Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Vanessa Ngan, Staff Writer, 2003. Updated by Dr Karen Koch, Consultant Dermatologist, WTS Donald Gordon Mediclinic, Johannesburg, South Africa. DermNet Editor in Chief Adjunct Assoc. Prof. Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy edited by Gus Mitchell. July 2018.
Introduction Demographics Causes Clinical features Complications Diagnosis Differential diagnoses Treatment Outcome
Porokeratosis is a type of abnormal keratinisation. It presents as a reddish patch (either scaly or atrophic) with a well-defined ridge-like border [1].
Porokeratosis of Mibelli is the second most common form of porokeratosis [2].
Porokeratosis of Mibelli most often starts during childhood but lesions may be present at birth or may first appear at puberty or later [2]. Sometimes it appears during adulthood following the suppression of the immune system by certain medication or illness [3].
Porokeratosis of Mibelli affects men twice as commonly as women [2].
The cause of porokeratosis of Mibelli is unknown. Occasionally there is a family history of porokeratosis of Mibelli or another type of porokeratosis such as linear porokeratosis or disseminated superficial actinic porokeratosis (DSAP), suggesting there is a genetic predisposition to the disorder.
The porokeratosis lesion starts as a small, light brown, scaly papule. Several papules may join into one or more plaques with irregular boundaries. Each plaque is separated from the surrounding skin by a warty rim with well-defined thin furrows running in its centre.
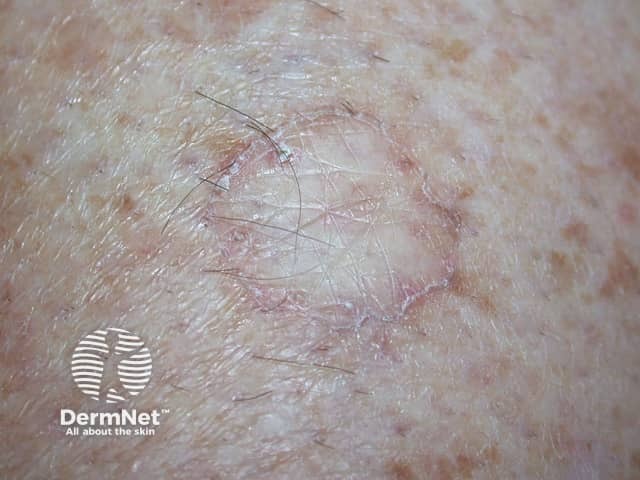
Porokeratosis of Mibelli
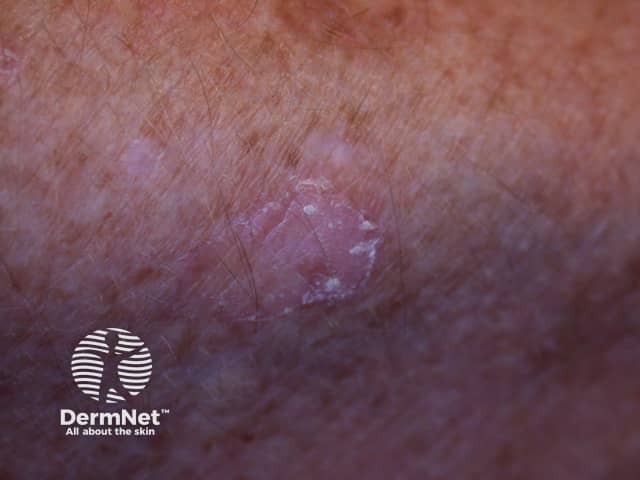
Porokeratosis of Mibelli
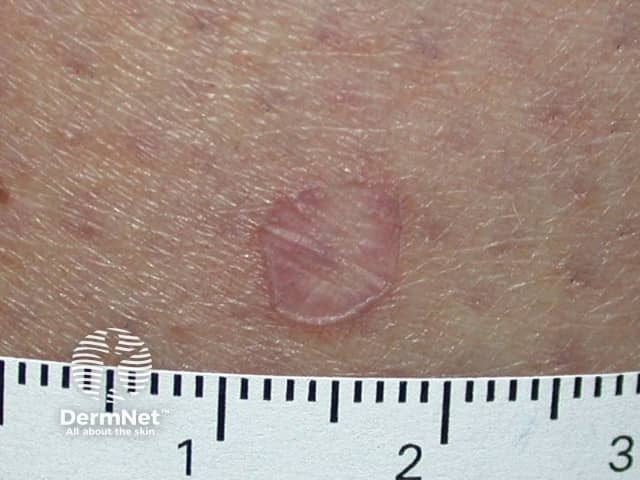
Porokeratosis of Mibelli
Porokeratosis of Mibelli most often affects the limbs, particularly the hands and feet, lower leg, neck, shoulders, face or genitals, although any part of the body may be affected including the mucous membranes [5].
The lesions usually reach only a few centimetres in size but 'giant porokeratomas' can be as large as 10 to 20 cm wide [6].
Lesions may remain unchanged for many years or may slowly grow between long periods of inactivity. A skin cancer can develop within porokeratosis of Mibelli. This may be either a basal or squamous cell carcinoma and is more likely to occur in older adults.
Rarely, porokeratosis of Mibelli may involve the distal fingers or toes and this can result in damage to the nails [8].
The diagnosis of porokeratosis is usually made clinically but sometimes a biopsy is needed. The pathology is very distinct for this condition.
Porokeratosis of Mibelli generally has a very specific appearance but some other skin lesions that could be considered include:
There is no known cure for porokeratosis of Mibelli and treatment is generally disappointing. However, the appearance may improve with the following measures:
Sun protection is very important as exposure to ultraviolet radiation may result in the development of skin cancer within the porokeratosis.
The risk of progression of porokeratosis of Mibelli to a basal or squamous cell carcinoma is about 10% [7]. This presents as a changing, enlarging crusted sore or nodule. It may require a biopsy or is cut out (excision).