Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Introduction
Demographics
Causes
Clinical features
Variation in skin types
Complications
Diagnosis
Differential diagnoses
Treatment
Outcome
Atopic hand dermatitis (also known as atopic hand eczema) is a multifactorial inflammatory condition affecting the fingers, hands, and wrists of an atopic individual. Atopic dermatitis is the most important risk factor for chronic hand dermatitis.
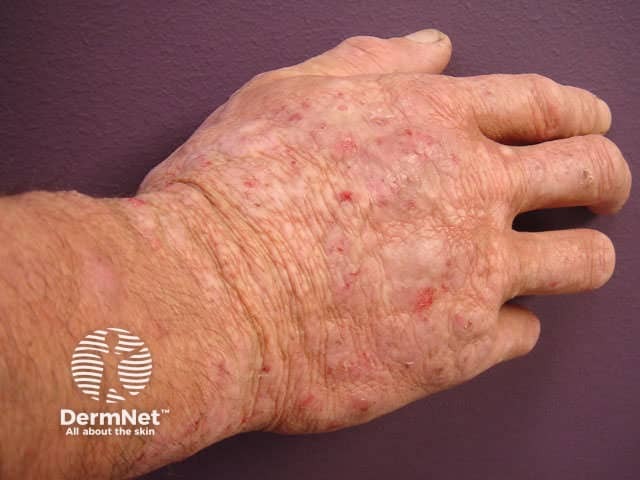
Atopic dermatitis
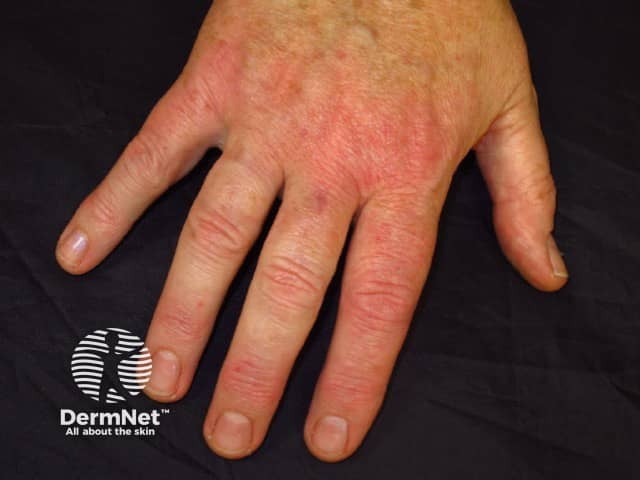
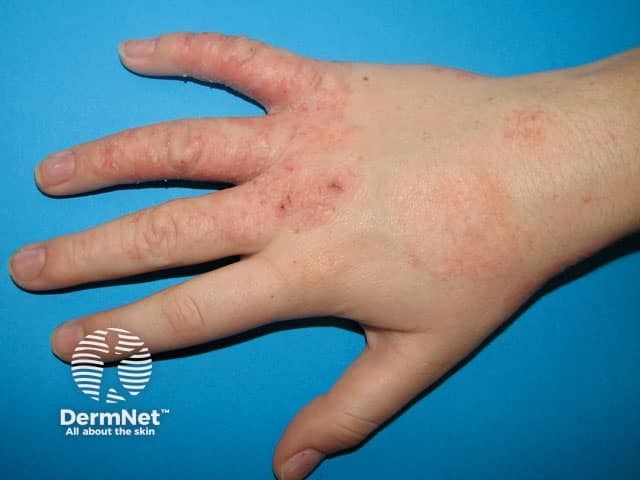
See more atopic hand dermatitis pictures
Atopic hand dermatitis occurs in at least 50–60% of people with active atopic dermatitis, including children. The prevalence of hand involvement increases with age, with hand dermatitis detected in 30–40% of atopic babies and toddlers (age 0–2 years), 55% of atopic children aged 3–12 years, and 65% in those aged over 12 years. This is probably due to increased exposure to irritants. Two-thirds of patients report developing hand dermatitis within one year of the onset of the atopic dermatitis.
Atopic hand dermatitis is multifactorial with inherited and environmental factors contributing to skin barrier dysfunction and immune system dysregulation.
Skin barrier function in atopic dermatitis is impaired due to a deficiency in or defective function of filaggrin, increasing transepidermal water loss (TEWL), and the risk of contact dermatitis and infection.
Atopic hand dermatitis has increased Th2 activation and production of IL-4, IL-13, IL-31, CCL17, CCL18 and CCL22.
Irritant contact dermatitis more commonly complicates atopic hand dermatitis than allergic contact dermatitis. Water exposure is a frequent trigger reported to aggravate atopic hand dermatitis.
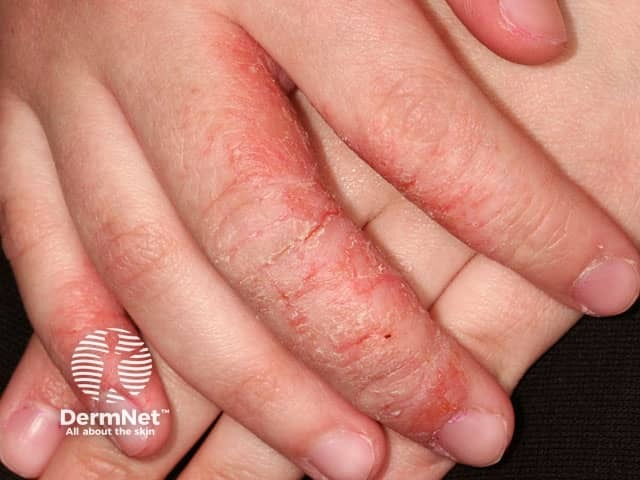
Atopic irritant hand dermatitis
Atopic hand dermatitis preferentially affects the backs of the hands (90%) and fingers (70%), and both aspects of the wrists (50-60%). Involvement of the palmar aspect of the hands and fingers is less common (30%). Atopic hand dermatitis commonly presents with pruritus and dryness, but may include other symptoms such as stinging, burning, and pain. Vesicular hand dermatitis or nummular dermatitis are uncommon presentations. Weeping and crusting can affect the skin surface.
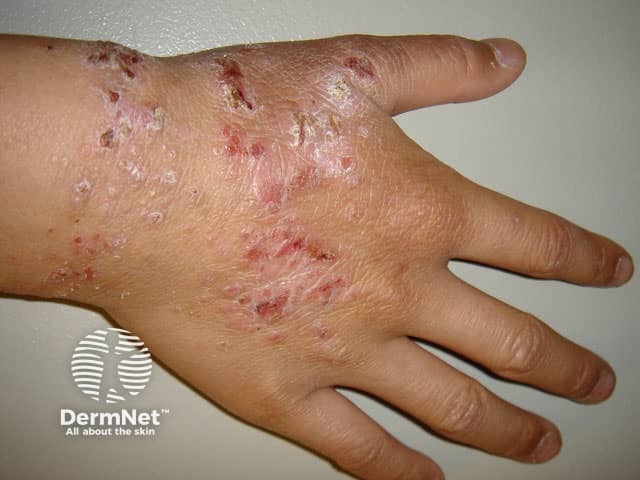
Chronic lichenified atopic hand dermatitis on the back of the hand and wrist
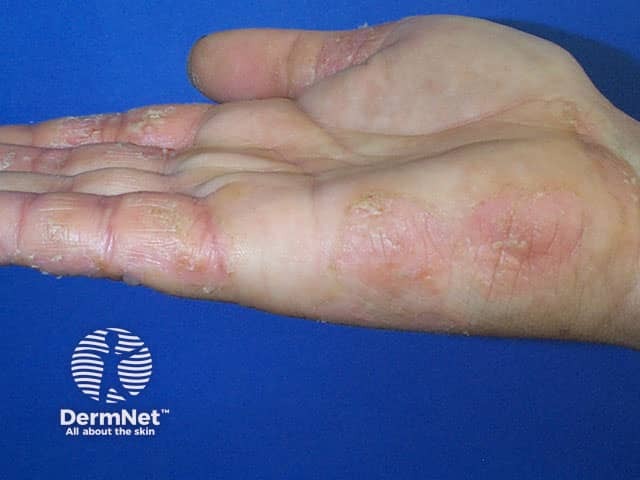
Atopic hand dermatitis involving the palmar aspect of the fingers and side of hand
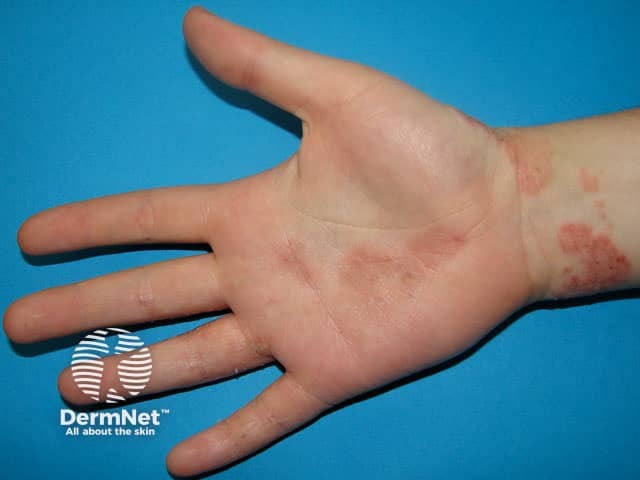
Atopic hand dermatitis involving the volar wrist and palm of hand
Clinical signs include:
However, there are no specific morphological features to distinguish hand dermatitis due to atopic dermatitis from other aetiologies, although the distribution may give a clue. Skin signs that suggest atopic hand dermatitis include hyperlinear palms, keratosis pilaris, and changes of atopic dermatitis elsewhere.
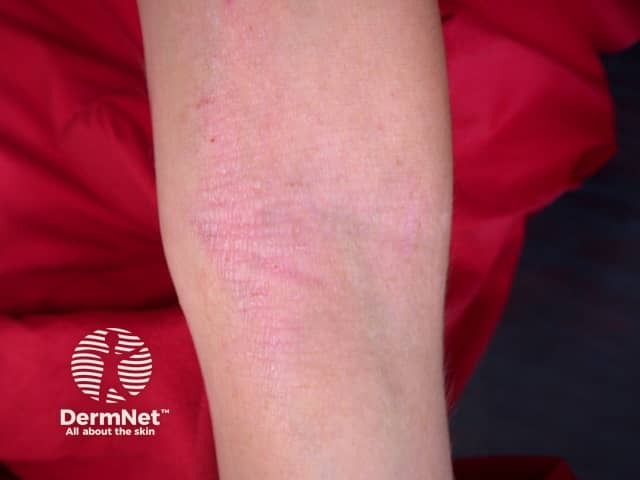
Atopic dermatitis: flexural involvement
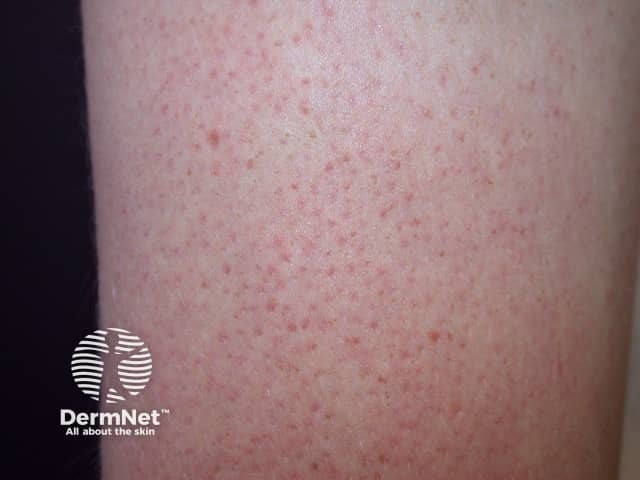
Atopic dermatitis: keratosis pilaris
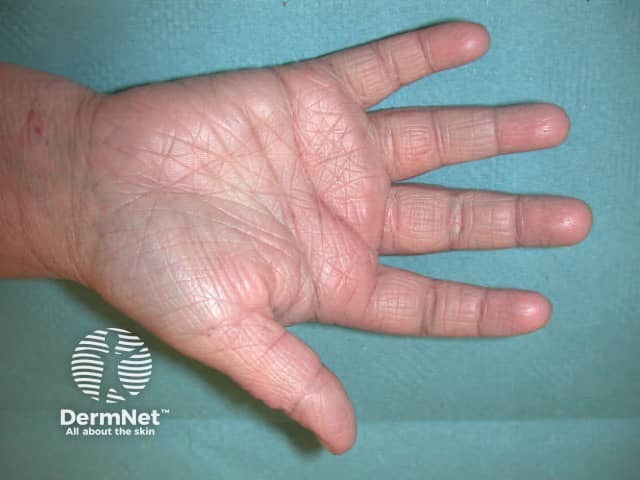
Atopic dermatitis: hyperlinear palm
Nail changes associated with dermatitis involving the distal fingers include coarse pitting, transverse ridges/grooves, and loss of cuticle.
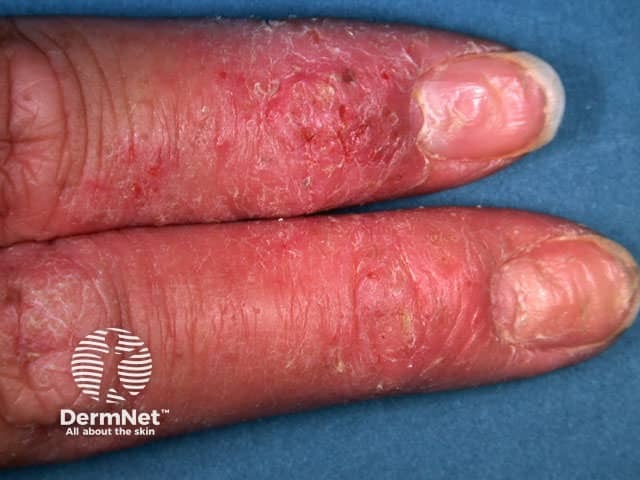
Transverse nail ridging with atopic dermatitis of the distal fingers
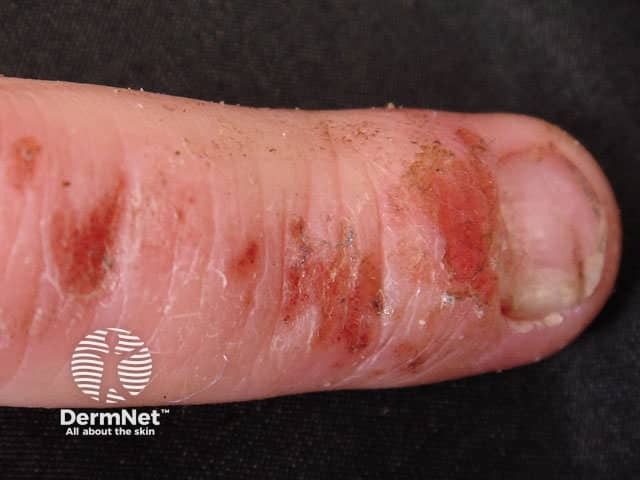
Atopic dermatitis on the finger with nail changes
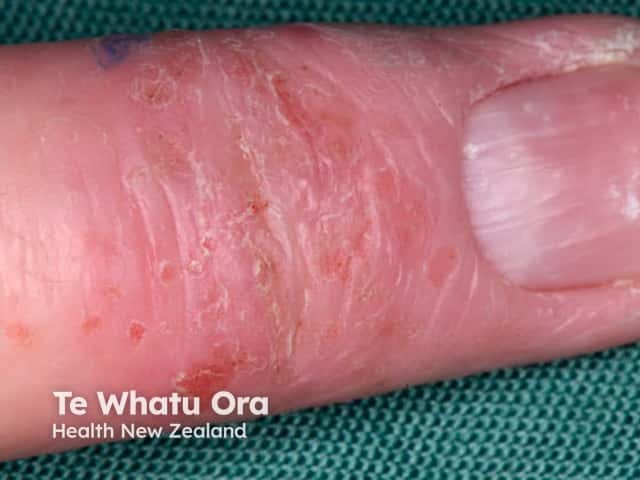
Longitudinal nail ridging and pitting with atopic dermatitis of the distal finger
Atopic hand dermatitis in skin of colour shows less obvious erythema and more postinflammatory hyperpigmentation than in white skin, and the overlying scale is often a grey colour.
[see also Complications of atopic dermatitis]
Atopic hand dermatitis is usually a clinical diagnosis based on a history of atopy and exclusion of other diagnoses. Assessment should include looking for aggravating factors such as exposure to irritants and allergens at home and at work.
Investigations may include:
Obsessive hand care is essential and is required long-term to minimise recurrence or flares due to environmental factors. Advice should be sought before commencing work in an occupation involving wet work or exposure to chemicals such as hairdressing or healthcare.
For severe or treatment-refractory atopic hand dermatitis:
Prompt treatment is recommended as hand dermatitis tends to become chronic. Patients are particularly prone to developing irritant contact dermatitis, but have the same risk of developing allergic contact dermatitis as the general population. Moderate to severe dermatitis is a strong predictor of persistent disease.