Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author(s): Dr Amanda Oakley, Dermatologist, Hamilton, New Zealand, 1998. Updated: Dr Jannet Gomez, Postgraduate Student in Clinical Dermatology, United Kingdom, July 2016; Casey P Schukow, Medical Student, Michigan State University College of Osteopathic Medicine, United States of America, February 2022.
Introduction
Demographics
Causes
Clinical features
Variation in skin types
Complications
Diagnosis
Differential diagnoses
Treatment
Outcome
Folliculitis barbae is an itchy and sometimes tender papulopustular eruption of hair follicles in skin areas prone to shaving, such as the beard-line in men. It also occurs in women who shave their legs and bikini area.
Deep-seated folliculitis barbae is called sycosis barbae and leads to scarring and areas of permanent hair loss.
Folliculitis barbae presents similarly to pseudofolliculitis barbae (PFB), which is a papulopustular foreign body reaction towards curved hair-follicles that penetrate the perifollicular epidermis as they grow out of the skin (ingrown hairs). PFB presents more frequently in post-shaven hair-bearing areas of persons with more curly and coarse hair, as seen in African Americans.
Both conditions may coexist.
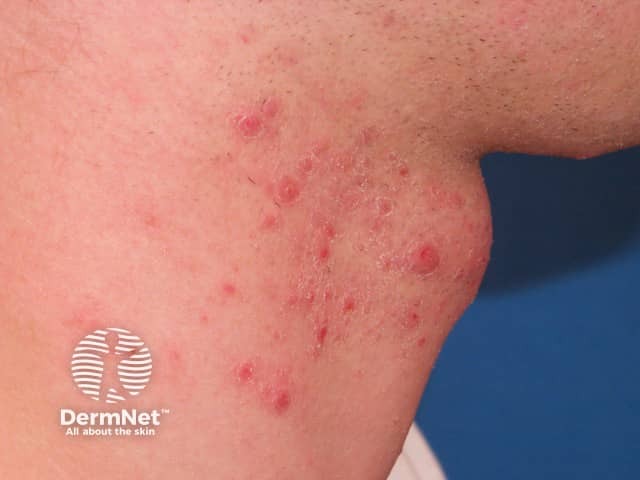
Folliculitis barbae on the neck
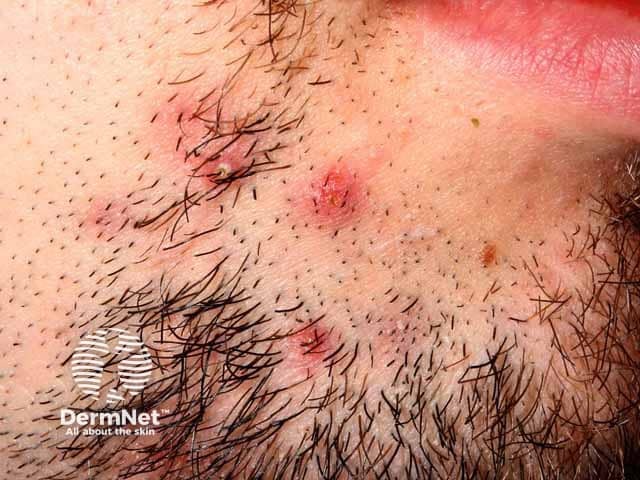
Deeper tender lesions in sycosis barbae
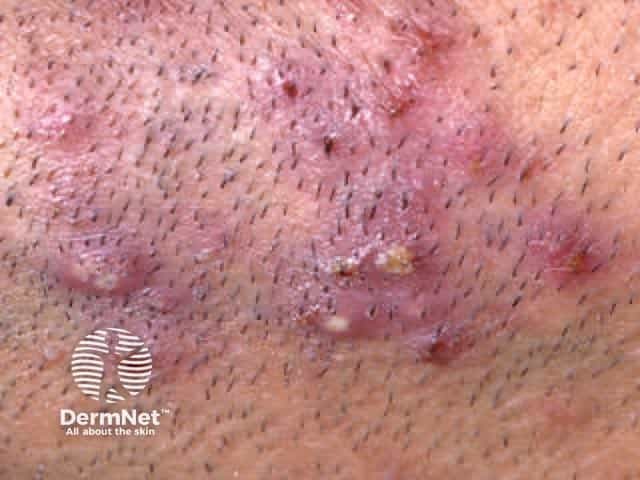
Folliculitis barbae on the chin
Folliculitis barbae most commonly affects recently shaved hair-bearing areas in men (such as the beard-line) of lighter skin types. Folliculitis may also develop after laser hair removal. However, it may also present in individuals who do not shave.
Cases of folliculitis barbae may occur secondary to viral, mycologic, or eosinophilic causes, and may be seen in competitive athletes and immunosuppressed persons.
Folliculitis barbae is most often due to Staphylococcus aureus (S. aureus) colonization of more superficial portions of the hair follicle (for example, the infundibulum) and skin surface. However, cases of herpes simplex and candida folliculitis barbae (folliculitis barbae candidomycetica) have been reported.
Reinfection by S. aureus after successful treatment may suggest persistent colonization of S. aureus within the nasal cavity or on previously used shaving equipment, such as razors.
If the colonization of S. aureus seeds deeper in the skin, it may induce sycosis barbae, which presents as persistent sinus tracts, abscesses, and inflammation deep between hair follicles.
Curlier and coarser hairs of persons with darker skin types (such as African Americans) are more likely to penetrate perifollicular epidermis, causing PFB.
While PFB and folliculitis barbae may co-present in darker skin individuals, finer and straighter hairs in persons with lighter skin types are less likely to cause PFB.
Folliculitis barbae is often a clinical diagnosis and may be aided by dermoscopy.
In cases of refractory folliculitis barbae, pustule and nasal cavity swabs may be necessary to determine bacterial culture/drug resistance and/or other potential aetiologies.
Uncomplicated folliculitis barbae due to S. aureus should respond within 1–2 weeks of treatment with topical antibacterials.
Cases of folliculitis barbae treated swiftly should resolve without any complications. Refractory, untreated, or persistent cases may lead to the development of sycosis barbae and/or permanent scarring, which may improve in appearance over time.