Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Dr Emily Horan, Resident Medical Officer, Princess Alexandra Hospital, Brisbane, Queensland, Australia. Medical Editor: Dr Helen Gordon, Auckland, New Zealand. DermNet Editor in Chief: Adjunct A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy edited by Gus Mitchell. September 2020.
Introduction Anatomy and embryology of the skin Microbiota in preterm infants Wraps Neonatal intensive care unit
Premature infants are babies born before 37 weeks of pregnancy, with further classification by gestational age as preterm (32–37 weeks), very preterm (28-32 weeks), or extremely preterm/ultra-low birthweight (less than 28 weeks and/or less than 1000g).
Complications associated with prematurity can be due to an underdeveloped and compromised skin. The quality of a neonate’s skin depends on the gestational age at birth. The skin is very fragile and translucent in extremely preterm neonates.
Skin functions include forming a barrier against water loss and irritants, controlling the absorption of substances, temperature regulation, electrolyte regulation, tactile sensation, protection from mechanical trauma, infection control, and immunity.
The epidermis develops from a single layer of cells to three layers by 11 weeks gestation, and to 4–5 layers by 23 weeks. The stratum corneum layer of the epidermis begins to develop at 15 weeks gestation and forms a functional barrier at 34 weeks’ gestation. Compared to a baby born at term, the epidermis of a preterm infant has fewer cell layers making it vulnerable to injury and heat loss, and with increased permeability to exogenous materials, fluids, and electrolytes. The stratum corneum of a term infant at birth is thicker than in an adult. At birth, the skin surface pH is neutral or slightly acidic, and this does not appear to be influenced by gestational age.
Compared to mature infants and adults, the dermis in premature infants has less structural protein connecting to the epidermis. Collagen fibre bundles are small and elastic fibres are sparse and immature. This leaves premature infants susceptible to skin injuries, including those caused by medical adhesives.
Vernix caseosa coats the skin of a fetus, with synthesis beginning from 28 weeks gestation. The vernix is a mix of water, lipids, and proteins.
Vernix:
The vernix is usually absent in extremely preterm ultra-low weight infants. Babies born at term have less vernix coverage than those born at 32–37 weeks gestation. If vernix is present, it should be retained and allowed to absorb naturally as it improves skin hydration, includes antimicrobial peptides active against common pathogens, has wound-healing properties, and lowers skin acidity.
The microbiota refers to the microorganisms that colonise the human body.
Infants are thought to be virtually sterile at birth and acquire their microbiota over time, reaching mature colonisation at 2–3 years of age. The development of the neonatal microbiota is influenced by the delivery method (vaginal or Caesarean section) and whether the baby is formula or breastfed.
Extremely preterm infants have a lower total microbial diversity than full-term infants. Staphylococcus and Escherichia species predominate on their skin, reflecting the infant's environment. Premature infants are more likely to require prolonged hospitalisation, ventilation and invasive lines, antibiotics and other medications, and have limited skin-to-skin contact with parents and other caregivers, all of which will alter the colonisation and development of the microbiota.
Impermeable wraps may be required to reduce heat loss in the first minutes after birth of a premature baby. Semipermeable wraps may then be used for days to weeks to reduce water and electrolyte loss through the skin. Although adhesive dressings have some advantages over non-adhesive wraps, they can strip the skin and cause irritation. Humidified incubators are also beneficial.
Premature infants may require admission to a neonatal intensive care unit (NICU) for further care due to their complicated medical problems.
Infants admitted to the NICU require supportive care that may increase the risk of skin injury. These include:
A premature infant's skin should be examined all over daily or more frequently as required. Staff in the NICU use tools such as the neonatal skin condition score (NSCS) to assess the skin integrity.
NICU guidelines for bathing, adhesives, care of medical equipment, topical therapies, and care of the umbilical cord aim to keep the infant healthy, warm, and protected from infection. Regular repositioning helps to minimise skin breakdown.
Premature skin develops to resemble the skin of a full-term infant by 2 to 4 weeks of age, although this may take longer in ultra-low weight neonates. Despite this apparent improvement, water loss through the skin remains high and full maturation may take 9 weeks or longer.
Kangaroo mother care is defined as frequent skin-to-skin contact between a mother and her newborn, and exclusive or near-exclusive breastfeeding. Kangaroo mother care can be considered for premature infants once their condition has stabilised. Morbidity and mortality in preterm infants may be reduced, with lower rates of serious infections and hypothermia, and a shorter hospital stay compared to conventional neonatal care. Growth in length, weight gain, and maternal satisfaction are reportedly improved.


Emollients can enhance the barrier function of skin and help to minimise transepidermal water loss. In developing countries, a clear benefit has been seen where preterm infants are traditionally massaged with sunflower seed oil or coconut oil. Traditional mustard seed oil massage, however, is not recommended as it increases skin irritation and decreases barrier function. There have been mixed results reported from research of emollient use in developed countries. Petroleum-based emollients have been discouraged due to some studies showing increased rates of infection in extremely preterm infants.
Baby wipes should be alcohol-free (not including mild benzyl alcohol), and not contain perfume or preservatives (particularly methylisothiazolinone) to reduce the risk of irritation and allergic contact dermatitis. Dry wipes moistened with sterile water can be used, although this lacks the acidifying benefits of some commercial wipes.
Dilute (0.2%) chlorhexidine solution appears to be a safe antiseptic, especially for extremely preterm skin, as it is less irritating than 0.5% chlorhexidine and carries less risk of thyroid suppression compared to povidone-iodine.
Bathing may start at 12–24 hours of age depending on the gestational age of the baby, and can occur at least every fourth day without increasing skin bacterial colonisation or the risk of skin infection. Tub bathing using a swaddled-immersion technique every 4th day appears to have a beneficial effect on temperature instability. Sponge bathing may increase heat loss and lead to cold stress, especially in premature infants. Plain water with a pH neutral cleanser or bath oil can be used. Infants should be dried thoroughly after bathing.
See also Skin conditions in newborn babies.
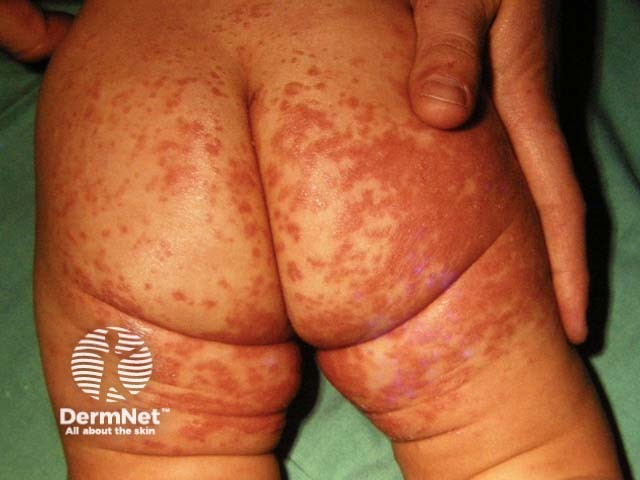
Napkin dermatitis
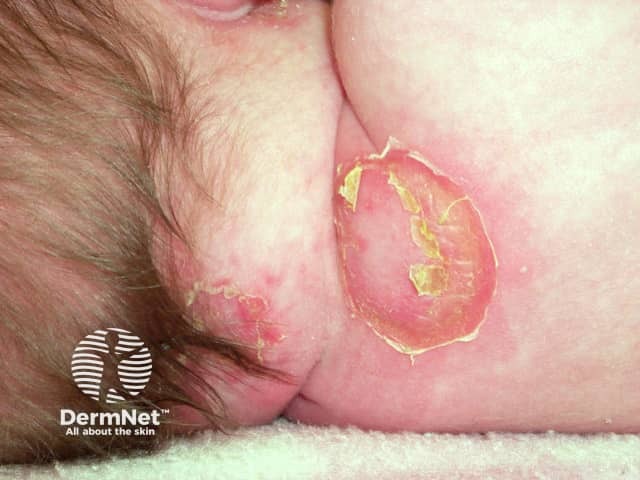
Bullous impetigo in a neonate
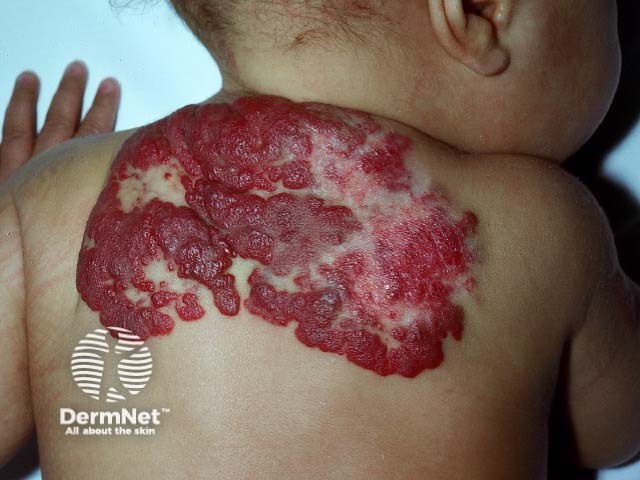
Infantile haemangioma
Napkin dermatitis (American terminology diaper dermatitis) is an irritant contact dermatitis due to wetness. Skin changes typically spare the folds. Neonates urinate more than 20 times daily and the use of antibiotics in NICU may increase the risk of bowel infections and malabsorption resulting in frequent loose stools. The immature barrier function of the stratum corneum may result in preterm infants being more prone to nappy rash than those born at full term.
Strategies to frequently monitor, prevent, and manage napkin dermatitis in a premature infant include:
Napkin dermatitis will often self-resolve within three days. Secondary bacterial infection or yeast infection may complicate nappy rash.
Skin infections are potentially serious in premature infants and may present with a variety of clinical features ranging from erythema to pustular and vesicular rashes. Infection can be due to organisms such as:
Prematurity is a major risk factor for infection caused by antibiotic-resistant bacteria such as methicillin-resistant S. aureus (MRSA) in NICU. Transmission can be vertically from the mother or horizontally from a colonised caregiver in direct contact with the infant. The most common sites of initial colonisation are the umbilical stump or inside the nose, and may progress to serious infections with significant morbidity including staphylococcal scalded skin syndrome. Interventions shown to reduce the risk of MRSA infection in a NICU include increased hand washing and screening/decolonisation of staff and patients.
Infantile haemangioma is the most common vascular tumour in babies and affects up to 30% of premature infants compared to 5–10% of neonates overall. Although benign with eventual regression, complications can arise in large lesions and those in critical locations.
Vascular malformations include capillary vascular malformations, such as naevus simplex and port-wine stain. Naevus simplex is very common in all newborns and does not appear to be more common in preterm babies.
Premature neonates in NICU are exposed to many medications, thereby increasing the risk of an adverse cutaneous drug reaction.