Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Vanessa Ngan, Staff Writer, 2003. Reviewed and updated by Dr Amanda Oakley Dermatologist, Hamilton, New Zealand; and Vanessa Ngan, Staff Writer; June 2014.
Atypical mycobacterial infections are infections caused by a species of mycobacterium other than Mycobacterium tuberculosis, the causative bacteria of pulmonary TB and extrapulmonary TB including cutaneous TB; and Mycobacterium leprae, the cause of leprosy.
Atypical mycobacteria may cause many different types of infections, which are divided into the following four clinical syndromes:
Skin infection tends to result in crusted nodules and plaques. Abscesses may develop in skin and bone infection.
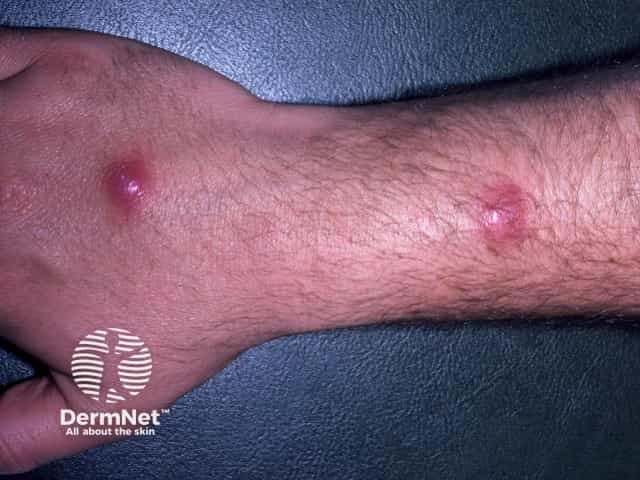
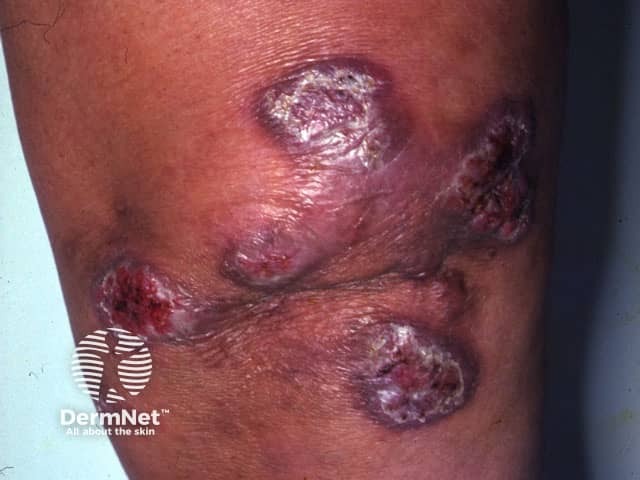
Mycobacterium chelonae
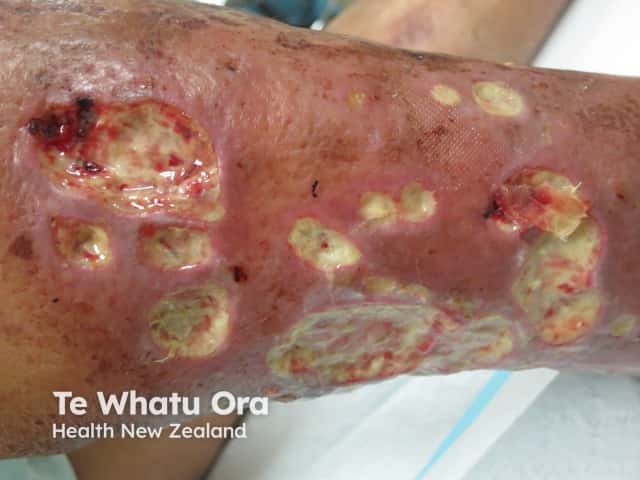
Mycobacterium abscessus
See more mycobacterial infection images
There are many different species of mycobacterium. To date at least 30 species of mycobacteria that do not cause tuberculosis or leprosy have been identified. Some of those causing atypical mycobacterial infections include:
Mycobacterium avium-intracellulare and Mycobacterium kansasii primarily cause lung disease similar to pulmonary TB, whilst Mycobacterium marinum, Mycobacterium ulcerans, Mycobacterium fortuitum and Mycobacterium chelonae cause skin infections.
The clinical features of atypical mycobacterial infection depend on the infecting mycobacteria.
Mycobacterium avium-intracellulare
Mycobacterium kansasii
Mycobacterium marinum
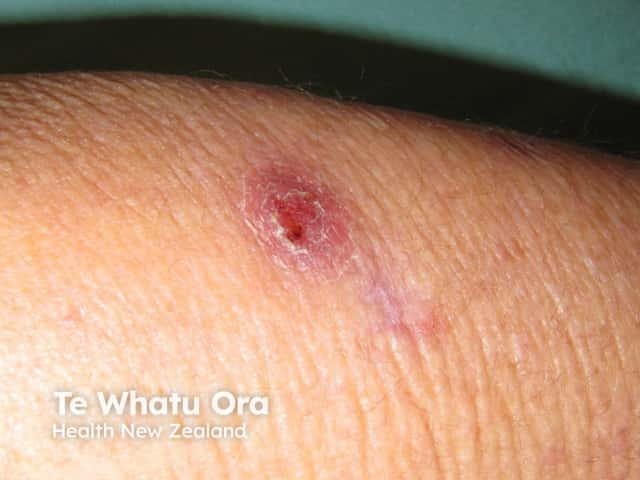
Mycobacterium marinum
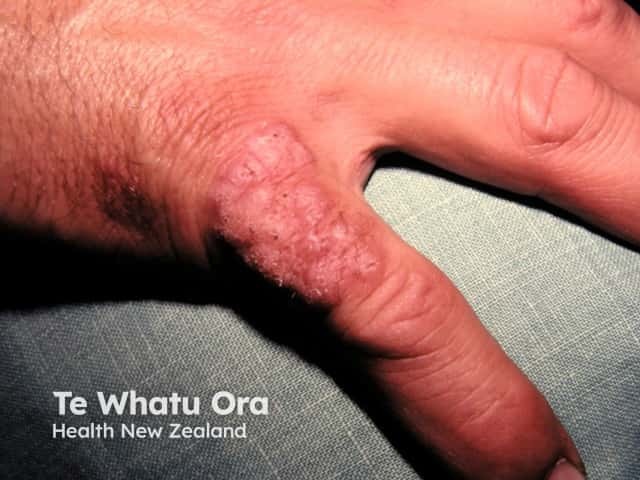
Mycobacterium marinum
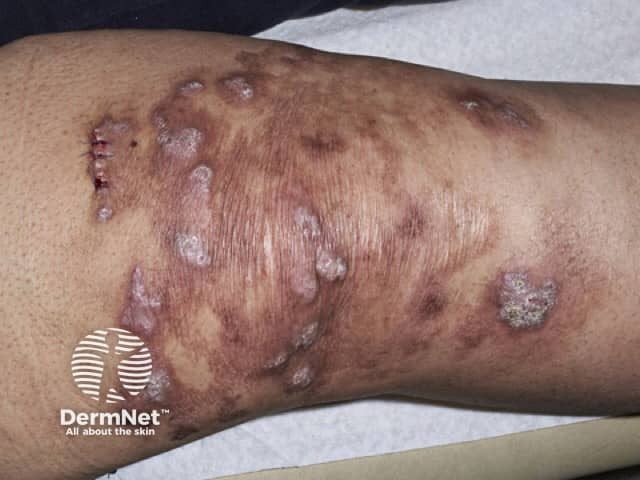
Mycobacterium marinum
See more mycobacterial infection images
Mycobacterium ulcerans
Mycobacterium chelonae
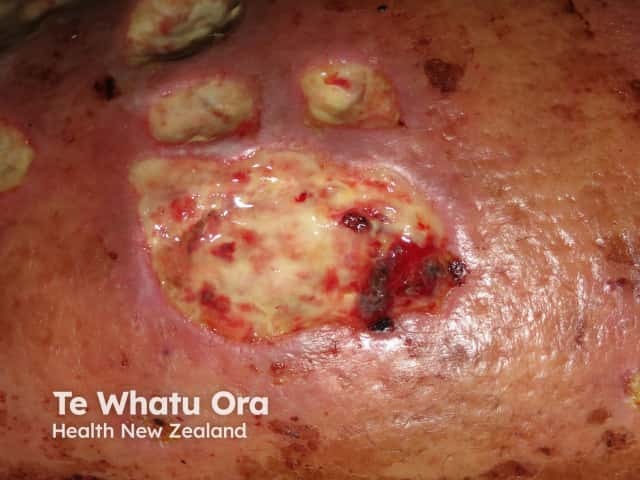
Mycobacterium chelonae
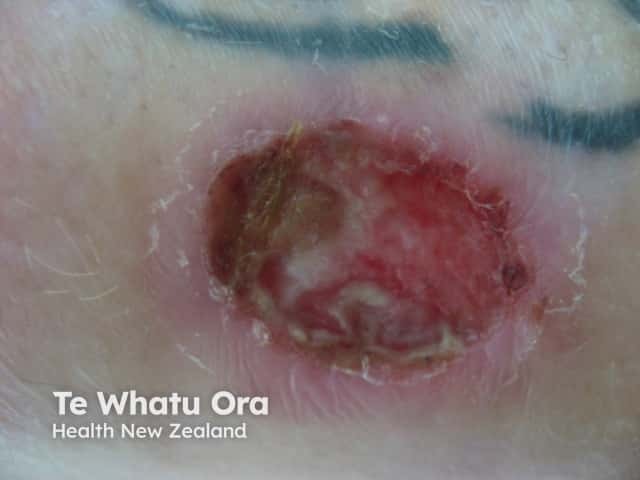
Mycobacterium chelonae
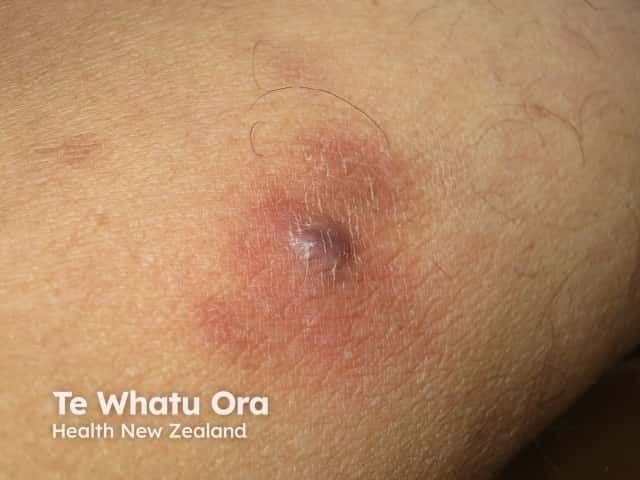
Mycobacterium chelonae
Mycobacterium abscessus

Mycobacterium abscessus
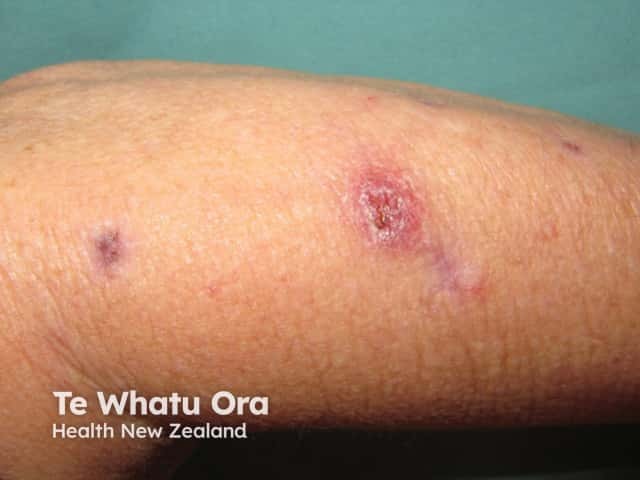
Mycobacterium abscessus
Mycobacterium fortuitum
See more mycobacterial infection images
Atypical mycobacteria are diagnosed on the culture of tissue. Specific conditions are required, such as cool temperature, so the laboratory must be informed of the clinician's suspicion of this diagnosis. The infections have specific pathological features on skin biopsy.
Other diagnostic tools used include radiographic imaging studies and more recently, polymerase chain reaction (PCR) testing on swabs of ulcers or tissue biopsies.
Treatment of atypical mycobacterial infections depends upon the infecting organism and the severity of the infection. In most cases a course of antibiotics is necessary. These include rifampicin, ethambutol, isoniazid, minocycline, ciprofloxacin, clarithromycin, azithromycin and cotrimoxazole. Usually, treatment consists of a combination of drugs.
Consider the following points when treating atypical mycobacterial infections with antibiotics:
Surgical removal of infected lymph nodes and aggressive debridement of infected skin lesions is sometimes necessary. In severe cases, skin grafts may be necessary to repair the surgical wound.
Some infections will heal spontaneously, often leaving significant scarring.