Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Juhee Roh, Medical Student, University of Auckland, Auckland, New Zealand. DermNet Editor in Chief: Adjunct A/Prof Amanda Oakley, Hamilton, New Zealand. Copy edited by Gus Mitchell/Maria McGivern. July 2019. Minor update October 2025
Introduction
Indications
How it works
Mechanism
Contraindications
Side effects and risks
Precautions
Hyperbaric oxygen is the breathing of pure oxygen at increased atmospheric pressure. It is a primary or adjunctive treatment for carbon monoxide poisoning, severe decompression sickness, arterial gas embolism, and chronic wounds [1].
There are over 1,200 hyperbaric facilities in the United States, but hyperbaric oxygen is less widely available elsewhere [2].
Hyperbaric oxygen therapy is primarily used to treat patients with:
Carbon monoxide poisoning can occur on inhaling combustion fumes, especially in an enclosed space. Occupations at risk include firefighters, miners, and people exposed to a charcoal or gas fire indoors with inadequate ventilation [4,5].
Decompression sickness, more commonly referred to as 'the bends', is a condition where dissolved nitrogen in the blood and tissues forms bubbles during a move from high to low pressure, causing muscle and joint pain. It occurs most commonly in scuba or deep-sea divers breathing compressed air. It also occurs at high-altitude or during deep unpressurised air travel [6].
An arterial gas embolism is the entry of an air bubble into the arterial systemic circulation, which can block blood vessels. It can occur during decompression, such as in divers, high-altitude aviators, and astronauts [7]. In divers, the presence of a patent foramen ovale (a hole in the heart that usually closes after birth) is known to increase the risk for arterial gas embolism [1]. Air can also be directly introduced into the circulation during arterial catheter placement, and cardiac, neurological, and otolaryngological (ear, nose, and throat) surgery [1].
Poor wound healing can be due to local, regional, systemic, or miscellaneous causes. It can occur with tissue ischaemia, active bacterial skin infection, arterial and venous insufficiency, diabetes mellitus, exposure to radiation, smoking, and the use of vasoconstrictive drugs [8].
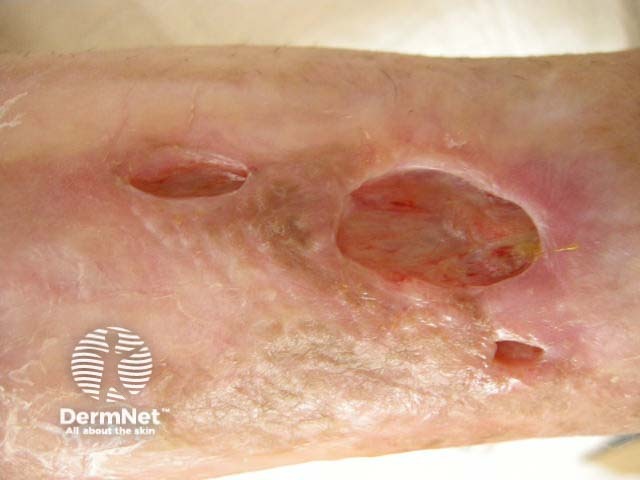
Chronic ulcer before hyperbaric oxygen
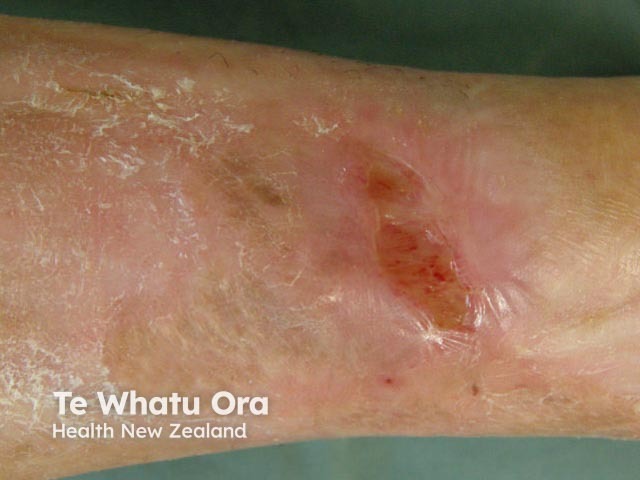
Chronic ulcer after hyperbaric oxygen
Hyperbaric oxygen may be used to treat a diverse range of medical conditions, including:
Hyperbaric oxygen can improve healing after acute traumatic crush injury and compartment syndrome (a pressure buildup in the muscles), resulting in fewer skin flaps, grafts, and amputations [12,13]. There is insufficient evidence to support the use of hyperbaric oxygen for burns [14,15].
The use of hyperbaric oxygen for soft tissue radionecrosis (degeneration of the tissues due to radiation exposure) and osteoradionecrosis (bone degradation due to radiation exposure) is controversial [16–20]. The current guidelines for prevention and treatment recommend 20–30 preoperative 90-minute sessions of hyperbaric oxygen at 2.4 atmospheres (atm) followed by 10 postoperative sessions [17].
Hyperbaric oxygen is used as an adjunctive treatment for aggressive soft tissue infections, such as clostridial myonecrosis (gas gangrene), necrotising fasciitis, and Fournier gangrene [21–27]. It should be commenced early, with 2–3 daily 90-minute sessions at 3 atm [17]. It is unclear whether hyperbaric oxygen therapy is useful for cutaneous soft tissue and rhinocerebral mucormycosis (zygomycosis), actinomycotic brain abscesses, or refractory osteomyelitis [1].
Hyperbaric oxygen is used as an adjunctive therapy to treat non-healing ulcers and skin grafts and to promote wound healing, although there is limited evidence to support its routine use [28–30]. Patients who require skin grafting or reconstructive flaps in areas with compromised blood flow, previous radiation therapy, or previous graft failure may benefit from prophylactic treatment.
Many other diseases have been treated with hyperbaric oxygen without evidence to support the treatment. Further research is required to confirm any benefits and justify its substantial costs and potential risks [1,31].
Hyperbaric oxygen therapy does not usually require hospitalisation so can usually be performed as an outpatient procedure. The specific details of treatment will depend on the hyperbaric oxygen facility and the indication requiring therapy.
Hyperbaric oxygen therapy involves breathing 100% pure oxygen in either a monoplace or multiplace chamber.
Pressures of 2.5–3.0 times normal atmospheric air pressure are generally recommended for both types of chamber [32].
The monoplace chamber is designed for one person and is appropriate for the treatment of a chronic medical condition in a stable patient [9]. The patient lies on a table that slides into a clear plastic tube, similar to a magnetic resonance imaging (MRI) machine [3].
The multiplace chamber is designed for two or more people and allows close monitoring of a critically ill patient [1,31]. The large chamber resembles a hospital room and the patient may sit or lie down. Oxygen is received through a mask or through a transparent, lightweight hood [3,31].
The mechanism of action depends on the condition being treated. See below for details.
Carbon monoxide has 200–250 times greater affinity to haemoglobin than oxygen, reducing the oxygen-carrying capacity of the blood [1]. The normal half-life of carboxyhaemoglobin is 4–6 hours; hyperbaric oxygen therapy reduces its half-life to 15–30 minutes [33,34].
According to Boyle’s law (the relationship between gas concentration, volume, and pressure), the volume of nitrogen bubbles decreases by approximately two-thirds at 3.0 atm. Hyperbaric oxygen therapy reduces the size of nitrogen gas bubbles and replaces inert nitrogen with oxygen [9]. The residual nitrogen is metabolised in the tissues.
Hyperbaric oxygen therapy achieves its therapeutic effect by increasing the oxygen delivered to tissues.
The concentration of oxygen dissolved in plasma at sea level is 0.3 mL/dL. Applying the principles of Henry’s law (the weight of gas dissolved in a liquid is proportional to the pressure of the gas upon the liquid), hyperbaric oxygen administered at 3.0 atm results in a dissolved plasma oxygen concentration of 6 mL/dL [1]. The delivery of oxygen in high concentration to tissues can restore tissue function, stimulate healing, and resist infection [31].
In vitro studies have demonstrated that reactive oxygen and nitrogen species are the key mediators of the bactericidal host response in acute and chronic injury, ischaemia, and inflammation [35–37].
Local hyperoxia (an excessive concentration of oxygen) induces the following effects:
Untreated pneumothorax is an absolute contraindication to hyperbaric oxygen therapy [1]. Relative contraindications include:
Side effects of hyperbaric oxygen therapy may include:
The most common complication of hyperbaric oxygen therapy is middle ear barotrauma (pressure-related trauma), which occurs with an incidence of approximately 2%, and may infrequently result in middle ear effusions and tympanic membrane rupture [41]. Pressure-related middle ear injury can be prevented through autoinflation techniques and placement of tympanostomy tubes in order to remove fluid and reintroduce air to the tubes in the middle ear [41].
The second most common complication is sinus barotrauma, which is usually seen in patients with upper respiratory tract infections or allergic rhinitis [1]. The risk can be minimised by nasal decongestants, steroids, or antihistamines prior to hyperbaric oxygen [41].
Rare complications may include:
Pure oxygen is a serious fire risk.
Potential fire hazards such as lighters, battery-powered devices, and petroleum-based hair and skincare products should be removed prior to the procedure [31].