Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Authors: Elena Redl, Medical Student, Vienna, Austria; Dr Martin Keefe, Assistant Editor and Dermatologist, DermNet, New Zealand. Copy edited by Gus Mitchell. February 2022
Introduction
Demographics
Causes
Clinical features
Variation in skin types
Complications
Diagnosis
Differential diagnoses
Treatment
Outcome
Pretibial pruritic papular dermatitis (PPPD) is a distinctive, itchy, papular dermatosis seen over the shins, first described in 2006.
Although the cause is uncertain, it is thought to be a reaction to chronic rubbing. It appears to be different to other dermatoses that result from persistent rubbing or scratching of the skin such as lichen simplex chronicus and prurigo nodularis.
PPPD seems uncommon but the incidence is unknown. Furthermore, as it has only been described relatively recently and can be confused with other conditions in which rubbing or scratching is a prominent feature, it may be more common than assumed. It is seen mainly in adult females.
PPPD is likely to result from persistent rubbing and gentle scratching of the skin of the front of the lower legs. The cause of the pruritus that leads to rubbing or scratching is unclear, however, cutaneous xerosis, psychological stress, and contact with irritants may be contributing factors.
Factors that lead to PPPD, other than itch/rubbing-related conditions, such as lichen simplex chronicus or nodular prurigo, are unclear but may involve the location of the dermatosis and the nature of the rubbing.
PPPD is clinically defined by multiple, uni- or bilateral, discrete, smooth flesh-coloured to erythematous papules located on the anterior surface of the lower legs.
Commonly, the papules coalesce, resulting in a cobblestone appearance. Larger plaques, erythema, and epidermal erosions may be seen.
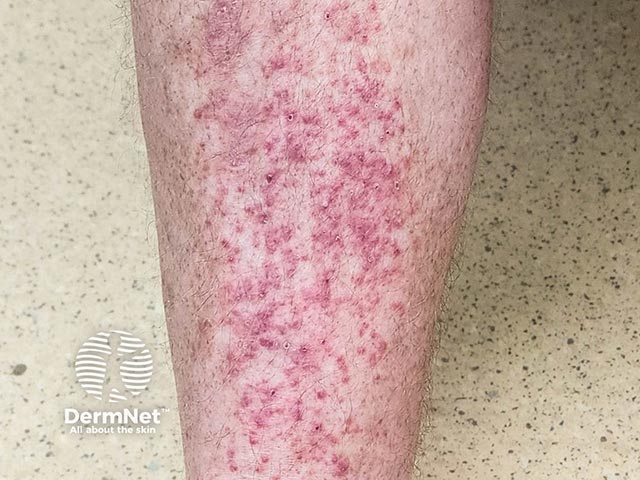
Itchy erythematous and purpuric hyperkeratotic papules on the shin in PPPD (PPPD-patient1)
There is no available data on the epidemiology or the clinical features in different ethnic groups.
No specific complications have been reported.
PPPD is diagnosed clinically, based on the history and clinical features.
Dermoscopy may be helpful: dermoscopic features of PPPD include dotted or globular vessels on a pinkish-whitish background that are often accompanied by a peripheral whitish collarette of scale with a petaloid appearance.
A skin biopsy will confirm the diagnosis and exclude other pretibial dermatoses. Histology shows orthokeratosis in combination with papillary dermal fibrosis, thickened dermal papillae, stellate and multinucleated fibroblasts, spindle cells, and eosinophils.
Other features have been described, including weak CD30 expression and lymphocyte atypia which may lead to confusion with lymphomatoid papulosis.
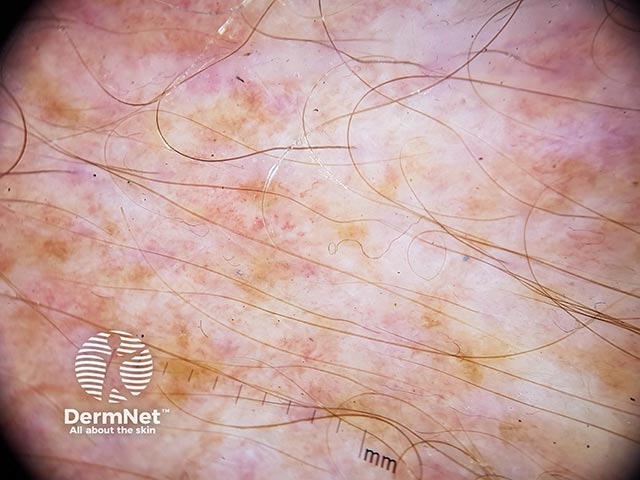
Dermoscopy of pretibial pruritic papular dermatitis (PPPD-patient1)
The differential diagnosis of PPPD includes dermatoses with similar clinical features and other dermatoses which result from rubbing and scratching.
Dermatoses with similar clinical features include:
Other dermatoses resulting from rubbing and scratching, but which can be distinguished clinically and histologically, include:
Treatment of PPPD includes:
PPPD runs a chronic course but remains limited to the anterior surface of the lower legs. Response to treatment is variable. Topical corticosteroids and other treatments may need to be used for a prolonged period and relapse is common.