Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Ben Tallon, Dermatology Registrar, Auckland Greenlane Hospital, 2007. DermNet Update August 2021
Introduction Demographics Causes Clinical features Complications Diagnosis Differential diagnoses Treatment Outcome
Pruritic papular eruption of HIV (Human Immunodeficiency Virus) is the most common rash associated with HIV infection, and is often the presenting sign in an otherwise asymptomatic HIV-positive person.
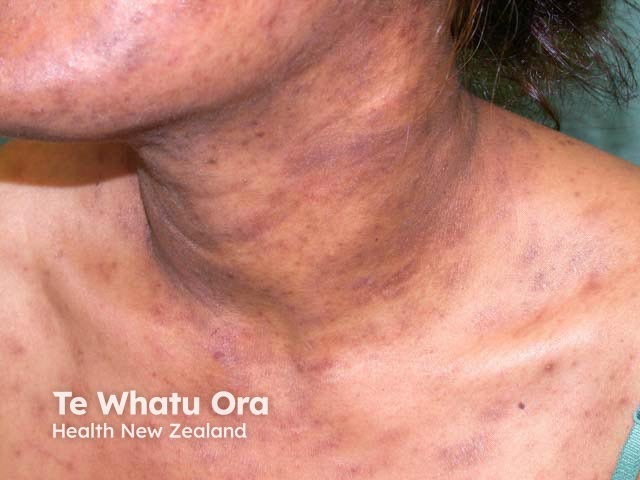
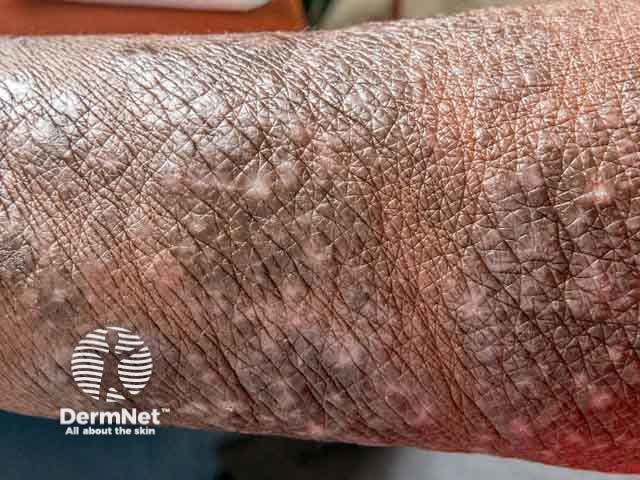
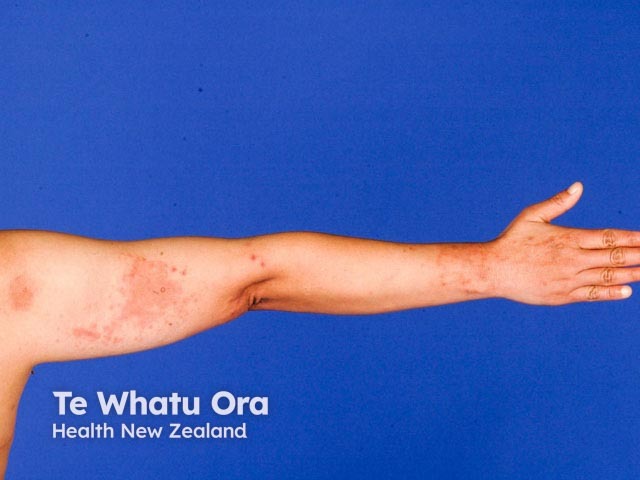
Pruritic papular eruption (PPE) of HIV affects 11–46% of patients with HIV, including children. The prevalence varies with geographic location and is most common in the tropics and subtropical areas.
Most studies report a female predominance.
PPE of HIV is the presenting symptom of HIV in 25–79% of cases. It is classified as WHO Stage 2 HIV disease. It is reported to be a skin sign of advanced HIV, being three times more common when the CD4 lymphocyte count is less than 200 x109/L.
Currently the cause has not been identified. Medications, autoimmunity, and direct HIV infection of the skin have been considered but not proven. An exaggerated immune response to insect bites is supported by the geographic distribution, clinical and histological features, and increased IgE and eosinophils in the blood.
Pruritic papular eruption of HIV presents as a very itchy chronic rash:
PPE of HIV has not been observed in the immune reconstitution inflammatory syndrome (IRIS).
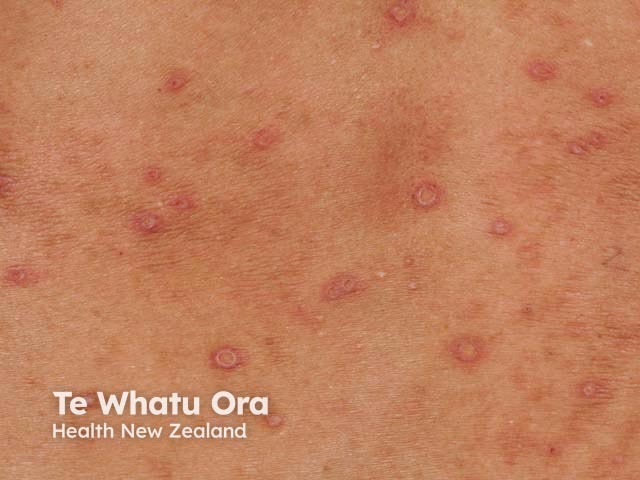
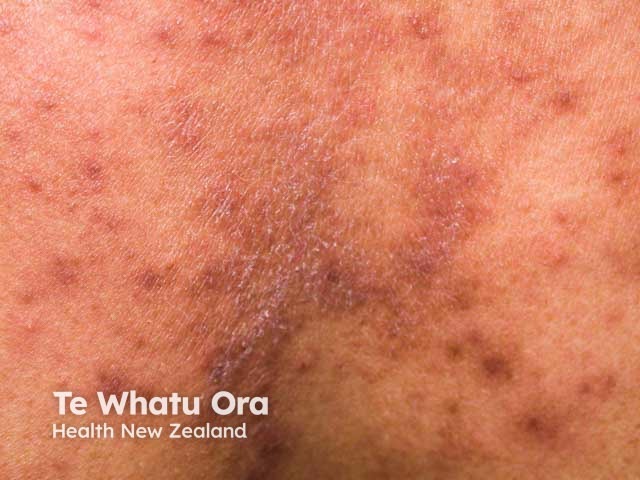
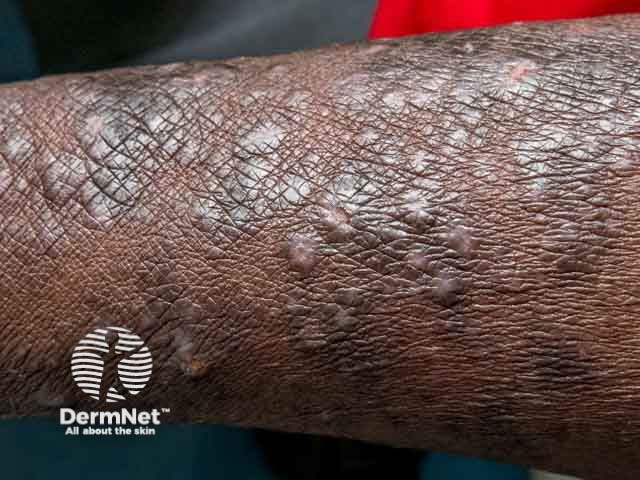
Pruritic papular eruption of HIV should be suspected clinically in a patient at risk of, or known to have, HIV infection.
Investigations include:
Itch may be relieved when using:
Effective highly active antiretroviral therapy (HAART) has been reported in case series to provide not only symptomatic relief of itch, but also resolution of PPE of HIV lesions without recurrence in the majority of patients.
Untreated, pruritic papular eruption of HIV is persistent.