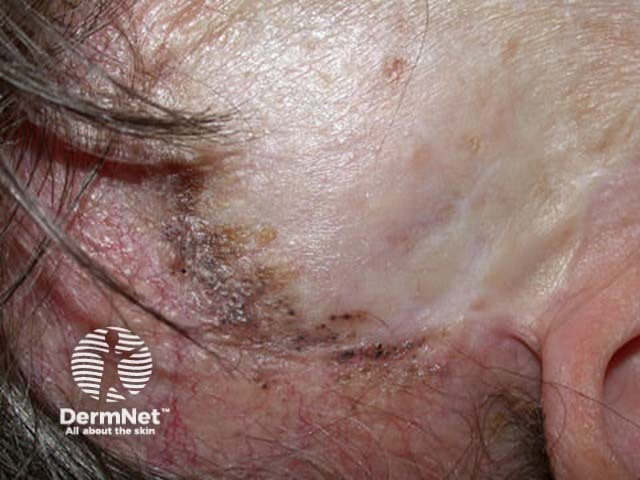
Recurrent pigmented BCC
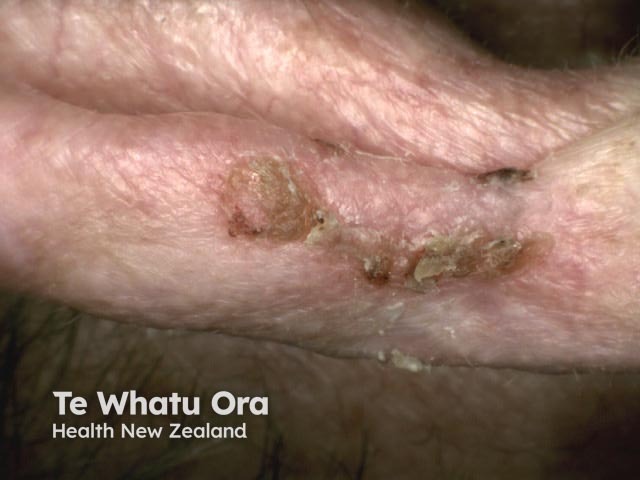
BCCs rarely metastasise but can be locally invasive and cause local tissue destruction. Recurrent BCCs usually require more aggressive treatment resulting in greater tissue loss and surgical complications.
Development of local recurrence of SCC is associated with further local recurrence in about 25% of lesions and subsequent metastasis to regional nodes in up to 30%. About a third of patients who develop regional metastasis will die from their SCC [9].
Recurrent BCC is treated by resection of the scar, the recurrent tumour, and a 3–4 mm margin of surrounding skin [10,11]. Specialist referral should be considered, especially if the tumour edges are hard to detect. Mohs micrographic surgery may be indicated.
Specialist referral is recommended for recurrent SCC due to the risk of developing further recurrence and metastasis.
Follow-up requires inspection of the treated area using dermoscopy and palpation of adjacent structures [12].
An annual skin check is recommended for all patients with a history of skin cancer.