Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author(s): Hana Numan, Senior Medical Writer, DermNet Staff. Dr Jannet Gomez, PG Student in Clinical Dermatology, United Kingdom, 2016; A/Prof Amanda Oakley, Dermatologist, New Zealand, 1998. Copy edited by Gus Mitchell. February 2022
Introduction
Demographics
Causes
Clinical features
Variation in skin types
Diagnosis
Differential diagnoses
Treatment and prevention
Outcome
Pseudofolliculitis barbae (PFB) is a common inflammatory reaction of the hair follicle, most often on the face as a result of shaving. Also known as “razor bumps” or “shaving bumps”, it can also occur on any site where hair is shaved or plucked, including the axilla, pubic area, and legs.
Folliculitis barbae presents similarly, but is due to infection. Folliculitis barbae and pseudofolliculitis barbae can coexist.
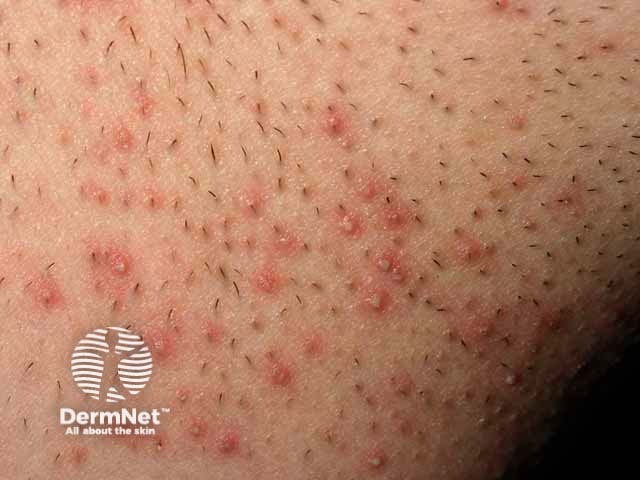
Pseudofolliculitis barbae
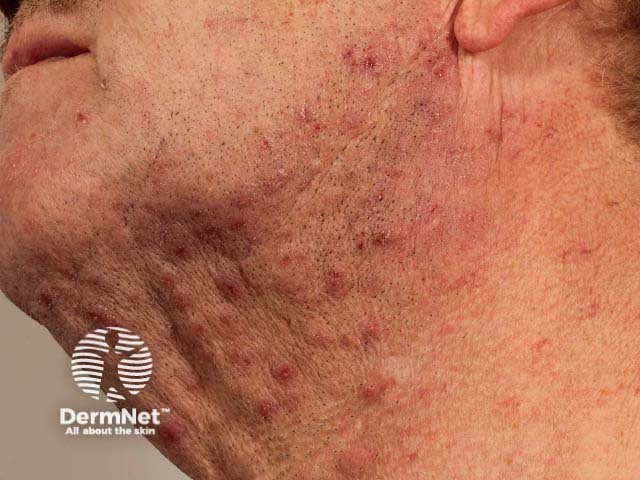
Pseudofolliculitis barbae
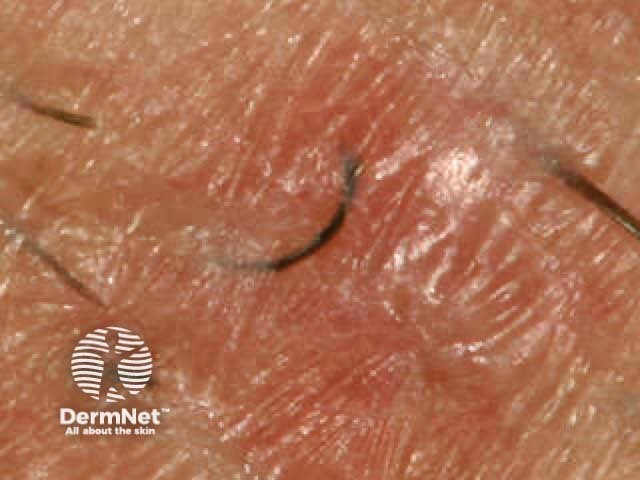
Ingrowing beard hair
Although PFB can occur in men of all races, it predominantly affects men of African ancestry (approximately 45–80%). This is likely due to a greater prevalence of tightly curled, coarse hair in the African population. A study demonstrated that the presence of a single nucleotide substitution in the hair follicle companion layer-specific keratin (K6hf) is an additional risk factor. It can also affect women of all races, especially occurring in the groin.
It is associated with improper shaving technique and is more common with blade razor users compared to electric shavers.
Razor bumps are thought to be caused by intrafollicular or transfollicular penetration of tight curly hair, often of coarse nature. They may also occur in skin folds or scar tissue, allowing straight hair to re-enter.
This often occurs due to close shaving, as cut hair results in a sharp pointed end and may re-enter by either:
This subsequently leads to a foreign body inflammatory reaction. The injured follicles are highly susceptible to infection, causing folliculitis barbae.
Pseudofolliculitis barbae is more common in those with darkly pigmented skin. It is also more likely to occur in those with curly and coarse hair.
What are the complications of pseudofolliculitis barbae?
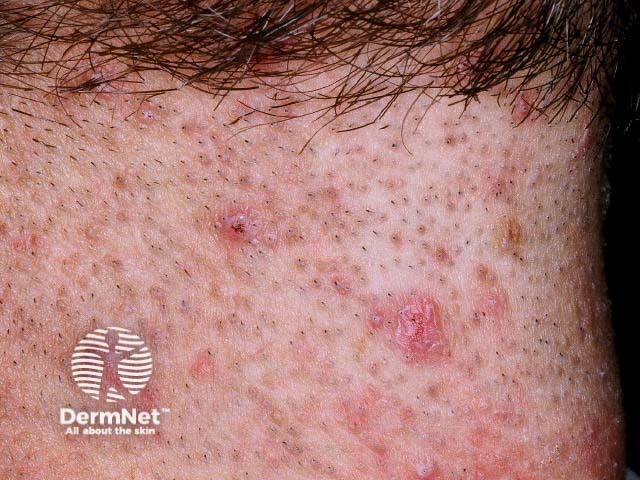
Pseudofolliculitis barbae
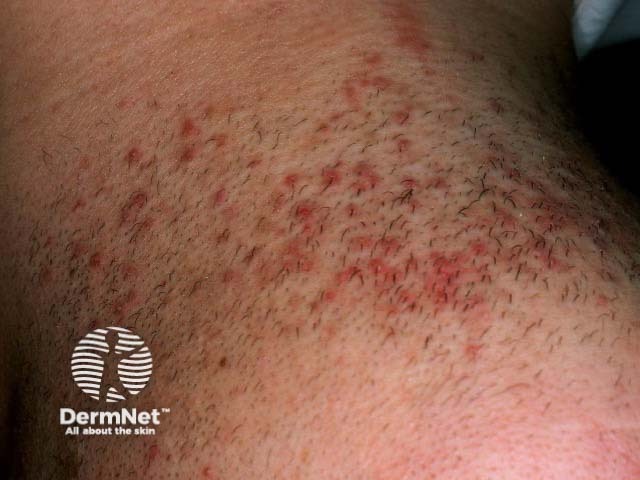
Pseudofolliculitis
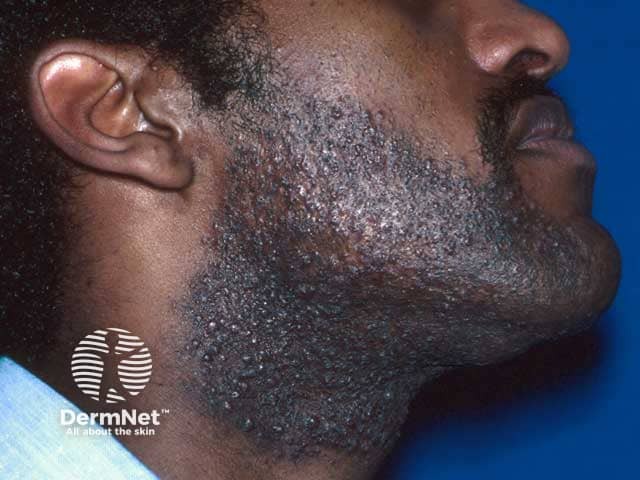
Rounded pigmented papules in the beard area in pseudofolliculitis barbae
Pseudofolliculitis barbae is a clinical diagnosis. Dermoscopy may be used as an aid to visualise ingrown hairs and exclude differential diagnoses.
The safest and most definitive cure is to discontinue shaving activity, thus patients should have the cause of PFB clearly explained to them. This may be unsuitable for many (eg, work, cultural, or personal reasons). If shaving is discontinued, it may take several weeks for the inflammatory response to cease (whilst hairs regrow).
Pseudofolliculitis barbae subsides approximately 4–6 weeks following cessation of the causative hair removal technique (most often shaving). The likelihood of experiencing further razor bumps can be reduced by trialling a different hair removal technique.
If no change is made, the condition will likely persist. Complications such as infection or scarring may arise and further treatment may be required.