Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Authors: Dr Dushyanth Gnanappiragasam, Dermatology Specialist Registrar; Dr Karen Harman, Consultant Dermatologist, University Hospitals of Leicester NHS Trust, United Kingdom. DermNet Editor in Chief: Adjunct A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy edited by Gus Mitchell. January 2020.
Introduction Demographics Causes Clinical features Differential diagnoses Diagnosis Treatment Outcome
Pachydermodactyly is a benign digital fibromatosis presenting as a progressive asymptomatic periarticular thickening, most commonly around the proximal interphalangeal joints. Palmar and distal interphalangeal (DIP) or metacarpophalangeal (MCP) joint involvement has been described.
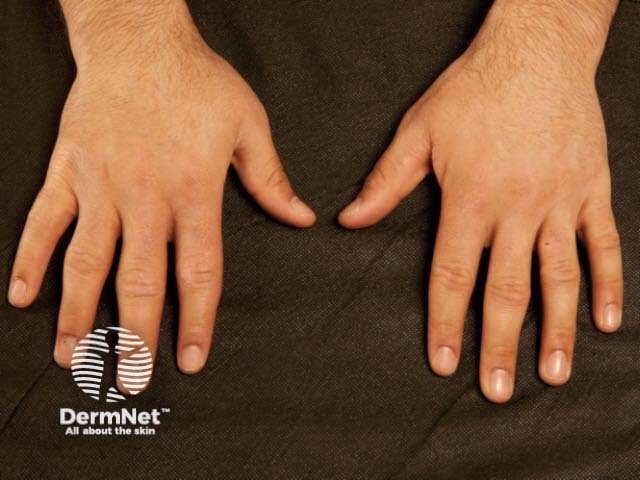
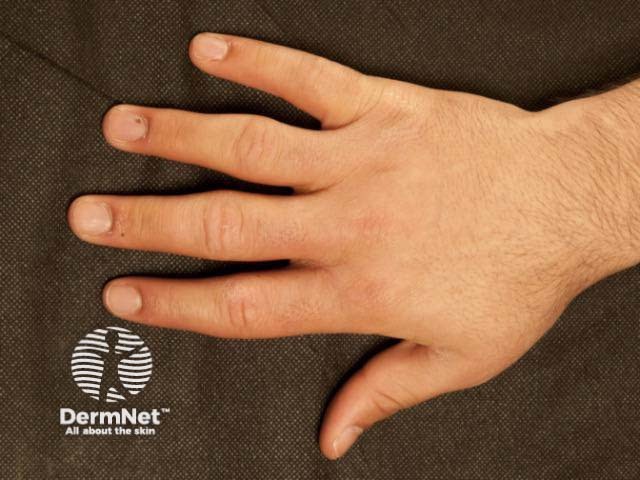
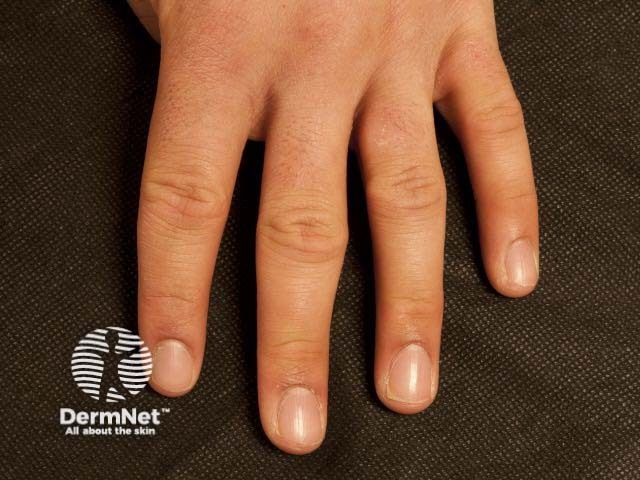
Pachydermodactyly most commonly occurs in adolescents and young men. The affected male to female ratio is 4:1 [1,2].
The exact cause of pachydermodactyly is not fully understood. It has been linked to repetitive mechanical stimulation in genetically predisposed individuals. Hormonal factors may also have an influence as illustrated by the predominance in male individuals and symptoms appearing at the age of puberty.
Common triggers identified have been habits such as interlacing, stretching, rubbing and cracking of the fingers, and increased mechanical irritation related to computer use, work, professional sport, and musical activities.
Associations with tuberous sclerosis and Ehlers-Danlos syndrome are reported [1,2].
The pathophysiology is thought to be due to deposition of abnormal collagen in the dermis, especially loose strands of type III and type V collagen.
Pachydermodactyly presents as a symmetrical soft-tissue thickening of the skin on the sides of the proximal interphalangeal joints, most commonly affecting the second (index), third (middle) and fourth (ring) fingers of both hands. The thumbs and fifth fingers are rarely involved. Some patients may also have overlying hyperkeratosis, lichenification, and hyperpigmentation. Movement of the fingers is not restricted. Pachydermodactyly is not associated with symptoms such as pain or stiffness. There is no evidence of a synovitis.
The toes are never affected.
Other conditions that may be considered in the differential of diagnosis of pachydermodactyly include:
The lack of symptoms and other signs make the following conditions unlikely:
Diagnostic criteria have been proposed [2]:
Investigations for inflammatory arthropathies may include:
Features seen in skin biopsies include [1,3]:
Inflammation is typically absent.
Pachydermodactyly may reverse or resolve with cessation of mechanical stimulation if any.
Intralesional corticosteroid (triamcinolone) and surgical resection have been trialled in severe cases with some benefit.
Overall, pachydermodactyly remains stable. Permanent joint deformities or damage are rarely observed.