Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Introduction Demographics Clinical features Diagnosis Treatment Proposed mechanism for development
White sponge naevus (Mendelian Inheritance in Man [MIM] number 193900) is a rare genetic condition that causes white spongy lesions of the mucous membranes, most commonly the mouth. It has also been called congenital leukokeratosis, mucosa oris, hereditary leukokeratosis, white folded gingivostomatitis, oral epithelial naevus and oral white sponge naevus.
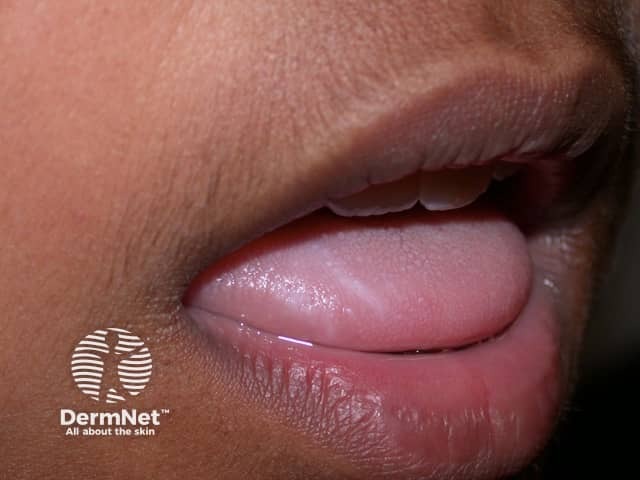
White sponge naevus
White sponge naevus is an autosomal dominant condition, meaning children of an affected parent have a 50:50 chance of inheriting the condition. However it can occasionally be sporadic with no history of affected family members.
It is believed to be rare, but may be underdiagnosed, especially in the absence of similar lesions affecting family members.
The extent of expression varies from case to case, from absent or mild to extensive changes. Some authors claim females are more commonly affected than males.
White sponge naevus may be present at birth or appears later in childhood or adolescence.
White sponge naevus presents as bilateral, sometimes symmetrical, soft white raised lesions of mucous membranes. The surface may appear folded and it feels spongy, not hard. It cannot be detached. The change may be quite subtle and localised or can involve the entire inside of the mouth.
It usually does not cause any symptoms, but patients may complain of roughness and of the appearance.
The mouth is the commonest site affected and the insides of the cheeks the most common site within the mouth. However the mucous membranes of inside the nose, the oesophagus, the genitalia (vulva and vagina) and anorectal sites can also be involved. Usually the mouth is the first site noticed.
No changes are noticed elsewhere on the skin, nails, hair or teeth. This is important when considering other possible causes of the lesions.
There have been no reports of oral cancer developing in a white sponge naevus.
The combination of the clinical appearance, the absence of any other skin problems and a positive family history should raise the possibility of this diagnosis which is then confirmed on biopsy of the lesion and pathology examination. The histopathology of white sponge naevus is very characteristic and in particular shows extensive areas of large clear skin cells in the epidermis.
The diagnosis can now be made definitively on genetic analysis and identification of a mutation in a highly conserved sequence of one copy of the gene coding for the keratin 4 or 13 proteins.
Many other genetic conditions may show white patches in the mouth, but these can usually be excluded on clinical examination as they all have visible changes elsewhere on the skin, nails, etc. These include pachyonychia congenita, Darier disease, dyskeratosis congenita and hereditary benign intraepithelial dyskeratosis.
Most commonly white sponge naevus is misdiagnosed as oral candidiasis (thrush) but this can be excluded on microbiological swabs, failure to respond to antifungal treatment and biopsy. A clue on clinical examination is that the white patches of candidiasis can be peeled off.
The second most common misdiagnosis is oral lichen planus and this is readily distinguished on biopsy.
Other causes of localised white patches in the mouth that may cause confusion include leukoplakia, cheek biting, chewing of tobacco or betel nut (oral submucous fibrosis), syphilis and lupus erythematosus. Again, the pathology of a biopsy will clarify this.
One of the important reasons for making this diagnosis is to avoid unnecessary treatment. In general, explanation and reassurance are all that is required.
When treatment is requested there have been some reports of successful control using topical or systemic antibiotics:
These are not curative, but may sometimes induce either a complete or partial remission which may be maintained by continuing with a low dose. When the antibiotic is ceased, the condition recurs, usually after weeks or months. Why these antibiotics should help some patients is unclear.
Many other treatments have been tried unsuccessfully including topical antifungal agents, oral antifungal therapies, retinoids such as acitretin and isotretinoin, vitamins and other antibiotics such as metronidazole and trimethoprim + sulphamethoxazole.
White sponge naevus is now known to be due to a mutation in the highly conserved regions of the 1a or 2b domains of the genes coding for keratin 4 or 13. Most commonly a missense mutation is found resulting in a change in a critical amino acid which interferes with the assembly of the intermediate filaments. Keratin 4 and 13 proteins are only produced in the oral, nasal, oesophageal and anogenital mucosae, hence the reason for the change being localised to these areas. Electron microscopy of white sponge naevus shows the abnormal aggregation of the intermediate filaments in the large clear cells.