Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Daniel Jun Yi Wong, Medical Student, University of Melbourne, Australia, 2013.
Achromic naevus is an uncommon birthmark (naevus) characterised by a well-defined pale patch. This is usually several centimetres in diameter, with an irregular but well-defined border. Shape and size varies. Often, smaller hypopigmented macules arise around the edges, resembling a splash of paint.
Achromic naevus (American spelling nevus) is also called naevus depigmentosus and non-pigmented naevus. The name is not quite right, as the hypomelanotic patches of an achromic naevus are not completely white, unlike the areas of depigmentation in vitiligo, which are amelanotic, and completely lacking melanocytes. Achromic naevi are usually solitary, in contrast to tuberous sclerosis, where multiple pale patches occur and are called ash-leaf spots.
Achromic naevus is usually noted at birth or early childhood, although lesions may not be apparent until mid-childhood in those with light-coloured skin. The naevus remains stable over time apart from growing with the child. Achromic naevus most commonly arises on the trunk, but may also arise on the limbs and elsewhere. It is solitary in 50% of cases and may follow Blaschko lines.

Achromic naevus
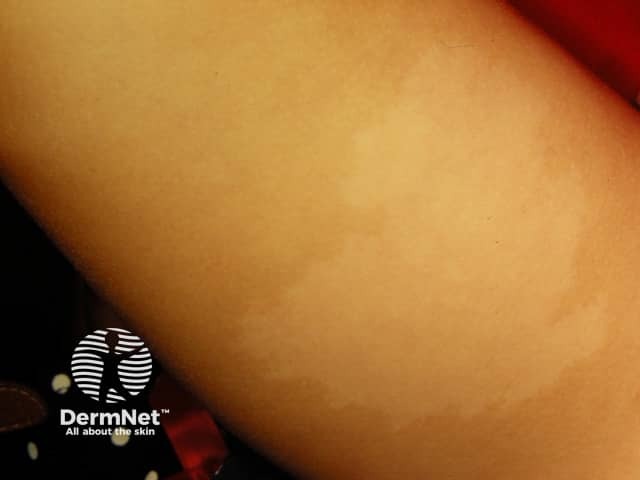
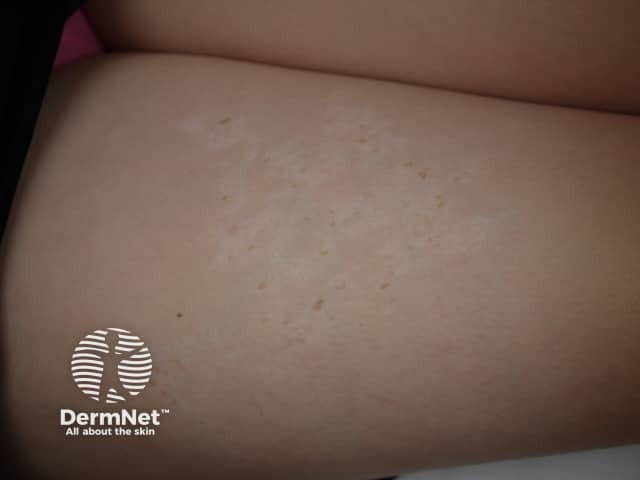
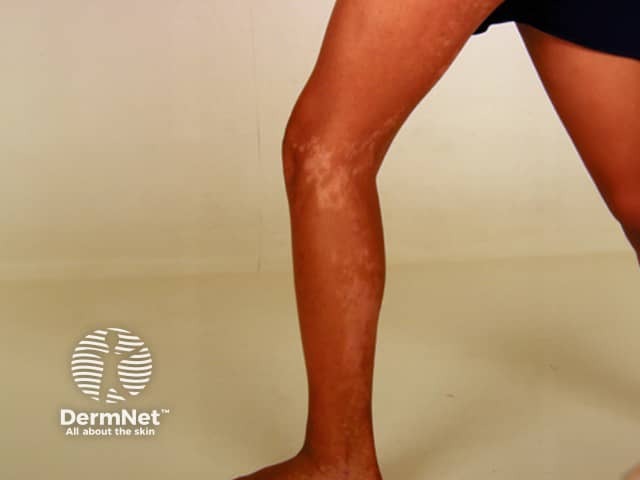
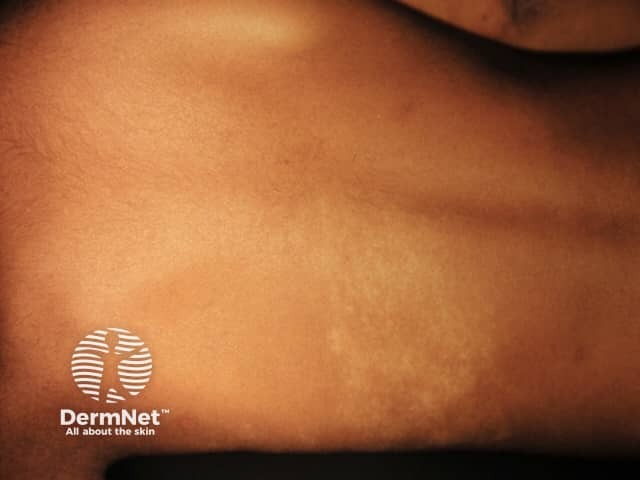
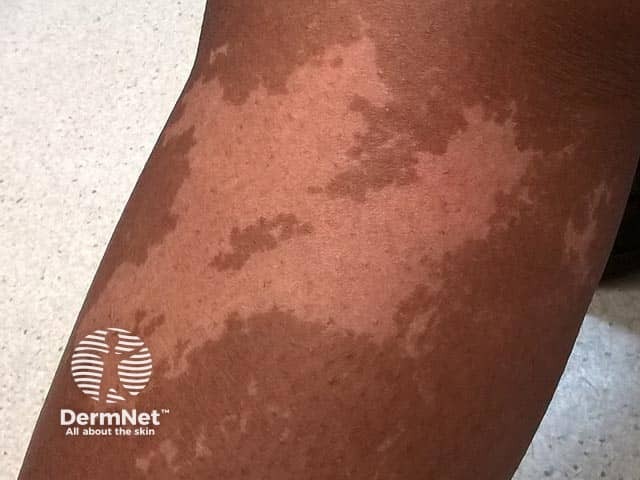
A unilateral depigmented lesion on the arm - the child was otherwise well. Now termed segmental pigmentation disorder
Achromic naevus is a form of cutaneous mosaicism. It is caused by an altered clone of melanocytes (pigment cells) with a decreased ability to make melanin (brown pigment). Melanocyte numbers are normal or reduced in number, Melanosomes may be reduced in the melanocytes and/or keratinocytes suggesting impaired transfer.
Variants of achromic naevus include:
Occasionally, achromic naevus is associated with other neurocutaneous disorders. Co-localised lentigines have been reported and are seen in figure 3 (top right) above. They may represent a reverse mutation. The ash-leaf macules seen in tuberous sclerosis are oval-shaped hypopigmented macules and look similar to achromic naevi but usually present as multiple lesions.
Coupe identified diagnostic criteria for achromic naevus in 1976:
Wood lamp examination: achromic naevus appears off-white, compared to the chalk-white accentuation seen in vitiligo.
Dermoscopy of achromic naevus: serrated border, pallor, and faint pigment network.
Skin biopsy: normal or slightly reduced melanocyte numbers with decreased melanin.
Treatment of achromic naevus is often unnecessary. Cosmetic camouflage may be helpful. Some of the options that have been used to attempt repigmentation include: excimer laser, phototherapy (PUVA), and skin grafting.