Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Jade Nutting, Medical Student, University of Sydney, Sydney, NSW, Australia. DermNet Editor in Chief: Adjunct A/Prof. Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy edited by Gus Mitchell/Maria McGivern. December 2018.
Introduction Demographics Causes Clinical features Complications Diagnosis Differential diagnoses Treatment Outcome
Keratolytic winter erythema is a rare inherited skin disorder characterised by recurrent palmoplantar erythema and peeling that is often worse in winter months [1]. It is also known as Oudtshoorn disease and erythrokeratolysis hiemalis.
Keratolytic winter erythema was first described in 1977 by dermatologists in South Africa who observed a skin condition prevalent in families in the Oudtshoorn area of Western Cape [2].
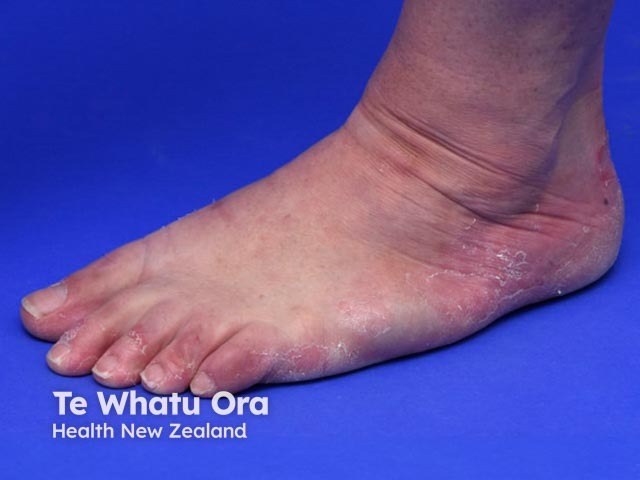
Keratolytic winter erythema
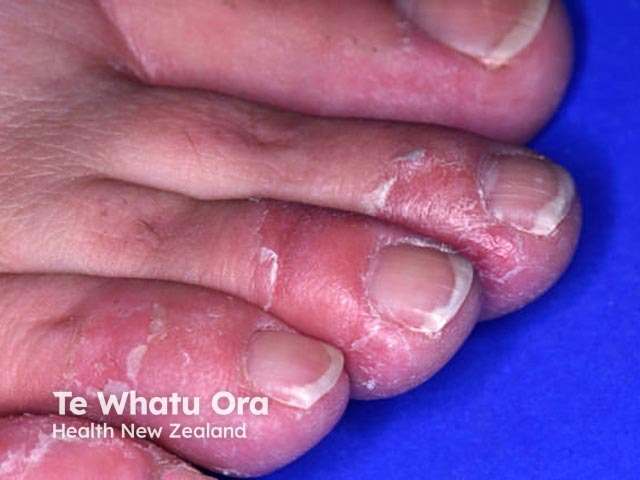
Keratolytic winter erythema
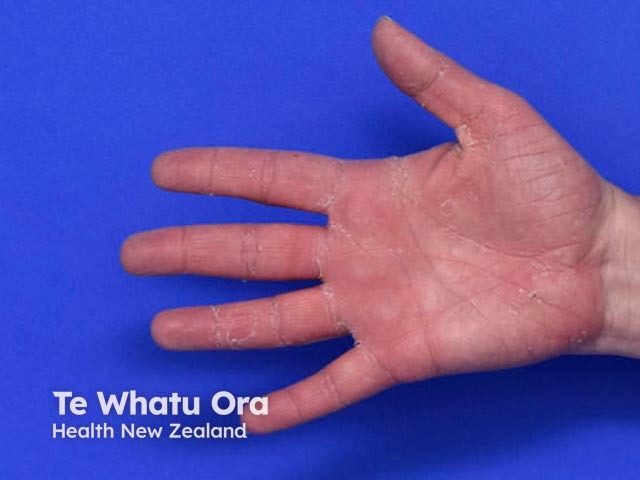
Keratolytic winter erythema
See more images of keratolytic winter erythema.
The prevalence of keratolytic winter erythema is estimated at 1 in 7,200 white Afrikaans speakers [1]. It is inherited in a monogenic autosomal dominant pattern with high penetrance but variable expressivity. It is usually diagnosed in childhood or early adult life.
Genealogical studies of affected South African families have identified a common ancestor, Captain François Renier Duminy, an 18th century Frenchman who settled in the Cape of Good Hope [1]. Sporadic cases have also been reported.
The keratolytic winter erythema gene locus has been mapped to chromosome 8p23.1–p22 [1]. A recent study of the human genome has proposed that the erythema results from an accidental duplication of an enhancer region (a part of the DNA that makes its adjacent gene more likely to be "read" for transcription) next to CTSB, a gene important in keratinocyte differentiation and desquamation [6].
Varying triggering environmental factors may disrupt the balance of CTSB and its regulatory factors to increase levels of cathepsin B, a lysosomal protease in the epidermis, and trigger apoptosis (body-mediated cell death) [3].
Keratolytic winter erythema usually presents between infancy and early adulthood, and it continues with an intermittent and recurrent pattern [2]. It ranges in severity with cyclical skin peeling and underlying erythema affecting the palms of the hands and the soles of the feet [3].
Some patients with keratolytic winter erythema also develop annular erythema on the limbs, buttocks, or trunk; there has been one reported case of facial involvement [4].
Aggravating factors may include:
Keratolytic winter erythema can improve in summer and during pregnancy [3].
Active flares of keratolytic winter erythema can be disabling in severe cases.
The diagnosis of keratolytic winter erythema may be evident clinically and may be supported by a positive family history.
On skin biopsy, keratolytic winter erythema shows characteristic histopathology with basal keratinocyte proliferation and defective layers of the stratum corneum [5].
Depending on the phase of the lesion, the differential diagnosis of keratolytic winter erythema may include [6]:
There is currently no established effective treatment for keratolytic winter erythema. Topical keratolytics, retinoids and steroids may aggravate keratolytic winter erythema [6]. Photodynamic therapy has shown disease-modifying results in one patient [5].
Keratolytic winter erythema typically improves or even clears during the summer months [4]. It also tends to improve with age and there may be only minimal scaling in the creases in adulthood [1]. In some severely affected individuals, it will persist [2].