Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Introduction Demographics Clinical features Diagnosis Treatment
Anetoderma is an uncommon condition in which the elastic tissue in the dermis is lost, resulting in a depression in the skin. It is also known as macular atrophy.
Anetoderma more commonly affects women than men, and the usual age range is 15–25 years. There is perhaps an increased incidence in premature babies, especially those with very low birthweight, and the lesions may develop where adhesives such as for monitoring leads had been attached.
Anetoderma seems to be most commonly reported in Central Europe.
There have been rare cases of anetoderma affecting family members including monozygotic (identical) twins.
There are two forms of anetoderma – primary and secondary. The cause of the primary form is not known.
Secondary anetoderma occurs at the site of other unrelated skin conditions which include:
Both forms of anetoderma may be associated with systemic diseases including:
There appears to be a particular association with the presence of anti-phospholipid antibodies, often without the other features required to diagnose anti-phospholipid syndrome.
The old classification of Schweninger-Buzzi and Jadassohn-Pellizari types, non-inflammatory versus inflammatory, is no longer considered useful as both types of lesion can be seen in the one patient and many clinically non-inflammatory lesions show inflammation on histology. This classification does not predict prognosis and is therefore no longer used.
There have been many theories proposed to describe the mechanism of development of anetoderma, but at this time this remains unknown.
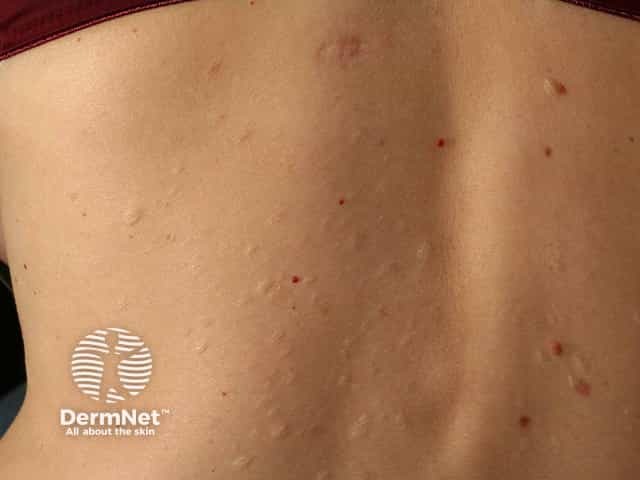
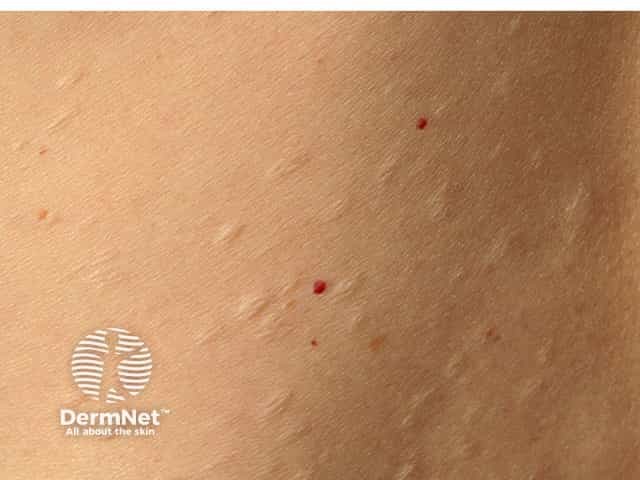
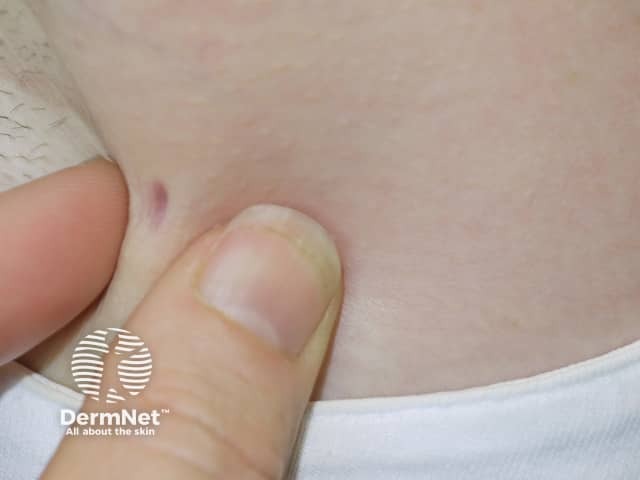
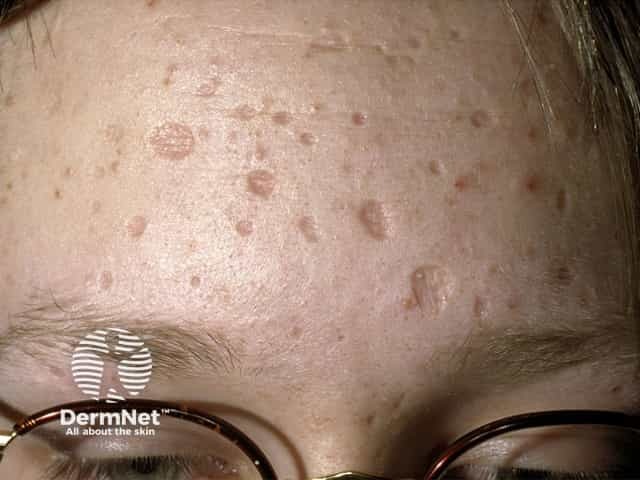
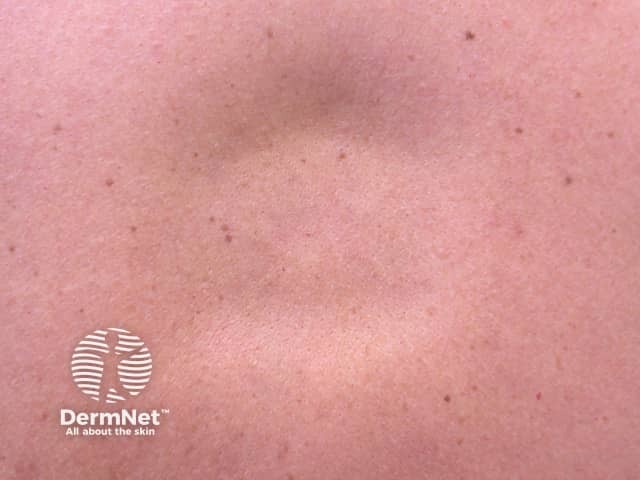
The typical clinical presentation of anetoderma is of multiple round well-defined 1–2 cm lesions with wrinkly skin overlying a palpable depression, the so-called button-hole sign.
Lesions may be flat, raised or depressed, skin-coloured or bluish-white.
Anetoderma lesions are most commonly found on the chest, back, neck and arms, but any site can be affected. They are not related to hair follicles.
Chickenpox scars
Lupus profundus
Anetoderma needs to be considered clinically so the pathologist knows to do the special stains on skin biopsy specimens. These are necessary to demonstrate the loss of elastic fibres in the upper to mid-dermis. On routine stains the skin looks relatively normal, perhaps with some signs of inflammation.
Some authors suggest doing blood tests for Borrelia serology where appropriate, and for autoimmune conditions including antiphospholipid antibodies (lupus anticoagulant and anticardiolipin).
There is no successful treatment to reverse the already formed lesions of anetoderma. Single lesions may be excised. Where an underlying condition has been diagnosed, successful treatment can prevent the formation of further lesions.