Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Anthony Yung, Dermatologist, Hamilton, New Zealand; Chief Editor: Dr Amanda Oakley, Dermatologist, Hamilton, New Zealand, March 2014.
Introduction - IgG4
Introduction - IgG4-related disease
Causes
Demographics
Clinical features
Diagnosis
Treatment
Prognosis
IgG4 is a subclass of IgG, which is the most common form of immunoglobulin. IgG accounts for 75% of antibodies circulating in the blood, which are an essential part of the secondary immune response to infection and toxins. IgG is made by plasma cells, a specific type of B lymphocyte.
There are four subclasses of IgG. Subclass IgG4 is the least common of these, accounting for about 4% of IgG in serum. IgG4 has a unique structure. Its specific biological role is uncertain. However, IgG4 is known to play a role in protection against type 1 hypersensitivity reactions, for example to bee venom, and in the pathogenesis of autoimmune blistering diseases such as pemphigus vulgaris, helminth infections, and malignancy including melanoma.
IgG4-related disease is a newly-described rare syndrome consisting of many disease entities that were previously thought to be unrelated. These conditions have the pathological features of:
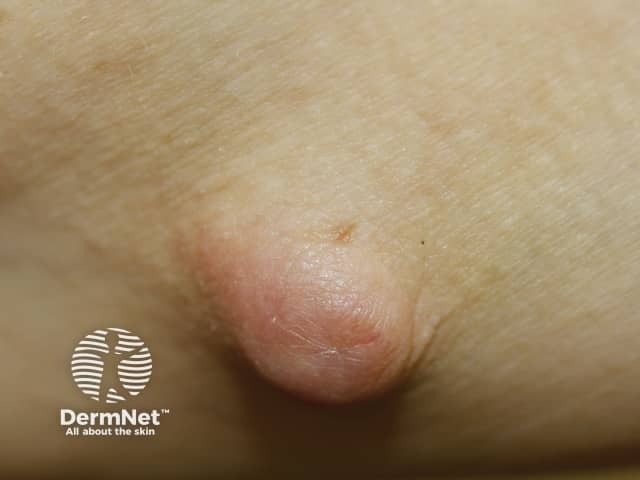
IgG4-related disease: cutaneous inflammatory pseudotumour
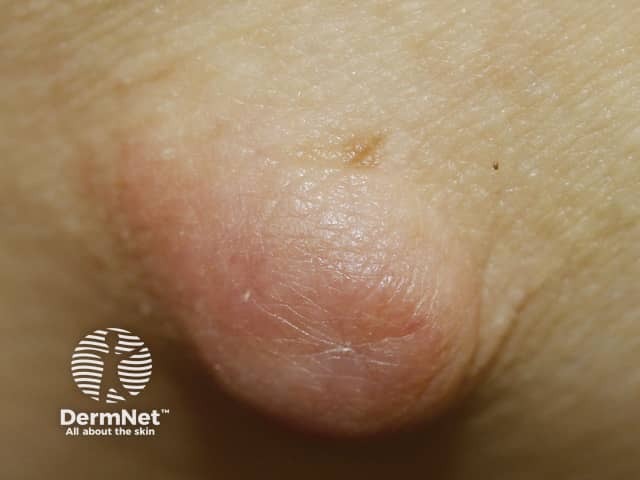
IgG4-related disease: cutaneous inflammatory pseudotumour
Elevated serum IgG4 is present in 60–70% patients.
The cause of IgG4-related disease is unknown.
Most patients described with IgG4-related disease are middle-aged or older men.
IgG4-related disease presents in various ways.
Organ-specific IgG4-related disease |
|
|---|---|
Organ |
Disease |
Gastrointestinal disease |
|
Lymph node involvement |
|
Salivary and lacrimal disease |
|
Eye disease |
|
Heart disease |
|
Thyroid disease |
|
Lung disease |
|
Kidney disease |
|
Skin disease |
|
Other |
|
The diagnosis of IgG4-related disease can be difficult, as multiple organs may be involved simultaneously. Diagnostic criteria have not been fully developed.
Investigation in suspected IgG4-related disease requires a combination of clinical, endoscopic, radiological and serological tests looking for organ involvement and end-organ damage (eg, hormonal abnormalities).
Tissue diagnosis requires a biopsy of affected organ tissues, including skin biopsy. See IgG4-related skin disease pathology. Features include:
Blood tests are not diagnostic but may show:
There are specific criteria for the diagnosis of some tissue-specific disorders, such as autoimmune pancreatitis.
IgG4-related disease is usually treated with systemic steroids, often prednisone 40 mg per day for 2–4 weeks followed by a gradual tapering of the dose.
In patients that cannot be taken off prednisone, a steroid-sparing agent like azathioprine or mycophenolate may be used. Rituximab, a B cell-depleting monoclonal antibody, has been used with some success. Inebilizumab depletes CD19+ B cells and can reduce the flares of IgG4-related disease.
Organ-specific replacement therapy may be required:
Prognosis of IgG4-related disease is variable. It may spontaneously resolve or persist, with remitting and relapsing symptoms.
Major causes for morbidity and mortality are significant organ involvement such as:
IgG4-related disease may be associated with a possible increased risk of non-Hodgkin lymphoma. It is not known if IgG4-related disease leads to an increased risk of other forms of cancer.