Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Hand care for healthcare workers — extra information
Hand care for healthcare workers
Author: Dr. Louise Reiche, Dermatologist, Palmerston North, New Zealand, 2009. DermNet Update April 2021
The importance of hand care
Hand skin preservation tips
Investigations for hand dermatitis
Treatment
Why is hand care necessary for healthcare workers?
Good hygiene practice and prevention of cross-infection are essential for healthcare workers in hospitals, clinics, aged care facilities, and private homes. Hand care is necessary because healthcare workers are prone to hand dermatitis mostly due to contact with irritants associated with frequent hand washing or cleaning using soap and water, aggressive disinfectants, and detergents. The use of surgical gloves may also cause dermatitis in some individuals.
Hand dermatitis is being seen increasingly in healthcare personnel involved in caring for patients during the COVID-19 pandemic due to the increased hand hygiene and glove requirements at work and after-work hours in the retail/entertainment environment; so-called 'COVID hand dermatitis'.
Exposure to irritants at home or during recreation may exacerbate the problem. Chemicals, extremes of temperature and humidity, mechanical injury (eg, rough surfaces and friction), plants, paints, some foods, and ultraviolet radiation may injure the skin.
The skin barrier may be disrupted by:
- Short, infrequent exposure to strong irritants
- Regular repetitive exposure to less damaging irritants.
Disruption of the skin barrier manifests as frank eczema or irritant contact dermatitis. Damaged skin is itchy, sore, less supple, and susceptible to secondary bacterial infection and the development of allergies (contact allergic dermatitis).
Dermatitis is most likely in those with pre-existing sensitive skin or who have atopic dermatitis in other sites. [see Atopic hand dermatitis]
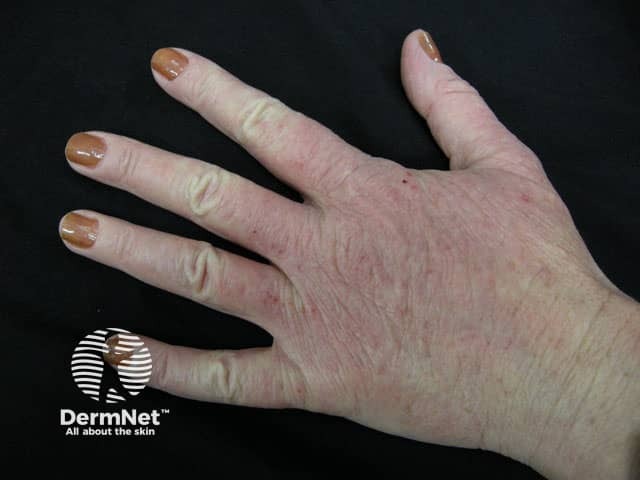
Hand dermatitis
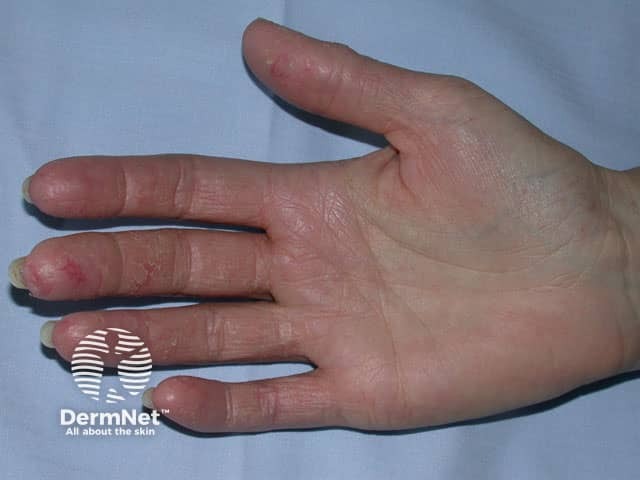
Hand dermatitis
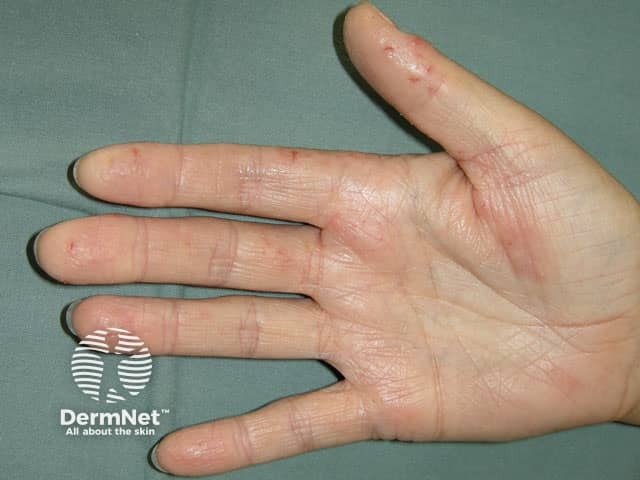
Hand dermatitis
Staphylococcus aureus and Streptococcus pyogenes are the usual causes of a bacterial infection. Hand dermatitis and wet work also predispose to yeast infection, generally presenting as paronychia infected by Candida albicans or as intertrigo between the fingers (erosio interdigitalis blastomycetica), and can be confused with tinea manuum (fungal infection of the hand).
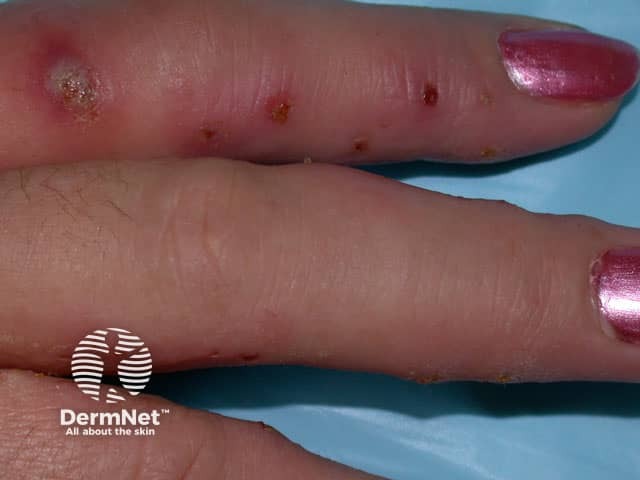
Staphylococcal infected eczema
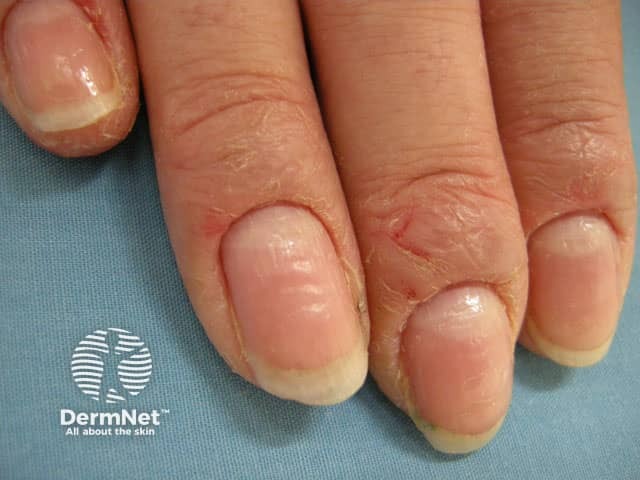
Paronychia
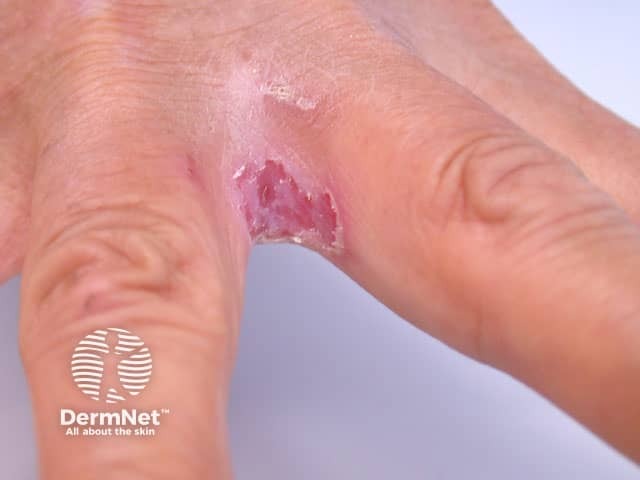
Erosio interdigitalis blastomycetica
Hand skin preservation tips for healthcare workers
Sanitisers
Evidence-based Cochrane reviews confirm alcohol-based hand rubs are superior to regular hand washing for reducing transmission of diseases in hospitals and healthcare services. They also cause less irritation compared with soap and water.
- At work, choose a colourless, alcohol-based hand cleanser without fragrances and perfumes.
- Wash with soap and water only when the skin is visibly soiled or contaminated with blood or other body fluids.
- Note that cream cleansers are not antimicrobial; soap and water or an alcohol-based hand sanitiser is needed for decontaminating hands in order to destroy pathogens such as SARS-CoV-2, the virus responsible for COVID-19.
Gloves
Gloves provide some barrier for the skin, but no single glove type will resist all chemicals indefinitely. Choosing the right glove design and construction will give the best protection, provided it also fits well. Similarly, protection against mechanical risk varies with different gloves providing different strengths of abrasion, blade cut, tear and puncture resistance.
- Latex gloves provide the best protection against viruses for healthcare workers.
- Non-powdered gloves are less irritating and drying than powdered gloves.
- Nitrile gloves are a suitable alternative for people with latex allergy.
- Vinyl gloves are not suitable for healthcare workers in direct contact with bodily excretions.
- Avoid petroleum-based emollients under latex gloves as they weaken the rubber
- If wearing occlusive gloves for more than 20 minutes, use well-fitting cotton gloves beneath them to reduce irritation caused by sweating.
Healthcare facilities often have a health and safety officer with knowledge about suitable gloves. Safety shops also offer advice and a wide choice.
What investigations are appropriate in hand dermatitis?
If hand eczema is slow to improve, seek a referral to a dermatologist for patch tests. Patch tests help decide if a contact allergy is contributing to the hand dermatitis. About 60% of patients with chronic hand eczema have one or more positive contact allergens on patch testing, however the relevance of the positive reaction must be assessed in the clinical situation. Loss of barrier function due to irritant contact dermatitis increases the risk of developing a contact allergy.
Common occupational allergens in healthcare workers include nickel, perfume/fragrance, rubber antioxidants, antiseptics, antibacterial soap, and preservatives.
Latex allergy typically results in immediate redness and swelling of the hands when donning gloves. Diagnosis may be confirmed by prick tests and specific IgE tests.
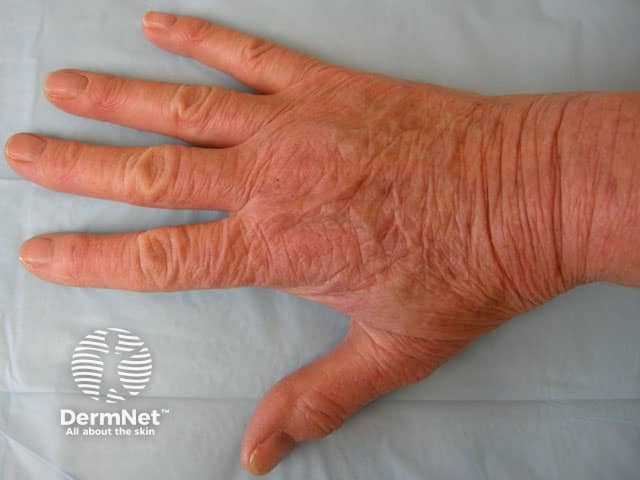
Hand dermatitis caused by gloves
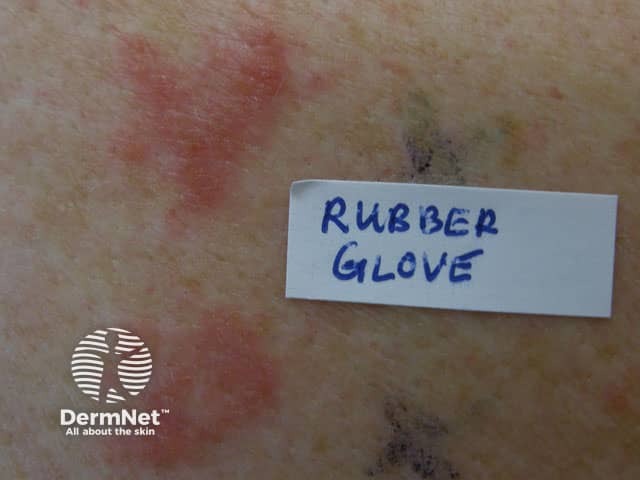
Positive patch tests to the gloves
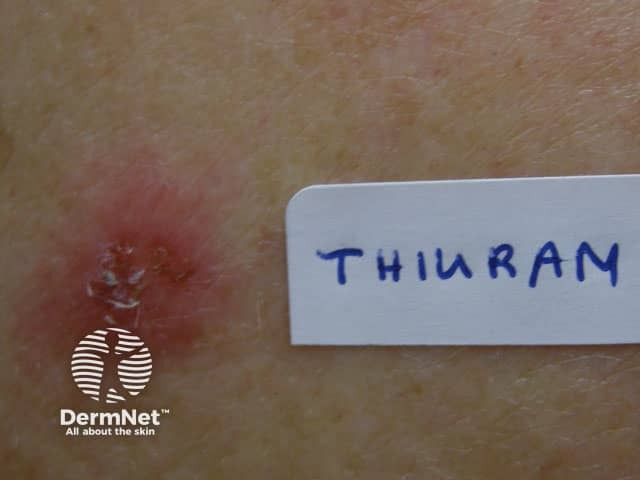
Positive patch test to thiuram, rubber antioxidant
What is the treatment for hand dermatitis?
Treatment of hand eczema includes:
- Minimising contact with irritants
- Avoiding known contact allergens
- Optimising skin barrier with suitable emollients during work and at home
- Courses of potent topical corticosteroids for flare-ups
- Antibiotics for secondary infection.
References
- Araghi F, Tabary M, Gheisari M, Abdollahimajd F, Dadkhahfar S. Hand hygiene among health care workers during COVID-19 pandemic: challenges and recommendations. Dermatitis. 2020;31(4):233-7. doi:10.1097/DER.0000000000000639 PubMed
- Tanner J, Dumville JC, Norman G, Fortnam M. Surgical hand antisepsis to reduce surgical site infection. Cochrane Database Syst Rev. 2016;(1):CD004288. doi:10.1002/14651858.CD004288.pub3. Journal
On DermNet
- Skin problems in healthcare personnel
- Gloves for hand protection
- Hand rubs
- Surgical gloves
- Hand dermatitis
- Patch tests
- Rubber antioxidant allergy
- Latex allergy
- Antiseptics
- Skin barrier function
- Antibacterial soap
- Soaps and cleansers
- Emollients and moisturisers
Other websites
- Healthcare careers advice – Skin@Work, Occupational Dermatology Research and Education Centre, Victoria, Australia
- Hand Hygiene – Waitemata District Health Board, New Zealand
- Looking After Your Hands at Work in Healthcare — Occupational Health and Wellbeing (UK)
