Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Authors: Vanessa Ngan, Staff Writer, 2005; Updated: Dr Aswan Tai, Junior Doctor, Peter MacCallum Cancer Centre, Melbourne, Australia; Dr Sarah Smithson, Dermatologist, Skin Health Institute, Melbourne, Australia. Copy edited by Gus Mitchell. September 2021
Introduction Demographics Causes Clinical features Variation in skin types Complications Diagnosis Differential diagnoses Treatment Outcome
Reactive perforating collagenosis is the most common type of primary perforating dermatosis. It is characterised by the transepithelial elimination of collagen from the dermis through the epidermis to the skin surface.
The pathogenesis of reactive perforating collagenosis is unclear.
The inherited form appears to be due to a genetic abnormality in collagen causing focal damage and extrusion through the epidermis. Cold weather and skin trauma typically trigger or aggravate the skin lesions.
Microvascular insufficiency and elevated fibronectin levels in plasma, as seen with diabetes and renal failure, may play a role in the acquired form. Another theory suggests microdeposition of substances and abnormal glycosylation of collagen I and III in diabetes alter collagen fibres.
Superficial trauma, such as scratching, and cold leads to necrobiosis and epidermal thinning in susceptible patients.
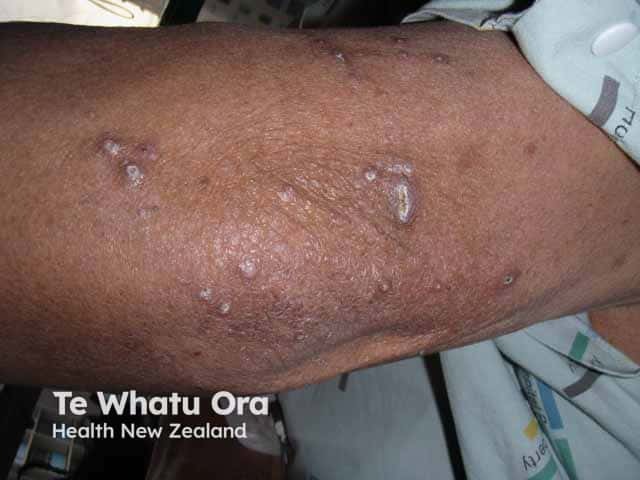
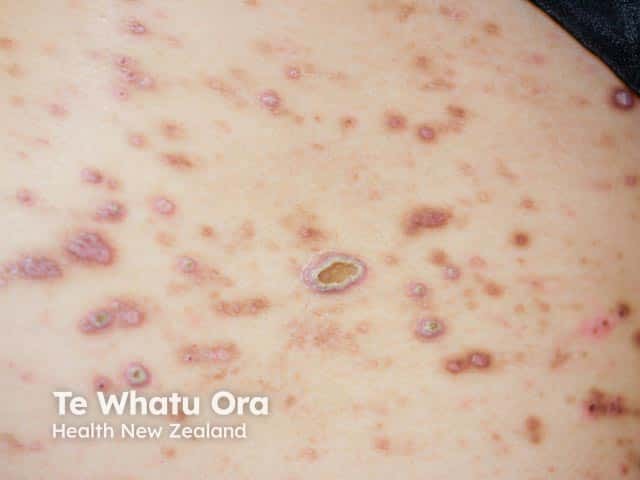
Reactive perforating collagenosis is a papulonodular mucocutaneous disorder with adherent keratotic plugs and crusts.
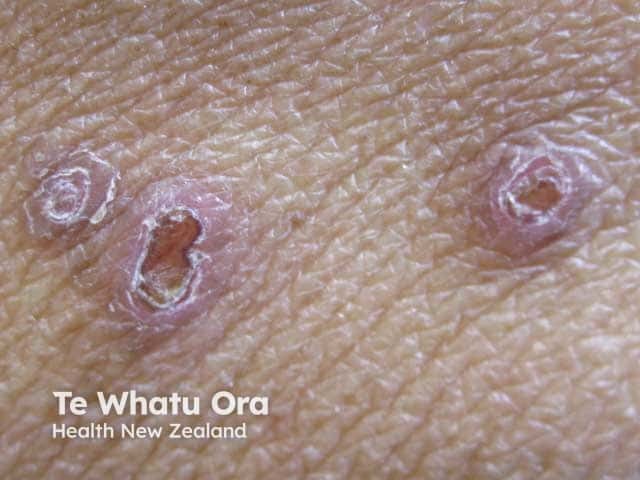
Nodules with keratotic crust
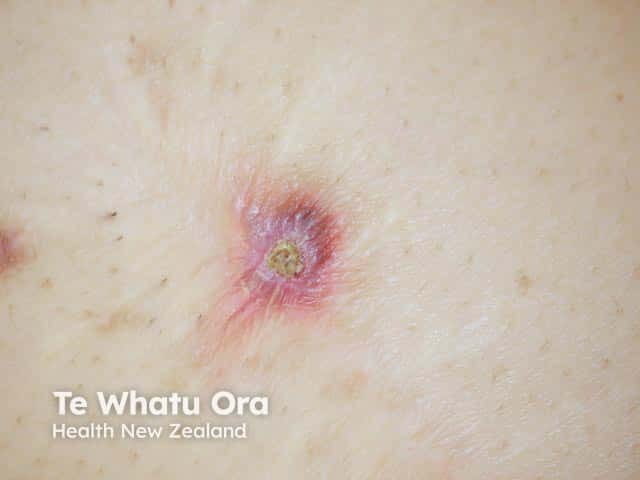
Nodule with keratotic plug and erythematous halo
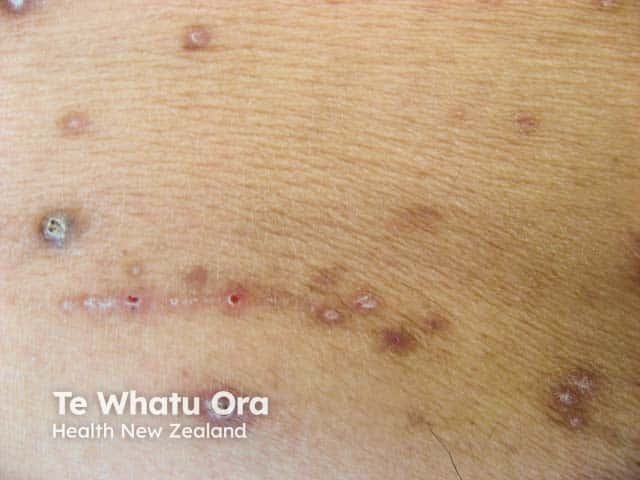
Keratotic papules with koebnerisation
The dermoscopy features of reactive perforating collagenosis are characteristic and consistent:
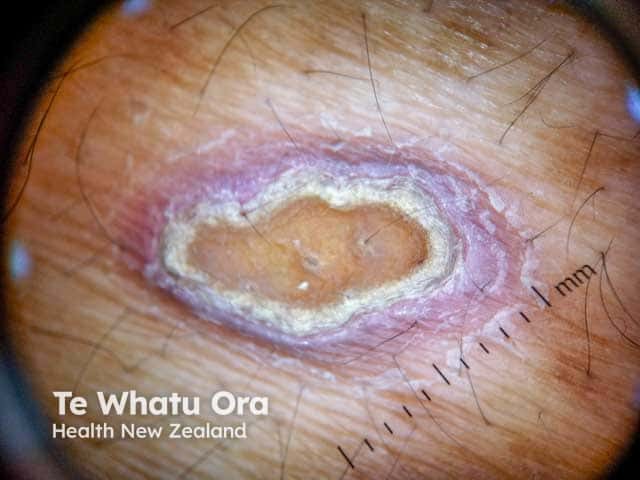
Reactive perforating collagenosis: dermoscopy
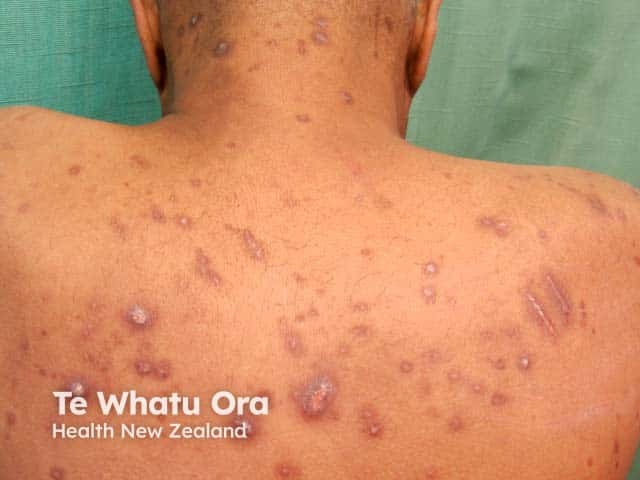
Reactive perforating collagenosis in skin of colour is associated with hyperpigmentation:
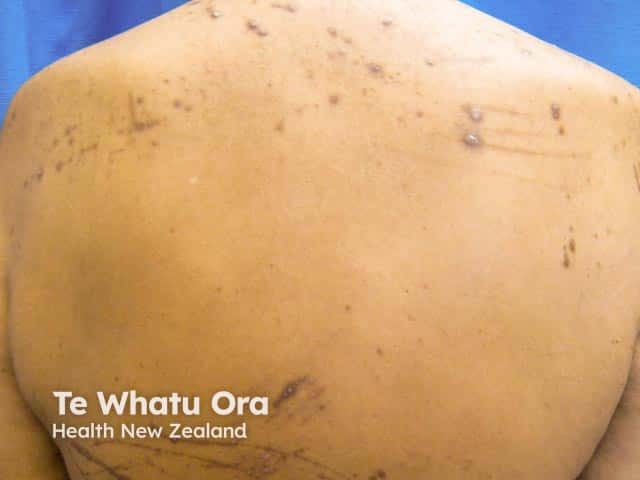
Hyperpigmented scratch marks
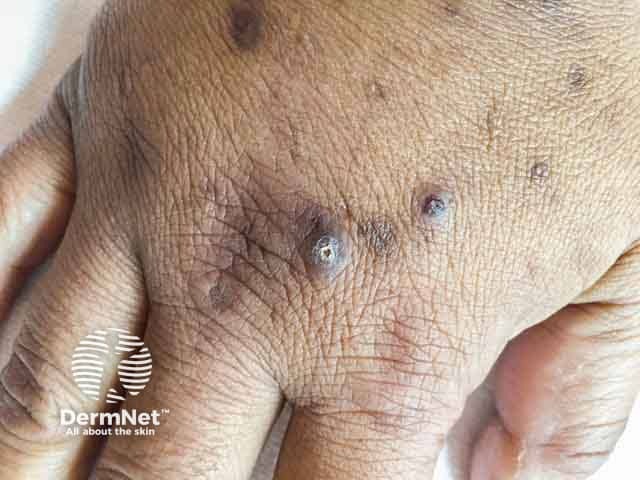
Hyperpigmented keratotic papules
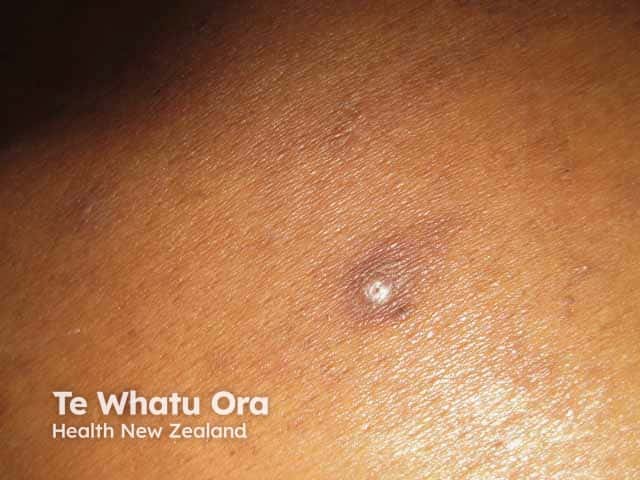
Hyperpigmentation around keratotic papule
Reactive perforating collagenosis can usually be diagnosed on its distinct clinical features and associated conditions, and confirmed on dermoscopy.
Multiple skin biopsies examined with multiple levels may be required to find the diagnostic histology [see Reactive perforating collagenosis pathology].
The main aim of treatment for reactive perforating collagenosis is to reduce itch and minimise skin trauma:
Reactive perforating collagenosis remains confined to the skin.
Familial reactive perforating collagenosis is a lifelong condition with lesions becoming larger and more numerous with age.
Individual lesions in both the familial and acquired forms are self-healing but often recur.