Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Authors: Dr Nicholas Van Rooij, MD, Dermatology PHO, The Royal Brisbane and Women’s Hospital, Australia. March 2022. Dr Ritva Vyas, Dermatology Registrar, Waikato Hospital New Zealand, 2010. Copy edited by Gus Mitchell.
Introduction
Demographics
Causes
Clinical features
Variation in skin types
Complications
Diagnosis
Differential diagnoses
Treatment
Outcome
Uraemic pruritus (uremic pruritus) is also called chronic kidney disease-associated pruritus (CKD-associated pruritus). Uraemia refers to excessive urea in the blood and occurs when the kidneys stop working (renal failure). Pruritus (itch) is a common problem for patients with chronic renal failure or end-stage renal disease.
It affects about one-third of patients on dialysis and is more common with haemodialysis than continuous ambulatory peritoneal dialysis (CAPD).
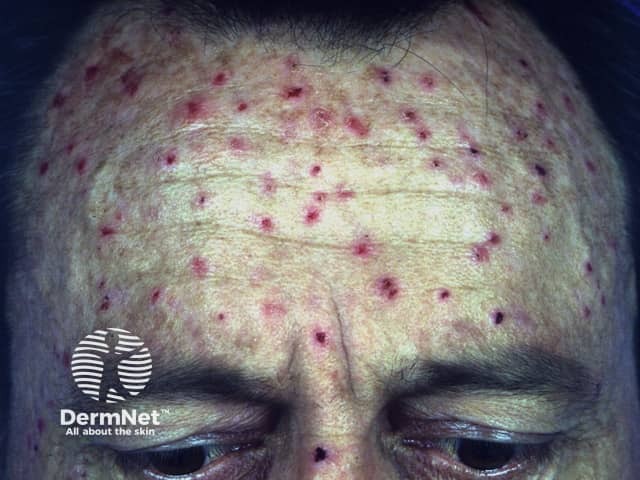
Uraemic pruritus (renal itch)
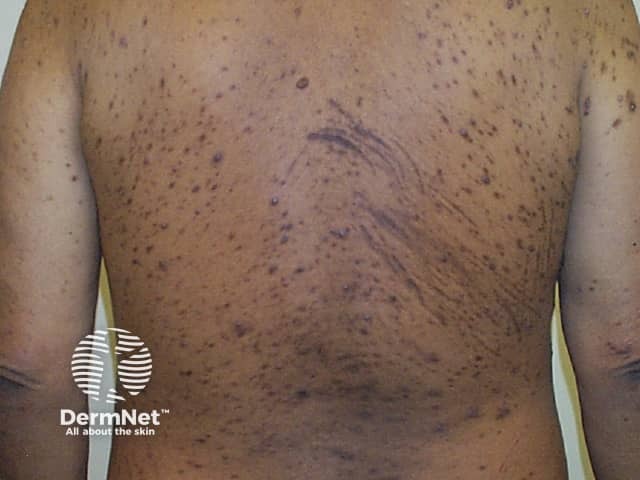
Uraemic pruritus (renal itch)
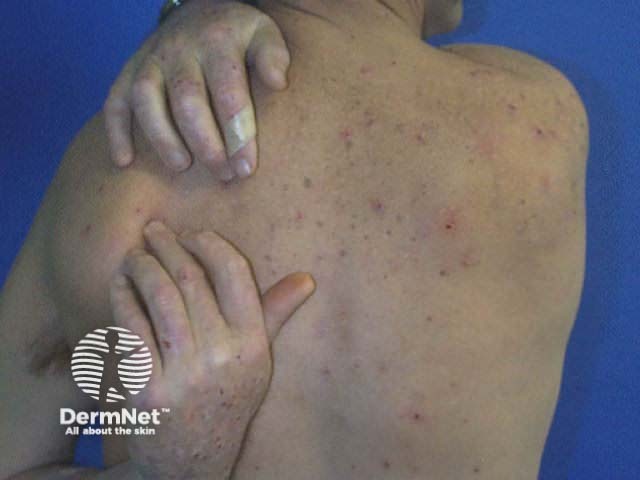
Pruritus
The prevalence rates of uremic pruritus are between 20–50% in those with chronic kidney disease, however, the reported rates appear lower in children at approximately 9%.
Uraemic pruritus is not associated with sex, age, ethnicity, duration of dialysis, or cause of renal failure. Pruritus does not arise when uraemia is due to acute renal failure.
Uraemic pruritus is thought to be due to a combination of factors including:
Some patients develop acquired reactive perforating collagenosis.
Itch in uremic pruritus most commonly affects the back, however, it can also involve the arms, head, and abdomen. Generalized pruritus is also noted in a proportion of affected patients (20-50%).
Other characteristic features include:
Uraemic pruritus can be associated with several non-specific cutaneous features resulting from repetitive scratching.
These may include:
Clinical presentation remains consistent across different skin types and ethnicities.
Scratching may lead to impetigo (skin infection), prurigo (papules) and chronic, lichenified dermatitis/eczema.
Uraemic pruritus can be very unpleasant; about half of affected individuals become agitated or depressed. Uraemic pruritus in haemodialysis patients is associated with a 17% increase in mortality.
Uraemic pruritus is largely a clinical diagnosis, based on a history of chronic kidney disease and onset of symptoms. The commencement of pruritus in patients coinciding with commencement of dialysis, persistence of symptoms, or elevated urea blood levels is consistent with a diagnosis of uraemic pruritus.
Laboratory investigations can help to confirm a diagnosis, investigations may include:
Other dermatological and general metabolic causes of itch may need to be excluded e.g. eczema, scabies, drug-induced reactions, iron deficiency, and thyroid disease.
The first step in treatment is optimising dialysis efficacy. It is also important to attempt to reduce serum parathyroid hormone in order to normalise calcium/phosphorus levels. These methods aim to reduce the underlying cause of itch.
Supportive general measures to improve symptoms include:
Topical preparations for itch are generally sufficient to help improve symptoms, these may include:
UVB phototherapy is the mainstay of treatment for severe uraemic pruritus that has not responded to conventional treatments.
Difelikefalin received FDA approval in 2021 for the treatment of uraemic pruritus in patients undergoing haemodialysis. Nalfurafine, another KOR agonist, has been approved in Japan since 2009 for this indication.
Other treatments that have been reported to help some individuals, include:
Oral antihistamines and systemic steroids are generally not effective.
Uraemic pruritus can be difficult to alleviate and patients with pruritus often have decreased quality of life such as poor sleep and depression. In cohort studies, it is associated as an independent predictor of morbidity, mortality, and leads to other poor patient outcomes. One study showed moderate to severe pruritus was associated with a 17% increase in mortality rate.
Kidney transplantation is the definitive treatment and usually results in resolution of uraemic pruritus.