Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Julie Smith MBChB, Dept of Dermatology, Grenlane Hospital, Auckland. Updated by A/Prof Amanda Oakley, February 2016.
Introduction
Demographics
Causes
Clinical features
Diagnosis
Treatment
Scleroedema (American spelling scleredema) is a type of cutaneous mucinosis of unknown cause.
Scleroedema should not be confused with ‘scleroderma’, in which the skin is fibrotic (morphoea and systemic sclerosis).
Scleroedema affects adults. In many cases, people with scleroedema have an underlying systemic disease. These include:
This is unknown.
Scleroedema presents with symmetrical hardening and thickening of the skin. The affected areas are firm and woody plaques, sometimes slightly red or brown and often with a ‘peau d'orange’ (orange-skin) appearance. The face may appear expressionless and there can be difficulty opening the mouth.
There are three types of scleroedema. All three types of scleroedema can restrict movement, but otherwise seldom have serious consequences. Occasionally swallowing and speech can be affected and other organs involved – eyes, tongue, parotid gland, muscles, joints and heart.
Type one is the acute type of scleroedema, and typically starts with an infection, most often Streptococcus pyogenes, the cause of tonsillitis. It mainly affects middle aged women and children. Hardening of the skin of the face and neck quickly develops and spreads to the upper trunk and arms. It usually improves spontaneously over six months to two years.
Type 2 scleroedema is not associated with infection. It starts more slowly and persists. Abnormal levels of an abnormal paraprotein (immunoglobulin) in the blood may occur, sometimes due to multiple myeloma.
Type 3, scleroedema adultorum of Buschke, also called scleroedema diabeticorum, occurs in diabetics, particularly adult men. It is very persistent. The skin of the neck and upper back slowly thickens over months or years.
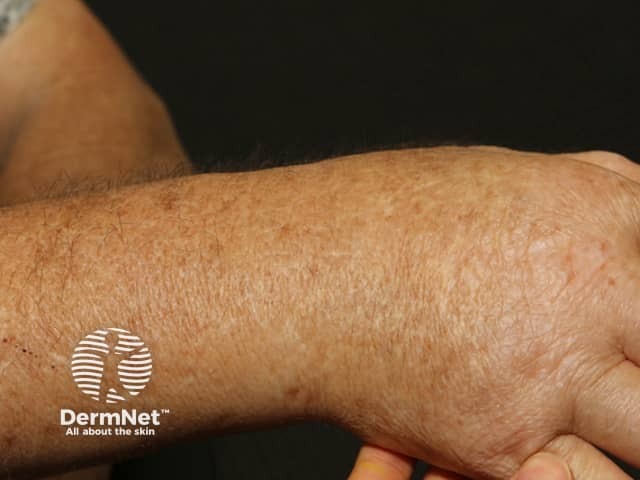
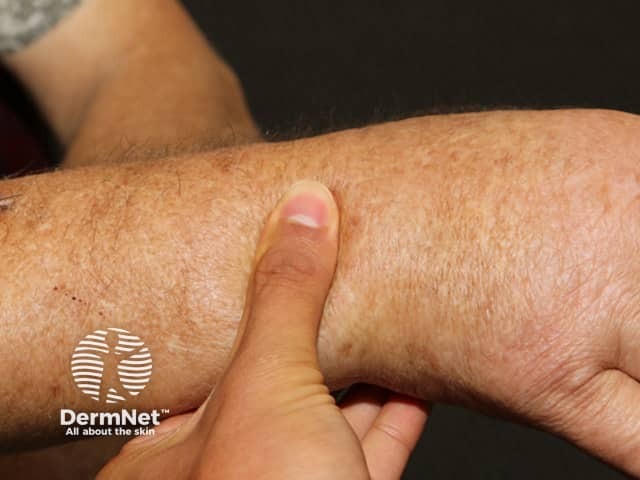
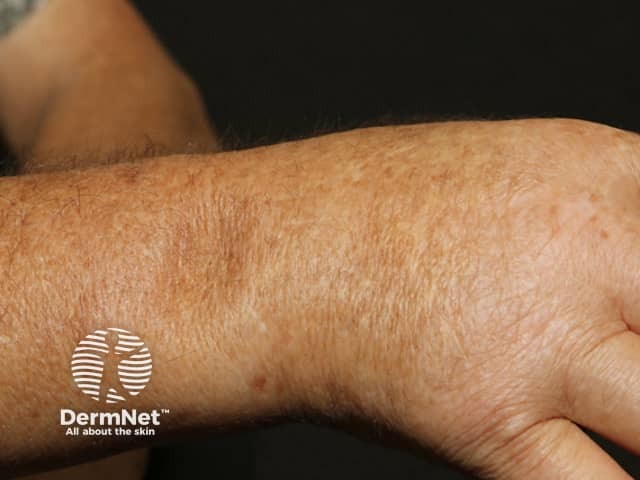

*Images provided by Dr Eugene Tan, Melbourne, Australia.
The diagnosis is confirmed by skin biopsy, which shows mucin deposits between collagen bundles in the dermis.
The best way to treat scleroedema is unknown, because of its rarity. Some benefit has been reported with the following: