Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Multicentric reticulohistiocytosis — extra information
Multicentric reticulohistiocytosis
Author: Dr Lauren Thomas, RMO, Royal Darwin Hospital, Darwin, NT, Australia. DermNet Editor in Chief: Adjunct A/Prof. Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy edited by Gus Mitchell. October 2019.
Introduction Demographics Causes Clinical features Diagnosis Treatment Outcome
What is multicentric reticulohistiocytosis?
Multicentric reticulohistiocytosis is a very rare multisystem arthropathic form of reticulocytosis. Reticulohistiocytoses are a type of non-Langerhans cell histiocytosis. Multicentric reticulohistiocytosis is characterised by skin and mucosal lesions, and arthritis [1].
Multicentric reticulohistiocytosis is referred to as lipoid dermatoarthritis, lipoid rheumatism, and giant cell reticulohistiocytosis.
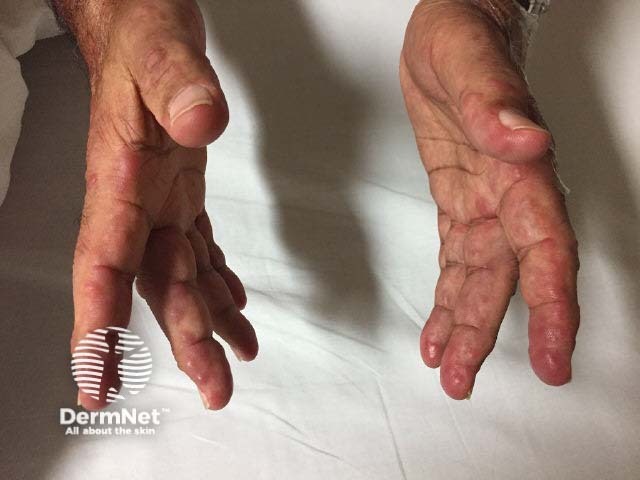
Multicentric histiocytosis
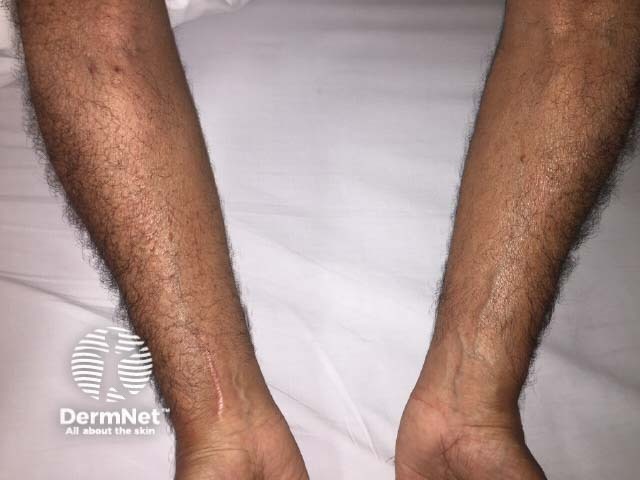
Multicentric histiocytosis
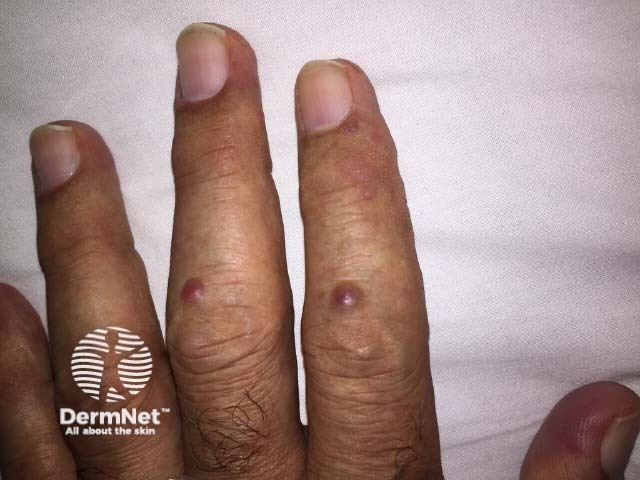
Multicentric histiocytosis
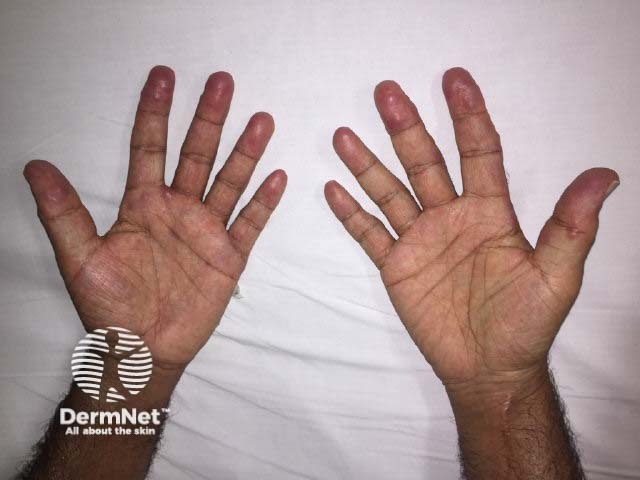
Multicentric histiocytosis
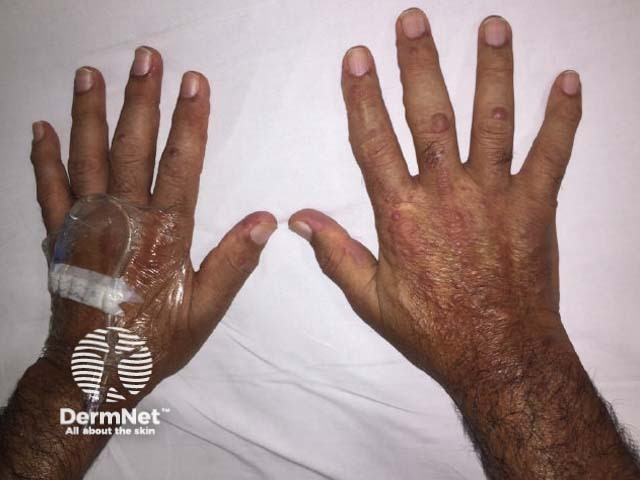
Multicentric histiocytosis
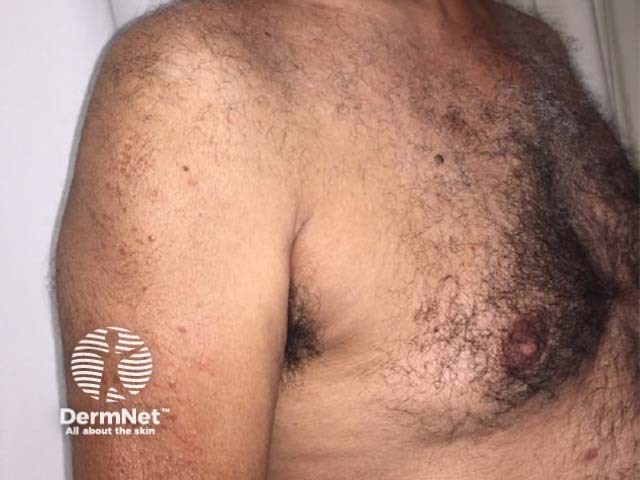
Multicentric histiocytosis
Who gets multicentric reticulohistiocytosis?
Multicentric reticulohistiocytosis is more common in women than men, with a ratio of 3:1 [1]. The mean age of people affected by multicentric reticulohistiocytosis is 47 years (age range 8-74 years) [5].
In approximately 1 in 4 cases, multicentric reticulohistiocytosis is associated with an internal malignancy [1]. The most common malignancies associated with multicentric reticulohistiocytosis are carcinomas of the lung, stomach, breast, cervix, colon, and ovary.
What causes multicentric reticulohistiocytosis?
The cause of multicentric reticulohistiocytosis is unknown. Molecular abnormalities have been reported in the MAP2K1, TT2 and other pathways [5]. Whether multicentric reticulohistiocytosis is a true paraneoplastic disorder is controversial.
- No consistent type of cancer has been associated with multicentric reticulohistiocytosis.
- Because multicentric reticulohistiocytosis is very rare, the association with cancer may be coincidental.
- A correlation between the removal of cancer and the disappearance or improvement of multicentric reticulohistiocytosis has not been established.
Multicentric reticulohistiocytosis is also associated with:
- Vasculitis
- Autoimmune diseases including Sjögren syndrome and primary biliary cirrhosis [3]
- Hyperlipidaemia.
What are the clinical features of multicentric reticulohistiocytosis?
Multicentric reticulohistiocytosis results in papules, nodules, and severe and rapidly destructive arthritis. It can involve the bones, tendons, muscles, joints, and solitary organs (eg, thyroid, eye, lung, kidney, and liver) [1].
- In half of the patients, the first sign of the disease is arthritis.
- In one-quarter, papules and nodules are the first sign.
- The remainder develops skin and joint manifestations at the same time.
Arthritis
Arthritis most commonly involves the fingers, hands, knees, and shoulders, but any joint can be affected. This is a symmetrical progressive arthritis that can be associated with joint stiffness and swelling. The symptoms of arthritis may wax and wane, but can rapidly become severe and lead to joint destruction and deformity in about 45% of patients. Importantly, this can be asymptomatic at the time of presentation, and hence needs to be looked for on radiology.
Cutaneous features
Multicentric reticulohistiocytosis skin lesions most commonly occur on the upper half of the body, especially the face, ears, mucosal surfaces (lips, tongue, gums, nostrils, throat, eyelids), hands, and forearms.
- There are yellowish or red-brown papules and nodules ranging from 1–2 mm to several centimetres in diameter.
- Lesions arise in isolation or in clusters or crops with a cobblestone appearance.
- Mucosal lesions are present in approximately 50% of cases.
- The skin lesions may cause destruction of cartilage around the ears and nose.
- Multiple tiny lumps around the nails may occur, known as ‘coral-beading’.
- Lesions are usually asymptomatic, but one-third of patients complain of pruritus [2].
Dermatoscopy of multiple papules in one patient has been reported. All showed the 'setting-sun sign' of a yellowish hue centrally and a pink-orange rim. Most also had brown reticular structures and less commonly a central white scar-like change were seen [6].
Multicentric reticulohistiocytosis can be accompanied by systemic symptoms, including:
- Weight loss
- Fever
- Malaise
- Myalgia
- Dysphagia
- Lymphadenopathy [2].
How is multicentric reticulohistiocytosis diagnosed?
Reticulocytosis is diagnosed from the characteristic histology of a skin biopsy, showing:
- Multiple multinucleated giant cells
- Histiocytes with eosinophilic cytoplasm and a ground-glass appearance [1]
- Positive immunohistochemical staining for histiocytes of a monocyte-macrophage origin and an abundance of cytokines, including tumour necrosis factor-alpha (TNF-α).
The specific diagnosis of multicentric reticulohistiocytosis is made when radiology shows the typical erosive arthritis especially in the hands.
Histiocytes and multinucleated giant cells can also be found in joints and occasionally in internal organs.
Blood tests are not diagnostic; they may include routine haematological investigations, lipid profile, thyroid profile, C-reactive protein (CRP), and rheumatoid factor. Most patients with multicentric reticulohistiocytosis have mild anaemia; 30–60% of patients have hyperlipidaemia and an elevated erythrocyte sedimentation rate (ESR)/C-reactive protein (CRP) [2,3].
A positive tuberculin skin test is found in 12–50% of patients with multicentric reticulohistiocytosis and is more common where tuberculosis is endemic [3].
Once the diagnosis of multicentric reticulohistiocytosis has been made, a thorough history and physical examination should be undertaken with age-appropriate screening tests for malignancy, including a chest x-ray and ultrasound scan of the abdomen/pelvis [1].
What is the treatment for multicentric reticulohistiocytosis?
There is no specific or curative treatment for multicentric reticulohistiocytosis. The following have been reported to be helpful:
- Methotrexate
- Short courses of systemic corticosteroids (oral prednisolone/prednisone)
- Ciclosporin
- Azathioprine
- Cyclophosphamide
- Leflunomide
- Etanercept [4].
What is the outcome for multicentric reticulohistiocytosis?
In many patients, multicentric reticulocytosis can go into remission after an average course of 8 years; however, by this time considerable joint destruction may have occurred. Arthritis mutilans may develop in 50% of cases [2]. Patients are left with crippling, deformed joints and a disfigured facial appearance.
References
- Shah SP, Shah AM, Prajapati SM, Bilimoria FE. Multicentric reticulohistiocytosis. Indian Dermatol Online J. 2011 Jul;2(2):85-7. doi: 10.4103/2229-5178.85998. PMID: 23130232; PMCID: PMC3481828. PubMed Central
- Amin BP M. Busam K. Dermatopathology. 1st ed: Saunders; 2009. Available at: www.sciencedirect.com/topics/medicine-and-dentistry/multicentric-reticulohistiocytosis (accessed 30 October, 2019)
- Saba R, Kwatra SG, Upadhyay B, Mirrakhimov AE, Khan FN. Multicentric reticulohistiocytosis presenting with papulonodular skin lesions and arthritis mutilans. Case Rep Rheumatol. 2013;2013:201563. doi: 10.1155/2013/201563. Epub 2013 Mar 10. PMID: 23555066; PMCID: PMC3608314. PubMed
- Kovach BT, Calamia KT, Walsh JS, Ginsburg WW. Treatment of multicentric reticulohistiocytosis with etanercept. Arch Dermatol. 2004 Aug;140(8):919-21. doi: 10.1001/archderm.140.8.919. PMID: 15313806. PubMed
- Bonometti A, Berti E; for Associazione Italiana Ricerca Istiocitosi ONLUS. Reticulohistiocytoses: a revision of the full spectrum. J Eur Acad Dermatol Venereol 2020. DOI: 10.1111/jdv.16214. PubMed
- Kaçar N, Tasli L, Argenziano G, Demirkan N. Reticulohistiocytosis: different dermatoscopic faces and a good response to methotrexate treatment. Clin Exp Dermatol 2010; 35: e120–2. DOI: 10.1111/j.1365-2230.2009.03738.x. PubMed
On DermNet
- Reticulohistiocytoma pathology
- Langerhans cell histiocytosis
- Non-Langerhans cell histiocytosis
- Skin signs and systemic disease
