Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Avee Naidoo, Medical Student, Faculty of Medicine, University of Toronto, Toronto, Canada. DermNet Editor in Chief: Adjunct A/Prof Dr Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy edited by Gus Mitchell/Maria McGivern. September 2019.
Introduction
Demographics
Causes
Clinical features
Complications
Diagnosis
Differential diagnoses
Methods of diagnosis
Treatment
Outcome
Chronic pruritus of unknown origin is defined as an itch lasting longer than 6 weeks in the absence of a known cause [1]. It is also called chronic idiopathic pruritus and generalised pruritus of unknown origin.
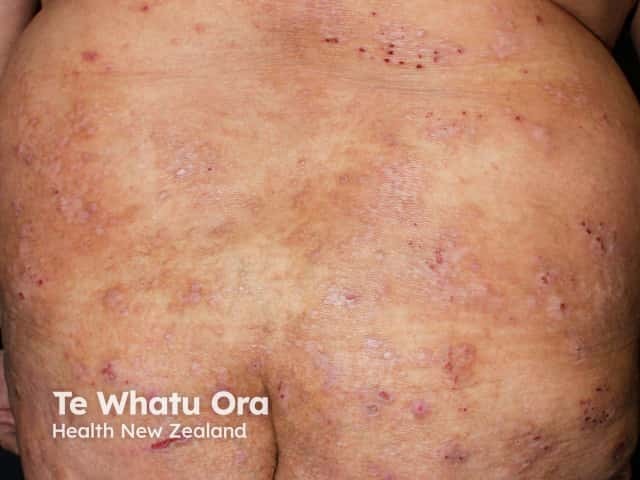
Scratching related to dermatitis
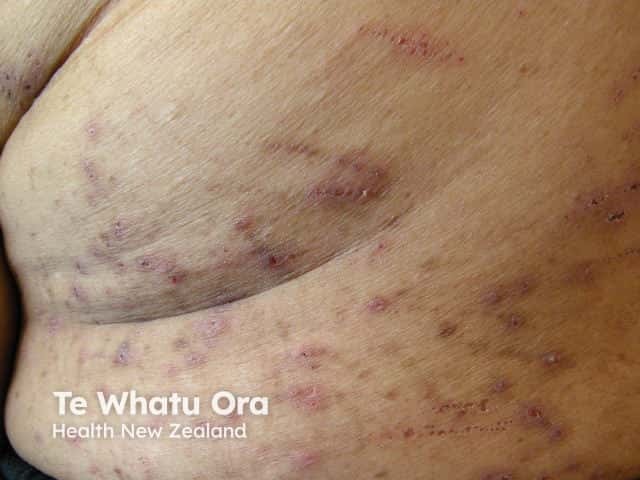
Scratching in uraemic pruritus
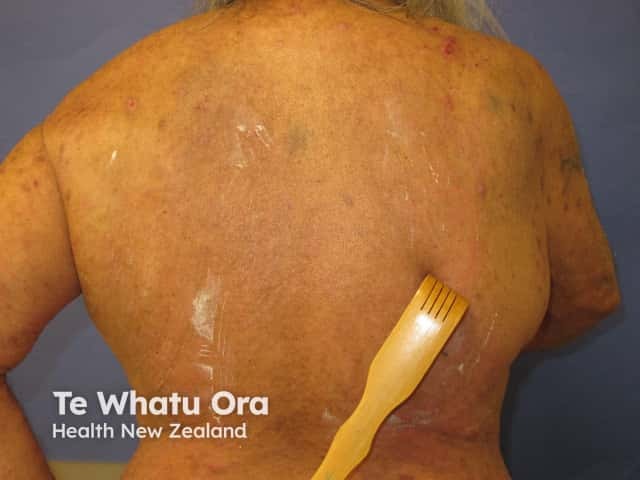
Back scratcher for pruritus
No detailed studies on the prevalence of chronic pruritus of unknown origin currently exist. However, there is an increased prevalence with older age [2].
By definition, the pathogenesis of chronic pruritus of unknown origin remains unknown [1].
In chronic pruritus of unknown origin, pruritus may be localised or generalised. The skin may appear normal or may be erythematous, rough, or bumpy. Repeated scratching may lead to secondary skin changes, such as lichenification (thickening, hyperpigmentation, and enhanced skin markings), bleeding, or a localised secondary bacterial infection [3].
When chronic pruritus is accompanied by intense scratching, complications may arise. Skin changes include:
Insomnia due to pruritus may greatly affect the quality of life, and lead to worsening of comorbid conditions, including depression and anxiety [3].
Chronic pruritus of unknown origin is a diagnosis of exclusion of any primary dermatological or underlying medical disorders.
Patients with chronic pruritus of unknown origin may present with some positive findings, although these findings will be nonspecific. These include eosinophilia, mild immunoglobulin (Ig)-E elevation (up to 1000 UI/mL), or dermal hypersensitivity. Eosinophils may be observed in the dermis on skin biopsy [1].
Chronic pruritus may be associated with various underlying conditions. The International Forum for the Study of Itch developed a classification system dividing chronic pruritus into six major groups based on its underlying cause: dermatological, systemic, neurological, psychiatric, multifactorial, or of unknown origin [4].
Dermatological causes of pruritus with visible signs include:
Systemic causes of pruritus include:
Neurological diseases that can lead to pruritus include:
Psychiatric diseases that can lead to pruritus include:
Multifactorial reasons for chronic pruritus exist when there is a combination of two or more underlying conditions.
Pruritus of unknown origin is diagnosed when the conditions described above have not been detected.
Factors in the patient’s history that can aid in identifying the cause of chronic pruritus include:
Core laboratory tests that can be done to identify the cause of chronic pruritus include:
Skin biopsy is recommended in any patient who has a primary non-scratched skin lesion in a pruritic site. Biopsy of an excoriation will show secondary change and is not helpful for diagnosis. It should undergo a histopathological examination and direct immunofluorescence.
If malignancy is considered a possible cause, refer for malignancy screening. If the pruritus is present for less than a year, evaluate for Hodgkin lymphoma and liver tumour, especially if fever, malaise, or weight loss are also present [2].
If a neurological cause is suspected, refer for a neurological work-up.
Lifestyle modifications to treat chronic pruritus of unknown origin should include:
Regardless of the origin of the itch, empiric therapies can relieve symptoms. These include:
If no cause is found once the diagnostic work-up of chronic pruritus is completed, treatment with topical and systemic agents is recommended. Often these agents are given for a trial period to determine if they will provide any relief of the itch.
Short-term treatment with topical steroids may be indicated for secondary eczema and to break the itch–scratch cycle. Long-term use of topical steroids is not recommended, as topical corticosteroids lead to skin atrophy and are not effective for pruritus.
Topical calcineurin inhibitors, such as tacrolimus ointment and pimecrolimus cream, have anti-inflammatory properties and exert their effects on cutaneous nerves to suppress itch.
Phototherapy has an antipruritic effect in several itchy skin conditions, including atopic dermatitis, psoriasis, cutaneous T-cell lymphoma, uraemic pruritus, and neuropathic syndromes. It may also be effective in chronic pruritus of unknown origin.
Ciclosporin is an immunosuppressive drug that can control inflammatory skin disease. It is usually ineffective in chronic pruritus of unknown origin.
Gabapentinoids, such as pregabalin and gabapentin, are used for neuropathic pruritic syndromes.
Antidepressants, such as selective serotonin reuptake inhibitors, may control somatoform pruritus and paraneoplastic pruritus. Mirtazapine has been shown to be helpful in chronic spontaneous urticaria and in chronic pruritus of unknown origin.
New agents under investigation for the treatment of chronic pruritus include:
Although chronic pruritus of unknown origin is not life-threatening, it has a significant impact on a patient's quality of life. It often persists for long periods or indefinitely.