Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Vanessa Ngan, Staff Writer, 2003. DermNet Update August 2021
Introduction
Demographics
Causes
Clinical features
Complications
Diagnosis
Differential diagnoses
Treatment
Outcome
Bacillary angiomatosis is an opportunistic cutaneous and systemic bacterial infection caused by Bartonella quintana and Bartonella henselae usually affecting immunocompromised patients.
Bacillary angiomatosis is seen predominantly with drug-induced immunosuppression, particularly organ transplant recipients, chronic lymphocytic leukaemia, and those with HIV/AIDS. However, otherwise healthy individuals, including children, can also contract the infection such as after major local trauma.
Bacillary angiomatosis is caused by Bartonella (Rochalimaea) quintana and Bartonella (Rochalimaea) henselae, gram-negative intracellular bacteria. Cats are the main reservoir for B henselae, and humans for B quintana. While cat bites and scratches can transmit the infection, fleas are the primary means of transmission, with ticks also serving as a potential vector. B quintana is transmitted by the human body louse (Pediculus humanus) and fleas.
Skin lesions are usually the first manifestation of bacillary angiomatosis.
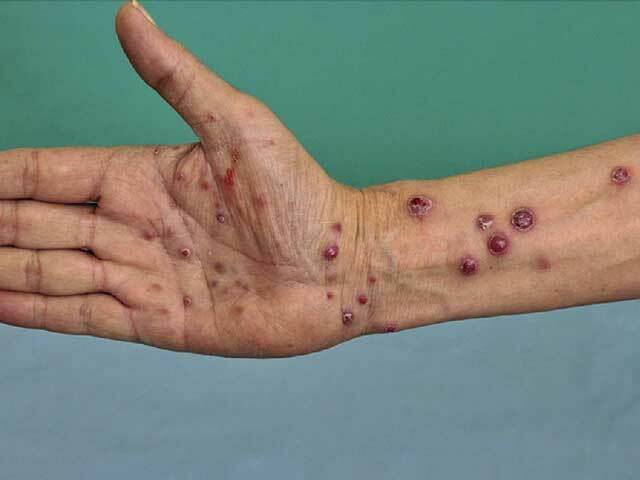
Bacillary angiomatosis in a transplant recipient
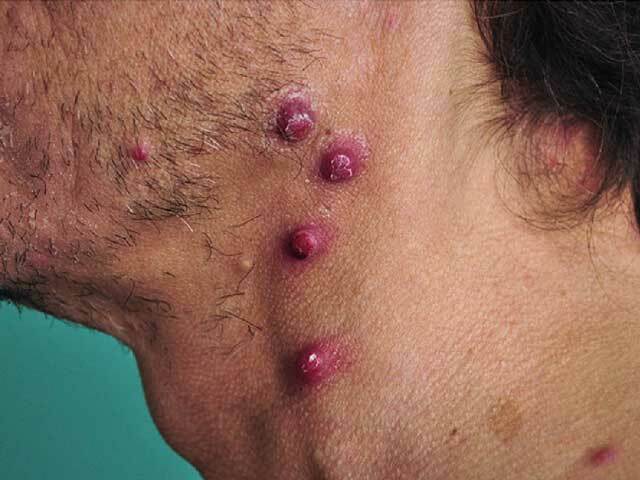
Bacillary angiomatosis in a transplant recipient
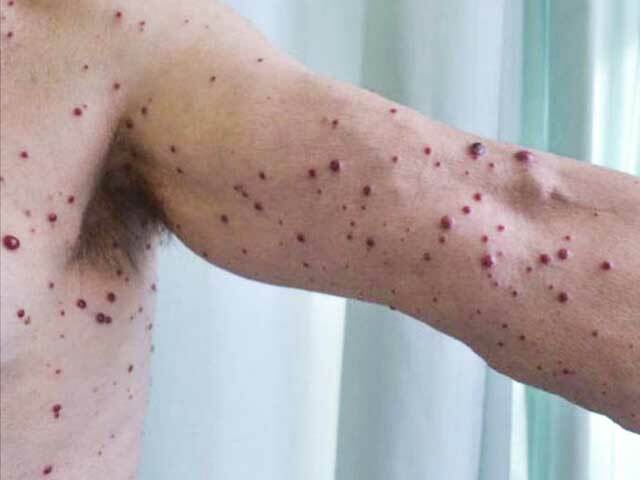
Bacillary angiomatosis in a transplant recipient
As the number of skin lesions increase, the patient may develop high fever, tender swollen lymph nodes, nausea, vomiting, sweats, chills, and poor appetite.
Hyperpigmented indurated plaques have been described mainly in skin of colour.
The infection can cause blood vessels to grow out of control and form tumour-like masses in other organs including the brain, bone, gastrointestinal tract, and respiratory tract with airway obstruction.
Liver involvement is called 'peliosis hepatis' or 'bacillary peliosis'.
Bacillary angiomatosis should be suspected clinically, particularly in an immunocompromised patient.
Skin biopsy shows lobular blood vessel proliferation with epithelioid endothelial cells, and an inflammatory infiltrate including neutrophils. The microorganisms can be seen as basophilic clumps in the stroma and confirmed on Giemsa or Warthin-Starry stain. [see Bacillary angiomatosis pathology]
Polymerase chain reaction (PCR) can be used to identify the causative agent.
Antibiotics should be continued for 3-6 months to prevent recurrence.
Large pus-filled lymph nodes or blisters may need to be drained. Supportive therapy includes hydration and analgesics for pain and fever. Warm moist compresses to affected nodes may decrease swelling and tenderness.
Cutaneous lesions of bacillary angiomatosis disappear with days to weeks of starting appropriate treatment, although response can be incomplete.
Spontaneous resolution has been reported.
Systemic bacillary angiomatosis can be fatal if not treated promptly.