Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Authors: Vanessa Ngan, Staff Writer, 2005; Updated: Dr Ian Coulson, Consultant Dermatologist, East Lancashire NHS Trust, UK. Copy edited by Gus Mitchell. October 2021
Introduction Demographics Causes Clinical features Complications Diagnosis Differential diagnoses Treatment Outcome
Delusions of parasitosis is a condition in which sufferers have a fixed, firm but erroneous belief that they are infested by living organisms such as lice, fleas, fungi, yeasts, worms, and even lizards.
It may be a primary condition, or secondary to other psychiatric conditions such as dementia, schizophrenia, depression, underlying medical conditions, recreational drug use, and prescribed medications. It is sometimes called delusional infestation, parasitophobia, psychogenic parasitosis, or Ekbom syndrome.
It is uncommon; the incidence has been reported to be between 1.9 to 27.3 cases per 100,000 population. The average age of presentation is in the late 50s and early 60s. Some surveys have found a female predominance (2:1), and less common in those of skin of colour.
Primary delusions of parasitosis are of unknown cause, but is thought to be the result of an increase in dopamine within the basal ganglia of the brain.
Secondary delusions of parasitosis may be due to:
Sufferers complain of crawling sensations under the skin, which will result in scratching and excoriations. They will find pieces of skin, crusts, and scabs, and interpret them as parasites, insects, or other living organisms.
They may complain of insects or worms appearing from their nose, ears, mouth, intestines, or genitalia.
They may have contacted the environmental health department and had their dwelling fumigated, and contacted several medical practitioners and entomologists.
Pets may have been dispatched to the vet for examination and treatment.
Other family members may have been convinced of the notion that they are infested and persuaded to apply insecticides and antiseptics.
Examination may show excoriations and ulcers from picking or gouging the skin to remove perceived parasites.
There may be an odour of antiseptics, disinfectants, and insecticides.
Specimens of skin and scabs may be brought as proof of their infestation (the 'matchbox sign').
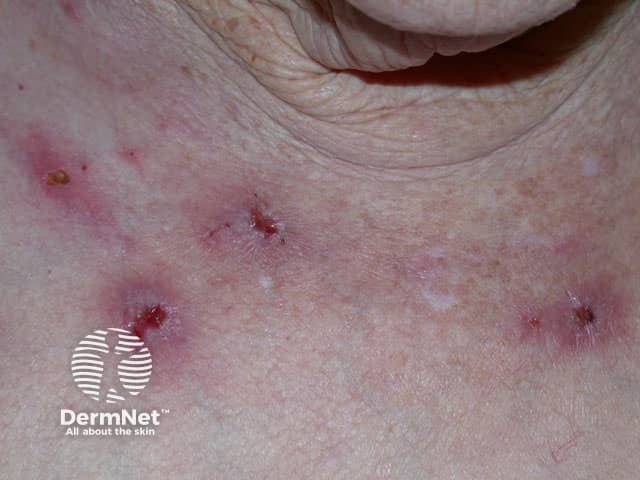
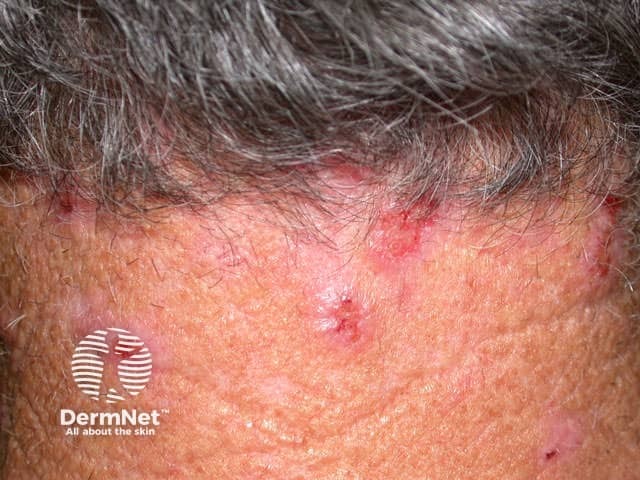
Excoriations
Other laboratory tests should include:
Often several consultations are required to gain trust, with repeat examinations of the skin, and any specimens offered. It is useful for the physician to express their concern for their distress, take time to listen to their complaints, and not be judgemental or dismissive. It can help to state that examination and microscopy “does not show any evidence of parasites today”. It is useful to explain that they have been able to help patients with similar symptoms in the past.
It is essential that there is no collusion with the patient, nor should the physician assert that the psychotropic drugs have “parasite killing” effects.
State that no parasites have been identified on microscopy and that these symptoms of crawling and itching are being interpreted by the brain as infestation, even though no parasites are evident, and that addressing these symptoms with medication will help.
Patients are often reluctant, and even refuse, to see psychiatrists. A remote liaison between the dermatologist and a psychiatrist can be helpful.
Symptoms of depression should be sought, as they may need specific treatment with a selective serotonin reuptake inhibitor.
Medications used include:
Between 60 to 100% of patients are reported to significantly improve with antipsychotics.
See the British Association of Dermatologists guidelines for the management of adults with delusional infestation 2022 for more information on the use and dosages of antipsychotic medication.
Antipsychotic medication is needed for at least 6 months, and can be tapered down thereafter and discontinued according to symptom control. Symptoms may recur and medication may be needed intermittently.