Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Lesions (cancerous) Systemic diseases
Authors: Dr Samir Seleq, PGY2 House Officer, Auckland Public Hospital, New Zealand; Chief Editor: Dr Amanda Oakley, Dermatologist, Hamilton, New Zealand; June 2015.
DermNet Update May 2021. Copy edited by Gus Mitchell.
Introduction
Demographics
Causes
Clinical features
Complications
Diagnosis
Differential diagnoses
Treatment
Outcome
Sézary syndrome is a rare leukaemic variant of cutaneous T-cell lymphoma (CTCL) defined by the triad of erythroderma, lymphadenopathy, and atypical malignant Sézary cells in the skin, blood, and lymph nodes.
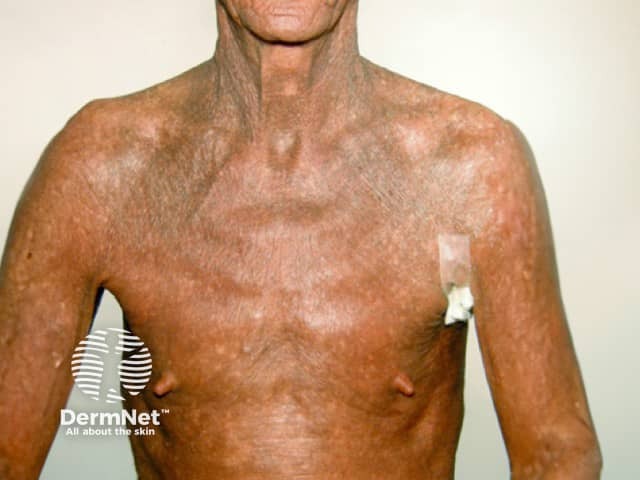
Sézary syndrome
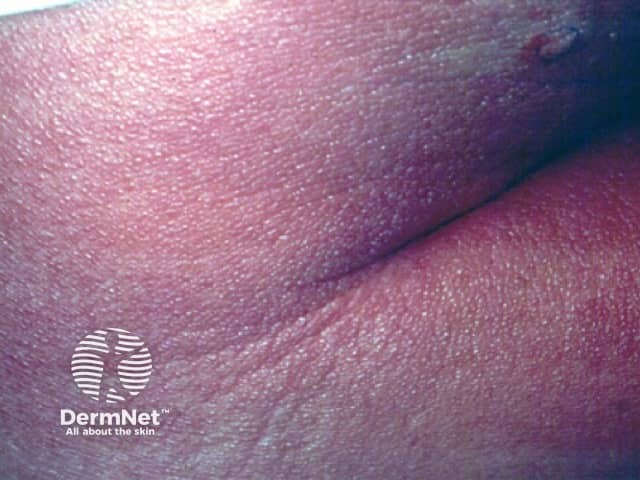
Sézary syndrome
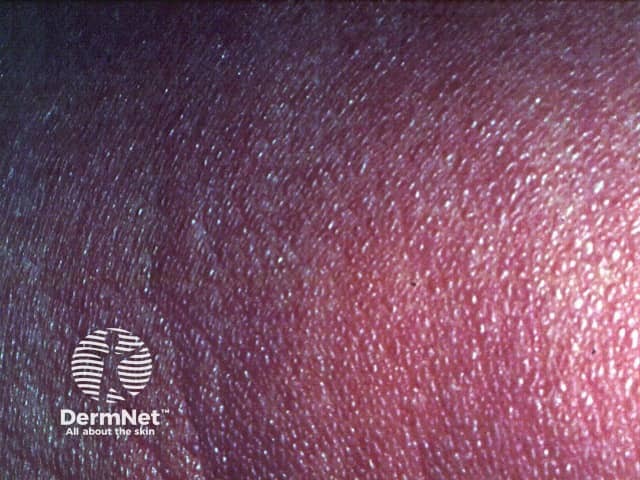
Sézary syndrome typically presents in patients 55–60 years of age, with a male predominance (2:1). The annual incidence is estimated to be 1/10,000, with a higher incidence in black skin over white. Sézary syndrome comprises 3% of all cases of CTCL.
Sézary syndrome arises from a skin tropic memory CD41 T-cell. The role of Staphylococcus aureus superantigen or chronic antigen stimulation has been proposed to lead to clonal expansion of T-cell and malignant transformation.
Sézary cells show diverse and complex chromosomal anomalies affecting many cellular pathways. Many genetic alterations have been identified in recent large-scale surveys, providing information on the molecular pathogenesis and offering new therapeutic targets under investigation.
A viral aetiology has not been identified.
Rare cases of malignancy including Sézary syndrome during treatment with JAK inhibitors have been reported. Causality has not been established and requires further investigation.
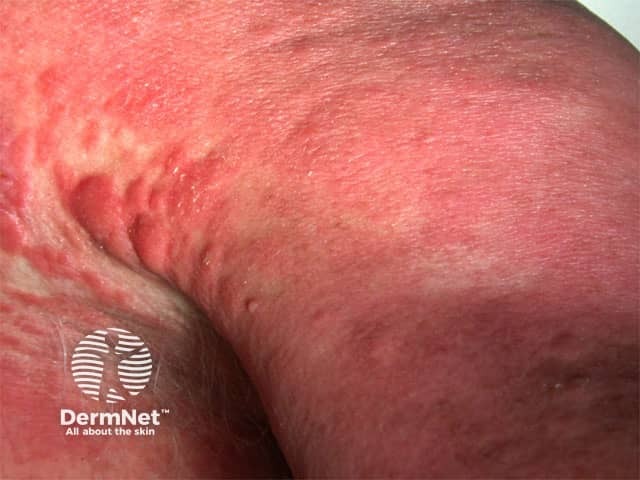
Erythroderma
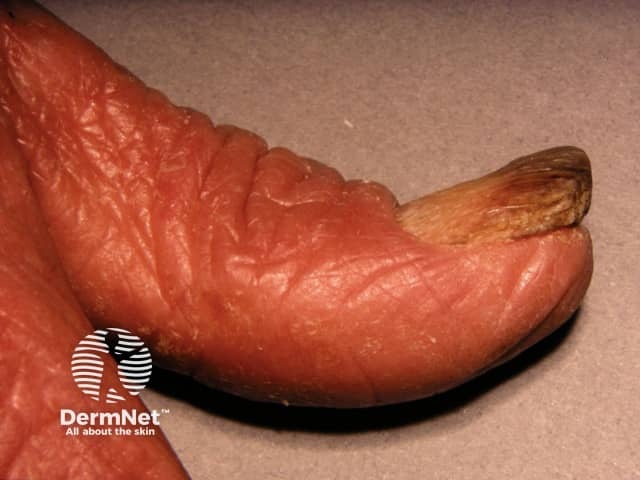
Nail change
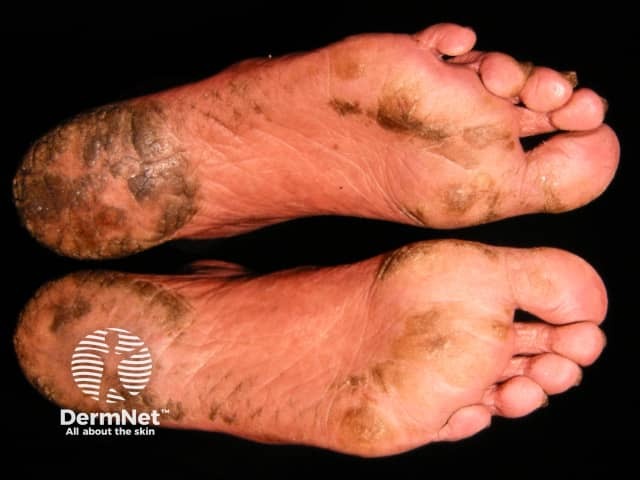
Plantar keratoderma
Sézary syndrome presents at a younger age in black patients than white (53 v 63 years of age) and survival is worse regardless of age and stage at diagnosis.
Sézary syndrome should be considered in the differential diagnosis for any patient presenting with erythroderma.
Imaging may include: chest x-ray, lymph node field ultrasound, CT, MRI, PET.
Staging for MF/SS: TNMB (tumour, node, metastasis, blood) – Sézary syndrome must, by definition, be T4 – erythroderma, N0-3, B2 – Sezary cells >1000/mm3 in peripheral blood, M0-1.
Poor prognostic factors for Sézary syndrome:
The median survival of Sézary syndrome is estimated to be 3–5 years with a five-year survival of less than 30%.