Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Introduction
Demographics
Clinical features
Diagnosis
Treatment
A knuckle pad is a well-defined thickening over a finger joint. They are also called Garrod pads or holoderma. Knuckle pads are classified as a form of fibromatosis along with Dupuytren contracture (palmar fibromatosis), pachydermodactyly, Ledderhose syndrome (plantar fibromatosis) and Peyronie disease (penile fibromatosis).
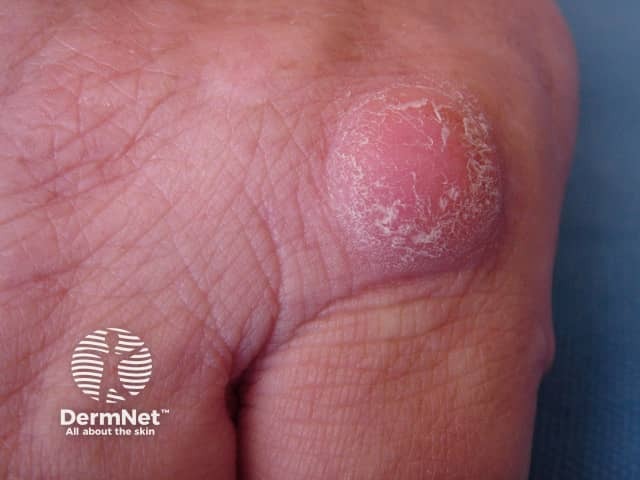
Knuckle pads
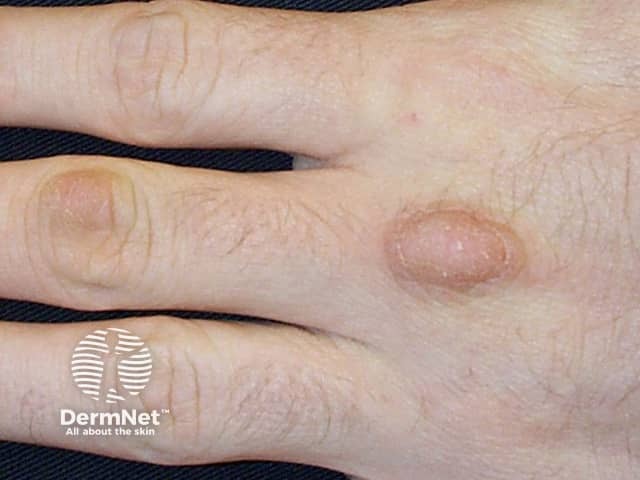
Knuckle pads
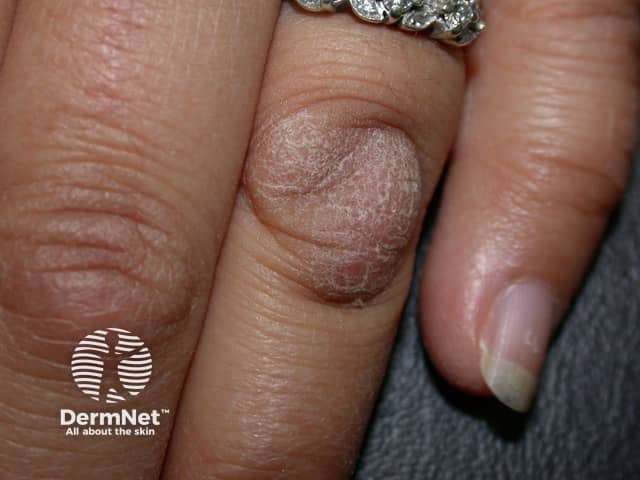
Knuckle pads
Knuckle pads can develop as part of an inherited syndrome, may run in families together with other forms of fibromatosis, or as a sporadic occurrence.
Examples of genetic syndromes that include knuckle pads as a feature are:
There is some debate as to whether true knuckle pads are a response to trauma (calluses). These are more likely to be callosities developing from repetitive pressure or friction, for example, occupational, sporting, finger sucking/chewing, or bulimia nervosa.
Some also attempt to distinguish ‘Dupuytren nodules’ and ‘dorsal cutaneous pads’, the former occurring only in patients with Dupuytren contracture and the latter occurring in both control and Dupuytren contracture populations.
Knuckle pads most commonly become apparent after the age of 30 years. Where there is a family history of knuckle pads, they usually appear at about the same age within a family. But the age of onset varies between families. In children, there is usually no apparent cause.
A knuckle pad is more often located over a proximal interphalangeal (second) joint than over a knuckle (metacarpophalangeal/first joint) or distal interphalangeal (third) joint.
The pad may be seen over just one joint or many. The hands are most commonly affected but other joints, such as the feet and knees, may be involved.
Knuckle pads are well-defined, smooth, firm thickenings that can be flat or more obvious and dome-shaped. They generally do not cause any symptoms but can be tender or painful.
Usually, knuckle pads are diagnosed clinically. However, there are several other conditions that may cause confusion including granuloma annulare, pachydermodactyly, rheumatoid nodules, and synovitis resulting in swollen joints.
Ultrasound can be useful for distinguishing knuckle pads from synovitis.
Should a skin biopsy be performed, histology shows hyperkeratosis and acanthosis of the epidermis and thickening of the dermis and individual collagen fibres. When associated with a keratin 9 gene mutation, as in epidermolytic palmoplantar keratoderma, suprabasal epidermolysis is also seen.
In general, treatment is not required for a knuckle pad. Avoidance of repetitive behaviour if possible may improve the situation. Moisturisers may be useful if the knuckle pads are hyperkeratotic. Surgery has been used, but can be complicated by the development of keloid scars.