Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Reviewed and updated by Dr Amanda Oakley, Dermatologist, Hamilton, New Zealand; Vanessa Ngan, Staff Writer; Clare Morrison, Copy Editor, March 2014.
Introduction
Differences between adolescent and adult acne
Treatment
Acne in adults is also called postadolescent acne. It can be persistent, with onset during teenaged years, or late onset beginning after the age of 25 years. Acne affects up to 15% of women, but is usually reported to be less common in men.
Adult acne can be predominantly inflammatory, with papules and pustules, or predominantly comedonal, often with many large closed comedones (whiteheads). Deep inflammatory lesions and macrocomedones may result in scarring.
Adult acne usually presents as acne vulgaris (common acne). But it often has the following characteristics.
As in younger subjects, hormonal factors may be important including pregnancy, polycystic ovarian disease and medicines (including supplements) with male hormone activity.
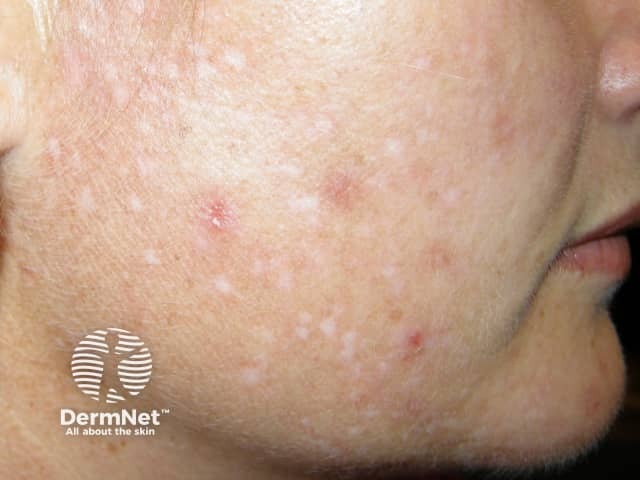
Adult acne
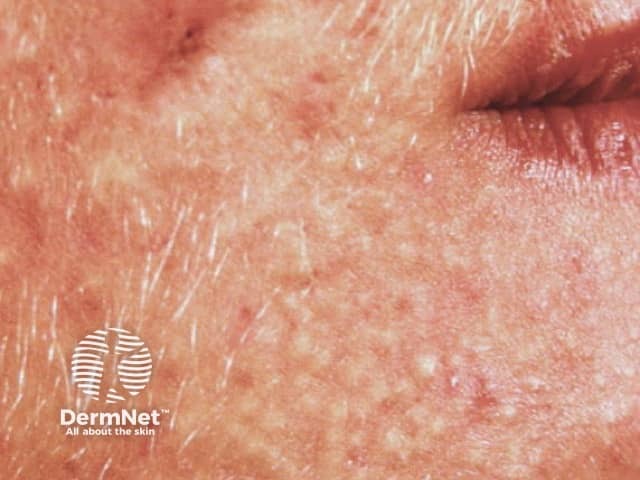
Adult acne
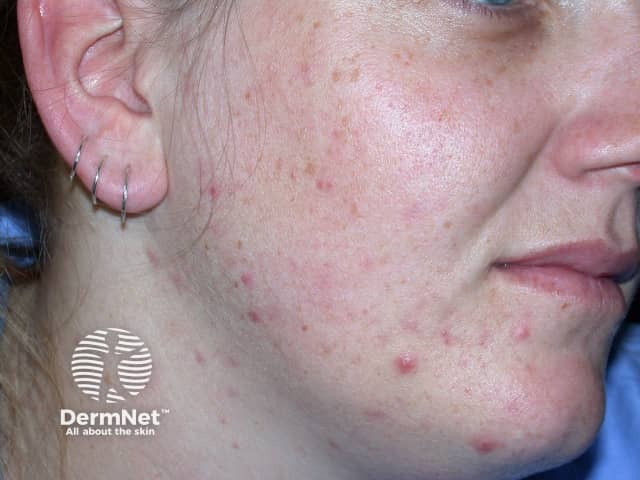
Adult acne
Adult acne treatment is no different from that in younger individuals. However, because of the persistence of the disorder, more aggressive treatments may be recommended for relatively mild symptoms. Many adults consider acne abnormal at their age and demand effective treatment.
Environmental factors should be evaluated, and patients with acne should be encouraged to minimise their intake of high glycaemic index foods. Make-up should be non-occlusive.
Mild acne is treated with topical anti-acne medications. This is suppressive, not curative, and needs to be continued to maintain effects. Some people find blue light treatment has moderate efficacy at reducing the number of inflammatory lesions.
More severe acne may also be treated with anti-inflammatory antibiotics such as tetracyclines. Antiandrogens such as certain oral contraceptives and spironolactone are also widely used as a treatment of persistent acne in women.
Oral isotretinoin can be very effective for adult acne. It is well tolerated in low doses and may result in suppression of the acne for several years or long term. However, it has important side effects and risks. It must not be taken in pregnancy as it may cause birth defects.