Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Last Reviewed: February, 2026
Author: Dr. Rui Baptista Gonçalves, Leeds Teaching Hospitals, United Kingdom. Copy edited by Gus Mitchell. July 2022
Introduction
Demographics
Causes
Clinical features
Variation in skin types
Complications
Diagnosis
Differential diagnoses
Treatment
Outcome
Nodular prurigo (NP) or prurigo nodularis is a chronic skin condition characterised by very itchy firm lumps. It can appear anywhere on the body but is most common on the arms, legs, back, and torso, in a symmetrical distribution.
It is the most severe form of prurigo and thus can be difficult to treat.
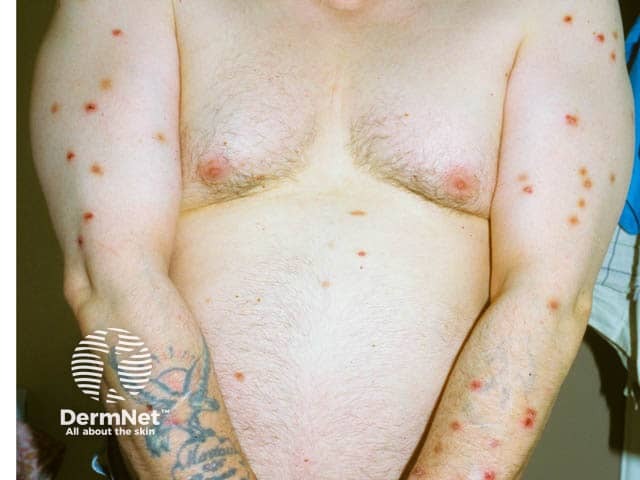
Excoriated papules on the arms in nodular prurigo
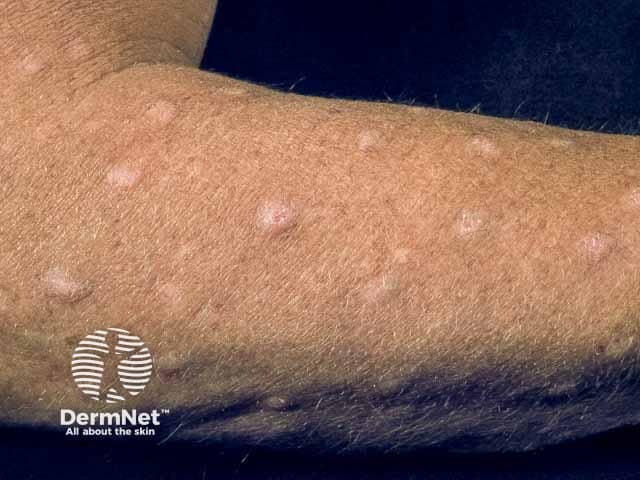
Nodular prurigo on the arms
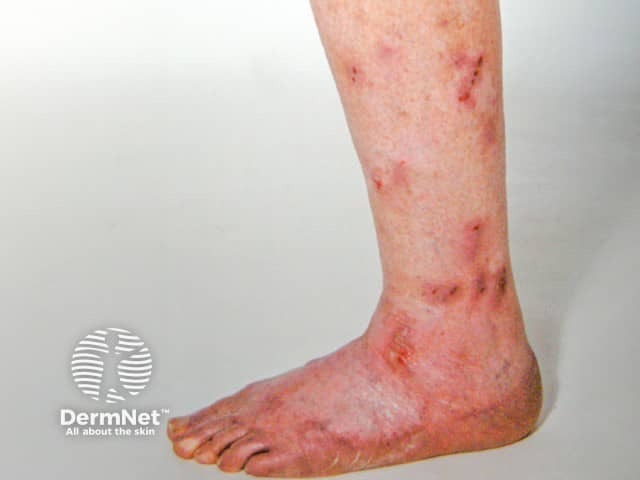
Excoriated prurigo lesions on the legs
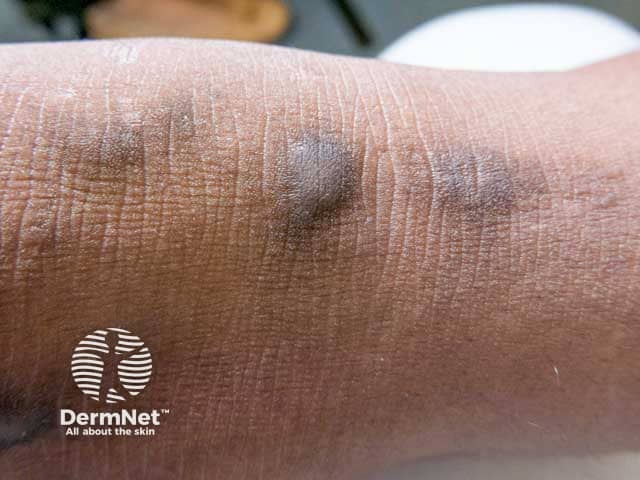
Pigmentation of prurigo nodules in skin of colour (NP-patient3)
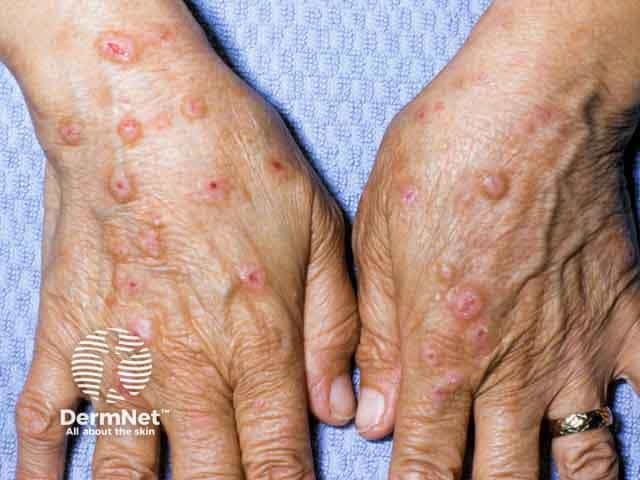
Prurigo on the dorsal hands in skin of colour
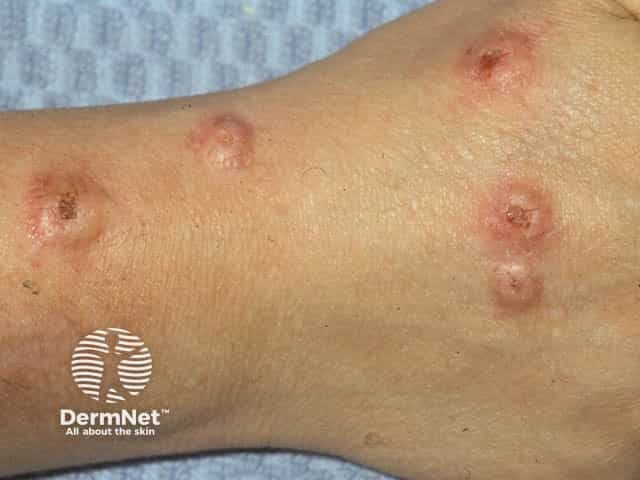
Dome shaped prurigo on the ankles
Nodular prurigo can affect both sexes and people of all ages but is more common in older adults.
There is also an association with:
The exact cause of prurigo nodularis remains unknown. It is thought to relate to a dysregulation of the nerves as skin biopsies have shown a greater number of nerve cells in the dermis but a reduced amount in the epidermis. There is also an increased number of Merkel cells in the epidermis and the papillary layer of the dermis, as well as more neutrophils and mast cells, thus more cytokine release; which may explain the severe itchiness.
The itchiness may start as a result of an insect bite, stress, dermatitis, or another underlying skin or systemic condition. There is also an association with brachioradial pruritus, which results from traction of spinal nerves in the neck. Scratching will thicken and inflame skin, worsening the condition.
Nodular prurigo can vary in severity, from a few to hundreds of lesions of varying size.
Initially, the rash:
Scratching leads to:
In darker skin, the lesions tend to be firmer, larger, and darker, similar to bumps on the skin that leave dark spots when healing, which can take longer to fade than in fairer skin types.
Aside from its chronicity, the main complications are:
Prurigo nodularis is most often diagnosed clinically, however, investigations are often useful particularly to ascertain the cause. These include:
Unfortunately, there is no cure and treatment can be challenging. Therapy must be multimodal, also including treatment of any identified underlying condition.
Common treatment options include:
Other treatment options include:
It is crucial that anyone suffering from NP stops scratching the lesions, as this can make the condition worse. Strategies that can help include:
Prurigo nodularis can be difficult to treat, taking months or even years to clear and may not resolve completely, often rendering it a chronic condition. It is important that patients follow their dermatologist’s recommendations and report any issues with the treatment so that different approaches can be used.