Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Nicholas De Rosa, unaccredited trainee in dermatology, Department of Dermatology, St Vincent’s Hospital Sydney, NSW, Australia. DermNet New Zealand Editor in Chief: Hon A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. July 2017. Copy Editors: Gus Mitchell/Maria McGivern. July 2017.
Introduction - insulin
Introduction - insulin resistance
Demographics
Causes
Clinical features
Complications
Diagnosis
Treatment
Insulin is a polypeptide hormone that is produced by β cells of the pancreas and controls blood glucose (sugar) concentrations. High blood glucose concentrations stimulate the secretion of insulin, which transfers glucose from the bloodstream into muscle, fat and liver cells. This promotes the storage of glucose for future energy needs, and in healthy individuals, this feedback mechanism keeps the body at euglycaemia (average glucose concentrations).
Insulin resistance is defined as a subnormal glucose response to a given concentration of insulin.
The natural progression of insulin resistance first involves hyperinsulinaemia (high levels of insulin) after meals and is later followed by fasting hyperinsulinaemia. The failure of compensatory mechanisms to maintain euglycaemia lead to hyperglycaemia, impaired glucose tolerance and diabetes mellitus.
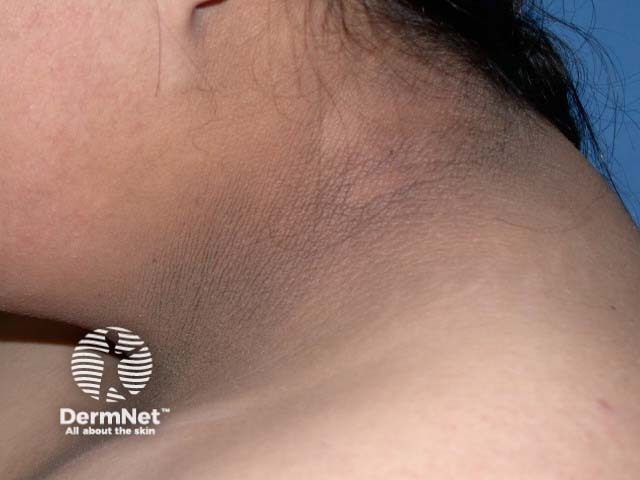
Acanthosis nigricans
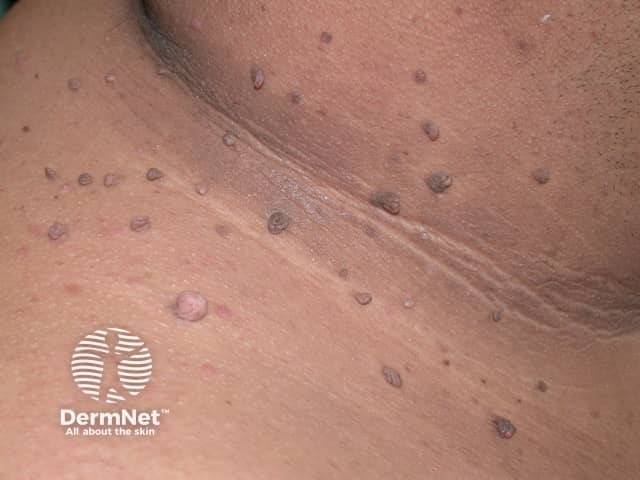
Skin tags
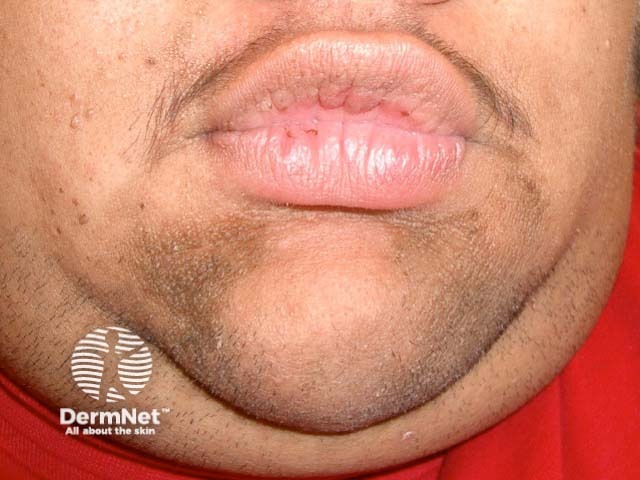
Acne, hirsutism + acanthosis nigricans
Insulin resistance is found in both men and women of all races and ethnicities. It is especially prevalent where people lead a sedentary lifestyle and consume a Western diet.
Insulin resistance is influenced by a combination of genetic, epigenetic and environmental factors.
Insulin resistance can rarely be the result of inherited metabolic disease. These include:
The majority of patients have secondary insulin resistance, which may be multifactorial.
Insulin resistance is associated with a wide variety of clinical presentations. Factors to consider include:
Insulin resistance is thought to induce skin changes through hyperinsulinaemia, which activates insulin growth factor-1 (IGF-1) receptors in fibroblasts and keratinocytes and stimulates their proliferation. Hyperinsulinaemia can also influence sex steroid production and increase free testosterone.
The skin manifestations of insulin resistance can help to diagnose the condition and its complications. Skin manifestations can include:
Skin diseases that have commonly been associated with insulin resistance and metabolic syndrome include:
The long-term consequences of insulin resistance include the effects of diabetes (eg, peripheral vascular disease, kidney disease, and visual complications) and certain malignancies associated with obesity and insulin resistance (eg, colon, breast, and endometrial cancers).
The hyperinsulinaemia, hyperglycaemia, and release of adipocyte cytokines associated with insulin resistance lead to vascular endothelial dysfunction, dyslipidaemia, hypertension, and vascular inflammation. These effects promote the development of the atherosclerotic cardiovascular disease.
There is currently no validated test to measure insulin resistance in clinical practice, and the diagnosis is usually made clinically.
While the euglycaemic insulin clamp technique is the gold-standard technique to diagnose insulin resistance in the research setting, it is complicated, invasive and costly, and rarely used in clinical practice.
Blood tests in patients with insulin resistance may reveal:
The presence of obesity, hypertension, increased fasting glucose and triglyceride concentrations, and low HDL (high-density lipoprotein) is used to diagnose metabolic syndrome.
The diagnosis of polycystic ovarian syndrome may be supported by the detection of multiple ovarian cysts on pelvic ultrasound examination.
There are no published guidelines on the management of insulin resistance per se.
Treatment that has been shown to decrease insulin resistance includes: