What is Morbihan disease?
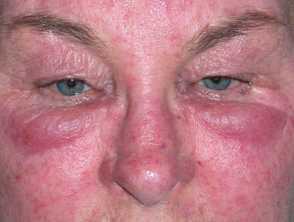
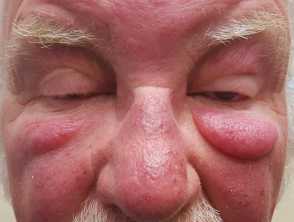
Morbihan disease was first described in 1957 by French dermatologist Robert Degos, and is characterised by a firm oedema on the upper portion of the face. Although generally considered as a refractory and chronic form of rosacea, Morbihan disease may exist in the absence of other features of rosacea, and thus may represent a separate disease process.
Morbihan disease
Click to see more images of Morbihan disease
Who gets Morbihan disease?
Morbihan disease usually affects Caucasians in the third and fourth decade of life.
There are only two reports of the disease in skin of colour [1]. It is more common in women than men.
What causes Morbihan disease?
The lymphoedema of Morbihan disease follows the loss of lymphatic vessel wall integrity and the passing of fluid through the vessel. [2,3] The cause is unknown, but possible causes have been speculated, such as:
- Local dysregulation of lymphatic vessels
- Lymphatic obstruction by granulomas and histiocytes (a type of immune cell) [3]
- Chronic inflammation due to acne, rosacea or contact dermatitis that destroys supporting connective tissue around dermal lymphatic vessels [2,3].
What are the clinical features of Morbihan disease?
Morbihan disease is characterised by erythema and solid, non-pitting oedema.
- The onset of Morbihan disease is slow, with intermittent swelling eventually becoming permanent infiltration of the skin.
- It affects the periorbital region, the forehead, the glabella, cheeks, and nose.
- Morbihan disease is not painful or itchy, but may be aggravated by sun exposure.
- Other features of rosacea may be present, like telangiectasia, flushing, papules and pustules [4,5].
What are the complications of Morbihan disease?
Persistent facial oedema leads to:
- Distortion of facial contours
- Vision impairment due to a narrowed visual field
- Psychosocial stress
- Cosmetic concerns.
How is Morbihan disease diagnosed?
There are no biochemical or histopathological findings specific to Morbihan disease.
Biopsy should be conducted to rule out other diagnoses. Nonspecific histopathology findings include:
- Perivascular dermal oedema
- Lymphohistiocytic periadnexal infiltrate
- Numerous mast cells confirmed by Giemsa stain
- Mucin confirmed by colloidal iron stain
- Dilation of lymphatic vessels
- Non-caseating granulomas
- Sebaceous gland hyperplasia [6].
Patch testing may also be arranged to exclude allergic contact dermatitis.
What is the differential diagnosis for Morbihan disease?
Differential diagnosis for Morbihan disease includes other granulomatous and inflammatory facial conditions [7,8]. Conditions to consider include:
- Sarcoidosis — characterised by epithelioid granulomas on histology and a positive serum angiotensin converting enzyme (ACE) test; it can be localised to the skin or systemic
- Orofacial granulomatosis — characterised by painless lip swelling, granulomas on histology, mouth ulcers, mucosal tags, and lingua plicata
- Systemic lupus erythematosus — where cutaneous findings include malar rash ('butterfly' rash), maculopapular rash, mucosal ulcers and photosensitivity.; this can result in systemic disease affecting the joints, lungs, heart, kidneys, brain, blood and nervous system.
- Foreign body granuloma — characterised by reddish-brown papules, nodules and plaques in response to tattoo, bovine collagen injection, silicone or paraffin injection, retained sutures, etc
- Scleroedema of Buschke — characterised by the symmetrical hardening of the skin of the neck and upper back typically associated with diabetes mellitus; there are caseating epithelioid granulomas containing acid-fast bacilli.
- Lupus vulgaris (cutaneous tuberculosis) — characterised by reddish-brown ‘apple jelly’ nodules.
- Cutaneous pseudolymphoma — various conditions can simulate cutaneous lymphoma.
What is the treatment for Morbihan disease?
Morbihan disease is frequently refractory to treatment.
Medical treatments
The antibiotic metronidazole and the tetracyclines, minocycline and doxycycline, are effective for inflammatory rosacea. Other options are:
- Isotretinoin 10–20 mg daily for 3–6 months
- Ketotifen 1 mg daily [6].
Thalidomide, clofazimine and systemic corticosteroids, such as prednisone, are typically ineffective.
Destructive therapies
Surgical excision of redundant oedematous tissue may be required for a full recovery. Other options are:
- CO2 laser blepharoplasty (laser eyelid surgery)
- Radiotherapy.
Other therapies
Facial massage can be used to improve lymphatic drainage. Contact irritants or allergens should be avoided to aid recovery.