Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Karen Koch, Consultant Dermatologist, Wits University, Donald Gordon Medical Centre, Johannesburg, South Africa, November 2017; DermNet Update. Copy edited by Gus Mitchell. June 2021
Introduction Demographics Causes Clinical features Variation in skin types Complications Diagnosis Differential diagnoses Treatment Outcome
Atrophoderma of Pasini and Pierini is a rare form of dermal atrophy characterised by asymptomatic slightly depressed areas with a well-defined ‘cliff-drop’ edge.
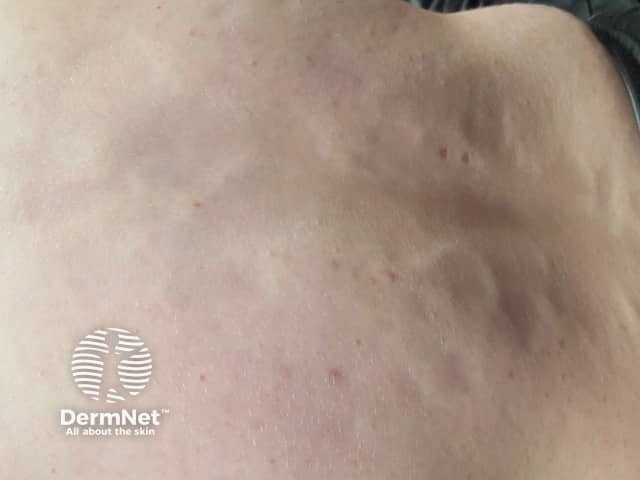
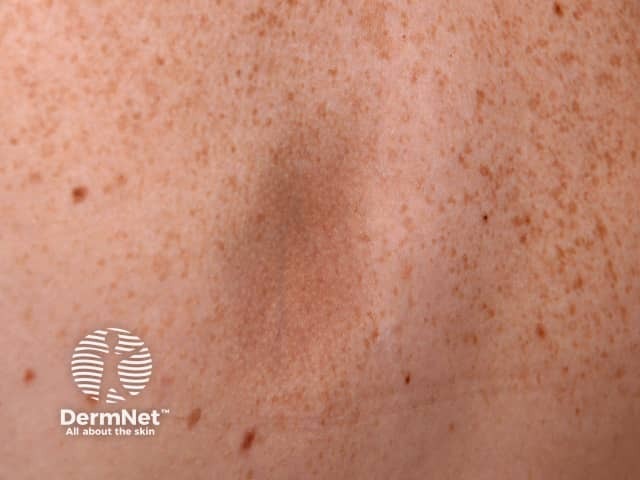
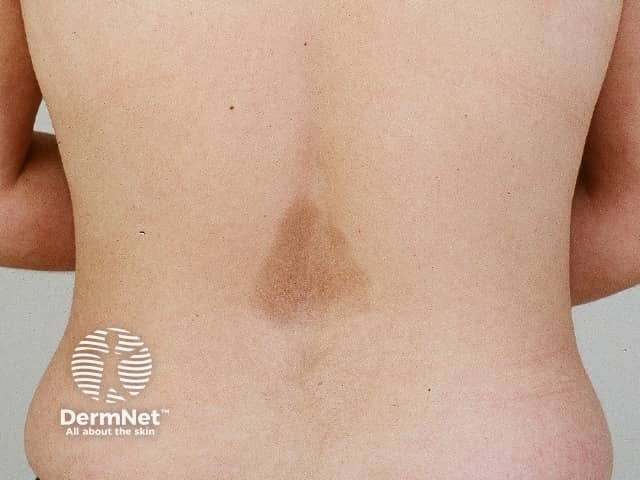
Atrophoderma of Pasini and Pierini is rarely reported with only about 100 cases in the medical literature.
Atrophoderma of Pasini and Pierini usually first appears in adolescence or early adulthood (second and third decade). Onset in infancy, childhood, and late adult-life has been reported, as has congenital presentation.
There is a strong female predominance (2-6:1) and most reports have been in Caucasians. Familial cases have been described.
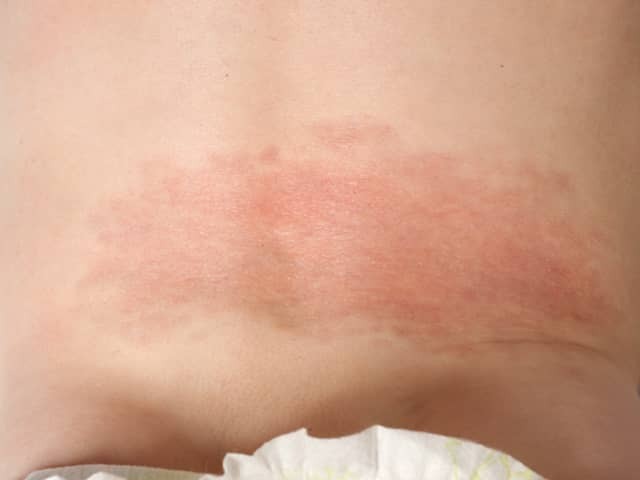
Baby aged 10 months
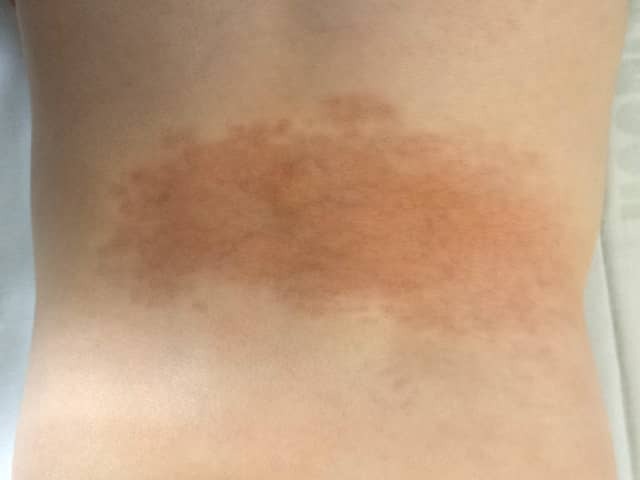
Baby aged 20 months
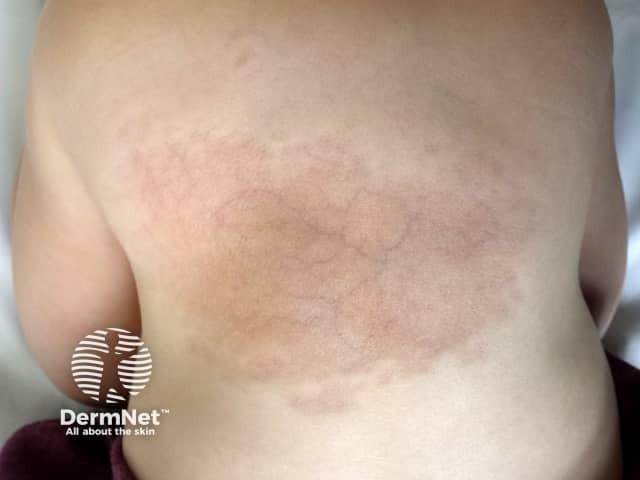
Visible subcutaneous vessels
*First two images are reproduced with permission from John Wiley and Sons. Liu S Oliver F, Agnew K. An unusual infantile rash. Clin Exp Dermatol. 2018;43:835–8. doi:10.1111/ced.13541
Atrophoderma of Pasini and Pierini is usually regarded as a variant of morphoea (localised scleroderma) due to overlapping clinical and histological features and the association in some cases with typical morphoea.
A subset of patients with atrophoderma of Pasini and Pierini have antibodies against Borrelia burgdorferi, and treatment with doxycycline has been reported to improve the skin lesions in some cases with IgM antibodies.
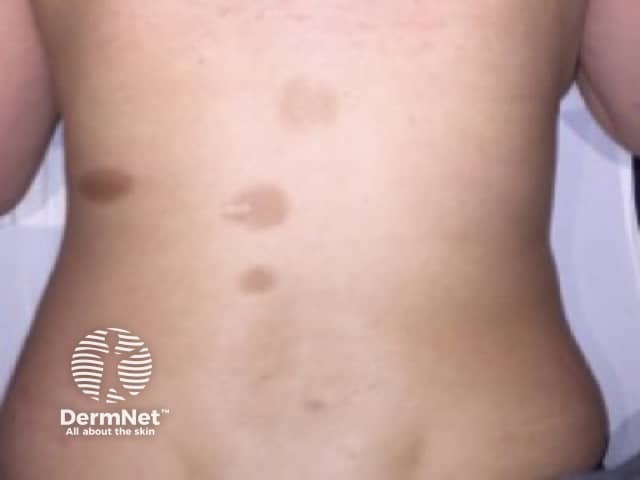
Hyperpigmented lesions
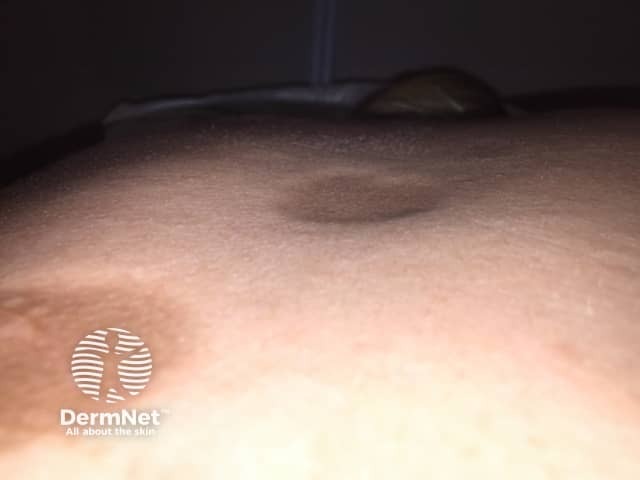
Cliff-drop edge
Lesions of atrophoderma of Pasini and Pierini are usually described as being hyperpigmented, but in skin of colour lesions are often hypopigmented or skin-coloured.
Atrophoderma of Pasini and Pierini can be associated with morphoea or systemic sclerosis. Sclerodermatous changes, detected clinically as areas of induration, may develop within pre-existing areas of dermal atrophy with histology resembling morphoea.
Atrophoderma of Pasini and Pierini should be considered on the history and clinical features. Dermal atrophy can be demonstrated on ultrasound. In endemic areas, serology for B. burgdorferi is recommended.
If a skin biopsy is required, it should be taken as a deep wedge across the border to include both involved and uninvolved skin down into the subcutis as the changes on histology are subtle:
There is no recognised treatment for atrophoderma of Pasini and Pierini. Cases associated with B burgdorferi antibodies may improve with doxycycline. Hydroxychloroquine and methotrexate have been reported to be co-incidentally effective in rare cases with associated disorders such as lupus erythematosus or psoriasis. Treatment with a Q-switched alexandrite laser (755nm) may help fade the hyperpigmentation.
Atrophoderma of Pasini and Pierini may remain unchanged or slowly progress over years with increasing size and numbers of lesions which may coalesce. Eventually it usually stabilises. Characteristically lesions do not involute, but spontaneous improvement has been reported.