Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Lydia Chan, Medical Registrar, Waikato Hospital, Hamilton. Chief Editor: Dr Amanda Oakley, Dermatologist, Hamilton, New Zealand, December 2014.
Introduction Demographics Clinical features Causes Diagnosis Treatment
Progressive macular hypomelanosis is a common skin condition presenting as circular areas of pale skin (hypopigmentation) mostly located on the trunk.
Progressive macular hypomelanosis affects teenagers and adults worldwide. It is more common in people of darker skin colour that light skin colour, and may be more common in women than in men.
Progressive macular hypomelanosis mainly affects the trunk, rarely extending to the arms, legs and/or neck. There are multiple, circular, poorly defined pale and non-scaly spots that merge together.
The patches are not scaly, unlike hypopigmented pityriasis versicolor, which can also cause pale patches on the trunk. They are not preceded by inflammation, unlike postinflammatory hypopigmentation following nummular eczema or psoriasis.
The course of progressive macular hypomelanosis is reported to be variable. Some cases may resolve in 3–5 years. Others remain stable and yet others progress over decades and may then resolve in middle age.
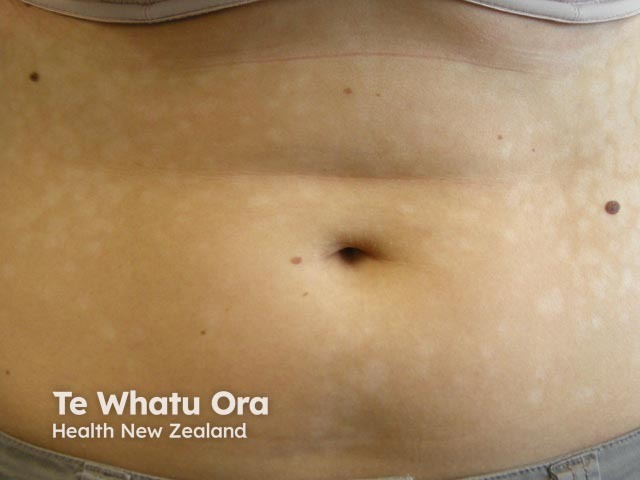
Progressive macular hypomelanosis
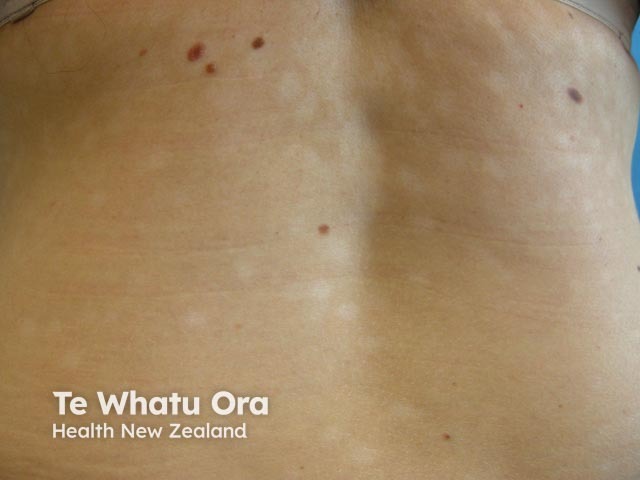
Progressive macular hypomelanosis
The cause of progressive macular hypomelanosis is not known. The acne bacteria, Cutibacterium acnes, have been found in hair follicles of hypopigmented areas and may cause the loss of colour. However, these bacteria have not been found in all patients with progressive macular hypomelanosis. Genetic factors are also thought to be important.
Progressive macular hypomelanosis is usually diagnosed by clinical suspicion and supported by the presence of fluorescence on Wood light examination. The hair follicles fluoresce with a red glow, indicating they are colonised by P. acnes.
Dermoscopy shows poorly-defined white macules with faint reticular pigmentation. The macules are usually not scaly but focal scale is occasionally seen.
Microscopic examination of a skin biopsy shows a reduction in melanin in the the affected skin, with normal numbers of melanocytes (specialised cells that produce melanin). On electron microscopy of affected areas, the melanosomes (the granules that store melanin in the cell) are smaller and aggregated, compared to surrounding skin.
Treatments for progressive macular hypomelanosis include:
Isotretinoin was effective in one case report.
The condition may relapse following treatment.