Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Juvenile plantar dermatosis — extra information
Juvenile plantar dermatosis
Author: Original page by Dr Amanda Oakley, Dermatologist, Hamilton, New Zealand, 1997. Updated by Dr Anita Eshraghi, Dermatologist, Sweden, and Dr Oakley, in March 2018. Revised September 2020.
Introduction Demographics Causes Clinical features Complications Diagnosis Differential diagnoses Treatment Outcome
What is juvenile plantar dermatosis?
Juvenile plantar dermatosis is a common and chronic, dry-skin condition of the feet that mainly affects pre-adolescent children.
Juvenile plantar dermatosis is also known as atopic winter feet and forefoot dermatitis.
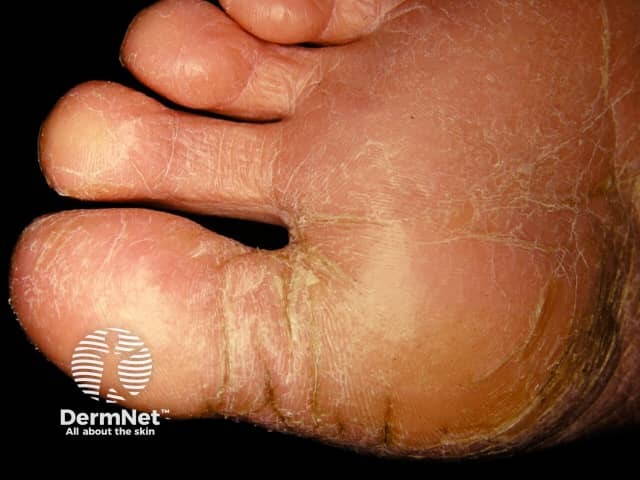
Juvenile plantar dermatosis
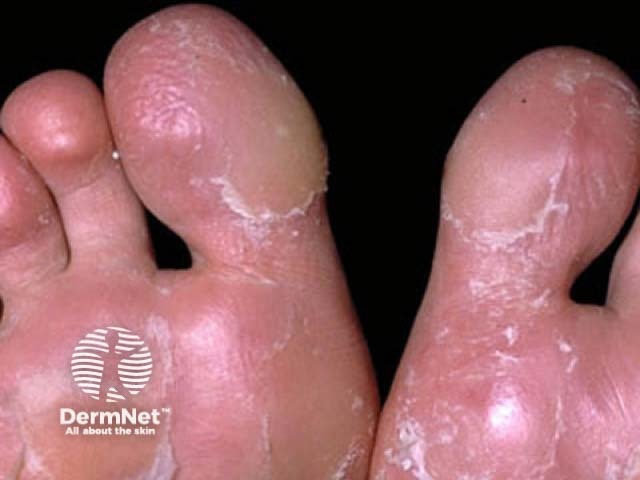
Juvenile plantar dermatosis
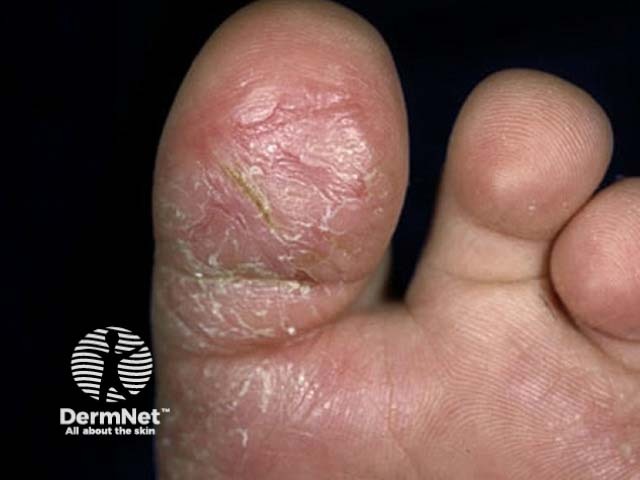
Juvenile plantar dermatosis
See more images of juvenile plantar dermatosis.
Who gets juvenile plantar dermatosis?
Juvenile plantar dermatosis commonly affects children between the age of 3 and 14 years, with an average age of 8. It occurs slightly more frequent in boys than girls. Juvenile plantar dermatosis is rarely seen in adults.
Although an association has been suggested with atopic dermatitis, asthma, or hay fever, this has not been confirmed in case control studies.
What causes juvenile plantar dermatosis?
Juvenile plantar dermatosis may be caused by:
- Repetitive frictional movements, as the foot moves up and down in a shoe
- The occlusive effect of covered footwear, especially synthetic shoes (eg, nylon or vinyl)
- Excessive sweating (hyperhidrosis), which when followed by rapid drying leads to cracking and fissuring
- Genetic sensitivity of the skin
- Climatic changes: with worsening during the summer months due to heat and sweating, and in colder months due to the wearing of winter boots. Hence there is no consistent seasonal variation.
What are the clinical features of juvenile plantar dermatosis?
Juvenile plantar dermatosis involves the weight-bearing areas of the soles of the feet presenting as itchy or sore, shiny, red skin with a glazed appearance and loss of the epidermal ridge pattern.
- It usually affects both feet symmetrically.
- Painful fissures, cracking, and scaling occur.
- The plantar aspect of the great toes (ball of the big toes) is the commonest site of involvement and is the usual initial site.
- Common involvement of the ball of the foot (forefoot) and in some cases the heel; toe-webs and instep are usually spared, helping to distinguish this from tinea pedis.
- It can rarely affect the palms and fingertips.
What are the complications of juvenile plantar dermatosis?
- The most common complication of juvenile plantar dermatosis is painful cracks and fissures. These may take many weeks or months to heal.
- Secondary bacterial skin infection is rare.
How is juvenile plantar dermatosis diagnosed?
The diagnosis of juvenile plantar dermatosis is based on the clinical findings.
Skin scrapings to exclude a fungal infection (tinea pedis) and patch tests for contact allergy to footwear may be performed.
Skin biopsy is rarely required. Histology shows epidermal spongiosis and dermal inflammation centred around the sweat ducts.
What is the differential diagnosis for juvenile plantar dermatosis?
Juvenile plantar dermatosis is sometimes difficult to distinguish from:
- Atopic eczema
- Keratolysis exfoliativa (focal peeling)
- Plantar psoriasis
- Tinea pedis
- Allergic contact dermatitis to shoe material, such as rubber accelerant, an adhesive such as paratertiary butylphenol formaldehyde (PTBF) resin, or chromate used as a leather tanning agent.
What is the treatment for juvenile plantar dermatosis?
There is no consistently useful treatment. General recommendations include the following without supporting studies to show benefit.
Reduce friction
- Wear well fitting shoes, preferably leather, to minimise friction.
- Wearing two or more pairs of cotton or woollen socks can also help reduce friction.
- Avoid wearing shoes and socks made of synthetic materials.
- Change socks regularly.
Lubricate the dry skin
- Apply moisturising cream containing urea or petrolatum, after bath and before bed.
- Barrier cream (containing dimeticone) are easier to wear during the day and should be applied every 4 hours.
Have a rest daily
- Schedule quiet times with little or no walking to allow fissures to heal.
Cover cracks
- Fissures heal faster when occluded. Adhesive plasters are usually satisfactory.
- Spray or liquid acrylate glue can be applied to the fissures to relieve pain.
Prescription ointments
When applied once or twice daily for courses of up to 4 weeks, these rarely prove more effective than simple emollients.
What is the outcome for juvenile plantar dermatosis?
Juvenile plantar dermatosis usually clears spontaneously in adolescence, but can persist into adult life.
References
- Ashton RE, Griffiths WA. Juvenile plantar dermatosis--atopy or footwear?. Clin Exp Dermatol. 1986;11(6):529–34. doi:10.1111/j.1365-2230.1986.tb00504.x. PubMed
- Ashton RE, Jones RR, Griffiths A. Juvenile plantar dermatosis. A clinicopathologic study. Arch Dermatol. 1985;121(2):225–8. PubMed
- Harding CR. The stratum corneum: structure and function in health and disease. Dermatol Ther. 2004;17 Suppl 1:6–15. doi:10.1111/j.1396-0296.2004.04s1001.x. PubMed
- Shipley DR, Kennedy CT. Juvenile plantar dermatosis responding to topical tacrolimus ointment. Clin Exp Dermatol. 2006;31(3):453–4. doi:10.1111/j.1365-2230.2006.02121.x. PubMed
- Elias PM, Choi EH. Interactions among stratum corneum defensive functions. Exp Dermatol. 2005;14(10):719–26. doi:10.1111/j.1600-0625.2005.00363.x. PubMed
- Ingram JR. Eczematous disorders. In: Griffiths C, Barker J, Bleiker T, Chalmers R, Creamer D (eds). Rook's Textbook of Dermatology [4 volumes], 9th edn, Wiley Blackwell, 2016: 39.21-2.
On DermNet
- Dermatitis
- Foot skin conditions
- Atopic dermatitis
- Pompholyx
- Shoe dermatitis
- Patch testing
- Psoriasis
- Tinea pedis
