Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Tim Aung, Primary Care Practitioner, Brisbane & Logan, Queensland, Australia. DermNet Editor in Chief: Adjunct A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy edited by Gus Mitchell/Maria McGivern. April 2019.
Introduction
Demographics
Causes
Drugs that cause pruritus
Treatment
Pruritus is the medical name for itching. Drug-induced pruritus is an itch caused or triggered by medication. There are various itchy drug eruptions, but generally, the term ‘drug-induced pruritus’ implies that no primary rash is present — just scratch marks.
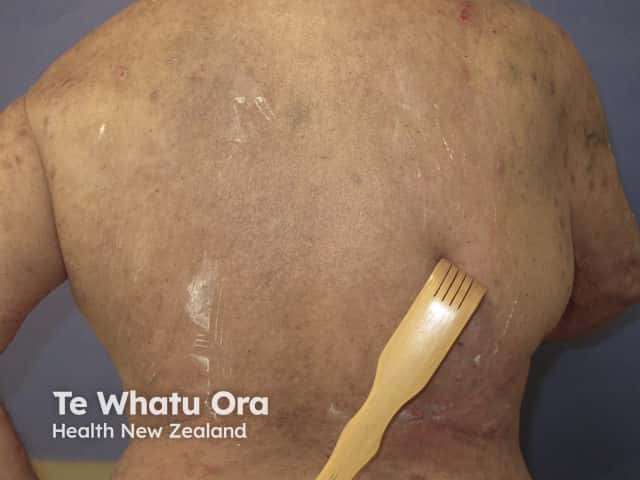
Scratching with back scratcher
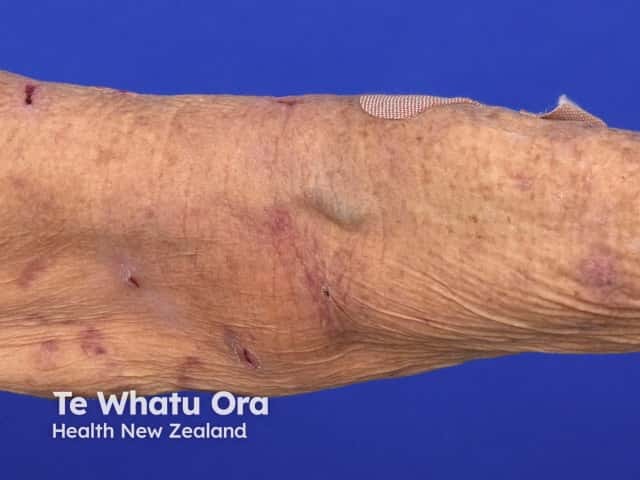
Pruritus
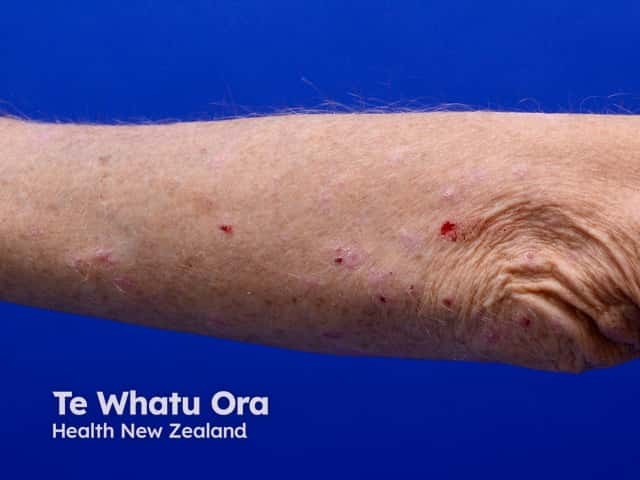
Scratch marks
The epidemiology of drug-induced pruritus is unknown. Generally, adverse drug reactions are more common in older patients and in patients taking multiple medicines.
The cause of drug-induced pruritus is often unknown and depends on the drug. It may involve:
The most commonly reported drugs to cause pruritus are opioids (especially during spinal anaesthesia), chemotherapeutic agents, and chloroquine (affecting 60–70% of black Africans prescribed this medicine).
The main groups of drugs that cause pruritus through various mechanisms are listed below.
Antimicrobials and antibiotics that cause pruritus include:
Cardiovascular medicines that can cause pruritus include:
Metabolic medicines that can cause pruritus include:
Neuroleptic and psychotropic drugs (used to treat psychosis) that can cause pruritus include:
Opioids and analgesics that can cause pruritus include:
Steroids and hormones that can cause pruritus include:
Chemotherapeutic and biological agents that can cause pruritus include:
Other drugs that can cause pruritus include:
The cessation of the causative drug is an immediate priority [1,4–6]. Treatment depends on how the causative drug triggered the itching and its severity.