Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Authors: Dr Anne-Marie Aubin and Dr Paul Chee, Department of Dermatology, John Hunter Hospital, New South Wales, Australia (2023)
Previous contributors: Dr Ben Tallon, Dermatology Registrar, New Zealand (2005)
Reviewing dermatologist: Dr Ian Coulson
Edited by the DermNet content department
Introduction Demographics Causes Clinical features Variation in skin types Complications Diagnosis Differential diagnoses Treatment Prevention Outcome
Marine stings include venomous or contact stings from any marine creature.
The main culprits causing contact stings are jellyfish and jellylike animals, fire coral, sponges, hydroids, and sea anemones; while penetrating injuries are caused by sea urchins, cone shells, and venomous fish. Venomous fish include stingrays, stonefish and zebrafish, lionfish and scorpionfish, and catfish.
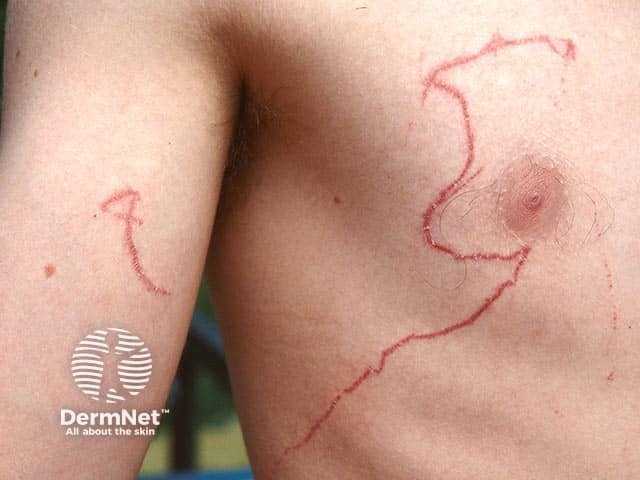
A serpentine configuration to box jellyfish stings (MAS-patient1)
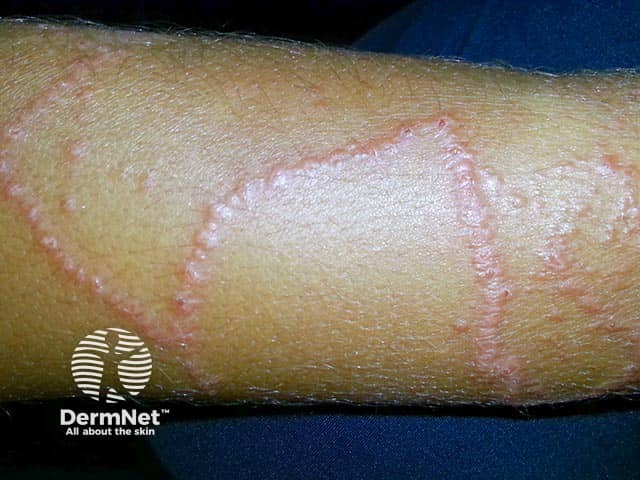
Box jellyfish stings in skin of colour
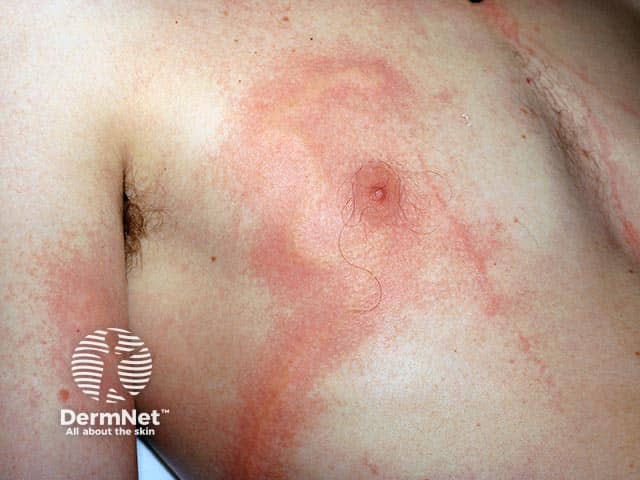
Urticated erythema in box jellyfish stings (MAS-patient1)
Marine wounds and stings occur amongst fishermen, swimmers, scuba divers, surfers, and aquaculture workers.
Jellyfish are most prevalent in calm warm seawater, sandy beaches, and harbours during the summer months, although they are also seen in other circumstances. Sea anemones, fire coral, sea urchins, sponges, and venomous fish are also commonly found in shallow coastal waters, as well as reefs.
Jellyfish cause the majority of marine stings.
Jellyfish stings occur when their tentacles contact human skin. Nematocysts (cells that line the jellyfish tentacles) fire poison-filled darts as they touch the skin. The severity of the sting depends on the amount of tentacle contact and the type of venom.
Corals, sea anemones, and hydroids also use nematocysts to sting, typically producing intense and sustained local skin reactions, characterised by burning pain.
Venomous fish, stingrays, and sea urchins all have venomous spines in their dorsum, ventral surface, or tail which can inject venom as they penetrate human skin. The venom typically stings more than the penetrating wound and effects are typically local, although very painful.
Sponges use structural elements in their skeleton called spicules to form small perforations from which chemicals or toxins can be extruded into human skin. Irritant or allergic contact reactions typically result (‘sponge dermatitis’).
When picked up or handled, blue-ringed octopus and cone shells envenomate via a bite (sometimes painless) and a dart-like apparatus respectively, delivering tetrodotoxin and conotoxins (nerve channel toxins).
Cuts and scratches among fishermen, swimmers, and surfers often fail to heal, which may relate to repeated exposure to seawater and foreign material such as sand in the wound.
Clinical features of marine stings include:
Irukandji leaves a small erythematous area or scarcely any skin marks, a diagnostic clue in itself. Irukandji syndrome may be delayed (20–30 mins) with severe generalised cramping pain and systemic effects (tachycardia, agitation, hypertension, and pulmonary oedema) and is potentially lethal.
Stonefish produce a single severely painful foot puncture with rapid surrounding oedema, in a tropical coral reef setting and typically no sighting of what caused the injury. Sea urchin and stingray injuries also typically involve the foot or ankle.
Other marine injuries (eg, cuts and scratches) are most often located on the feet, ankles, and back of the hands. They are often slow to heal and may be called ‘sea ulcers’. Peripheral callus formation may occur, similar to diabetic foot ulcer (even in non-diabetics).
Darker Fitzpatrick skin types may be more prone to keloid and hypertrophic scarring following injury.
Potential complications of marine stings include:
Diagnosis of marine stings relies on the sighting of the creature, historical clues, and clinical features. Enquire if the animal (or pieces of it) was obtained, or if photographs were taken. All significant jellyfish and spiny fish envenomations produce immediate and severe pain.
Dermoscopy may be used to identify the type of jellyfish sting with a peculiar finding of ‘serpentine ulceration’ with brown dots indicative of a P. noctiluca sting.
A definitive diagnosis of the jellyfish type can be made using sticky tape or a skin scraping to identify the characteristic nematocysts in the keratin layer. Skin scrapings are placed in a formalin solution (1–4%) and then examined under a microscope at x40 objective.
Toxicology advice can be obtained from local poison advisories (eg, the Australian Poisons Information Centre). Antivenoms exist for box jellyfish, stonefish, and sea snake envenomation.
Most marine stings are minor and do not require any medical intervention. Some bites and stings can result in serious tissue damage, penetrating injury, and systemic toxicity.
Death from a marine sting is rare and is largely due to cardiac arrhythmias caused from the toxins released by the box jellyfish, Irukandji jellyfish, or a major stingray trauma. Rare deaths have occurred from sea snake, cone shell, and blue-ringed octopus envenomation, which may cause paralysis and respiratory failure.
Marine stings rarely cause permanent scarring. Hyperpigmentation or hypopigmentation can remain for up to two months. Consider tetanus prophylaxis and treatment of secondary infection.