Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Childhood melanoma — extra information
Childhood melanoma
Author: Natasha Gattey, MD Candidate, Class of 2016 College of Medicine, University of Saskatchewan, Canada.Chief Editor: Dr Amanda Oakley, Dermatologist, Hamilton, New Zealand, December 2014. DermNet Update July 2021
Introduction
Types
Clinical features
Differential diagnoses
Demographics
Treatment
Outlook
What is childhood melanoma?
Melanoma is a skin cancer that arises from melanocytes (pigment-producing cells). Childhood melanoma usually refers to melanoma diagnosed in individuals under the age of 18 years. It is rare.
For more information about melanoma, see:
What types of melanoma arise in childhood?
Melanoma arising in children has been classified into the following types:
- Melanoma present at birth (congenital melanoma)
- Melanoma developing in congenital melanocytic naevus (CMN) - a brown birthmark
- Melanoma arising in patients with dysplastic or atypical naevi (most often superficial spreading melanoma arising de novo)
- Malignant blue naevus
- Nodular melanoma (40–50% of melanoma in children)
- Spitzoid melanoma.
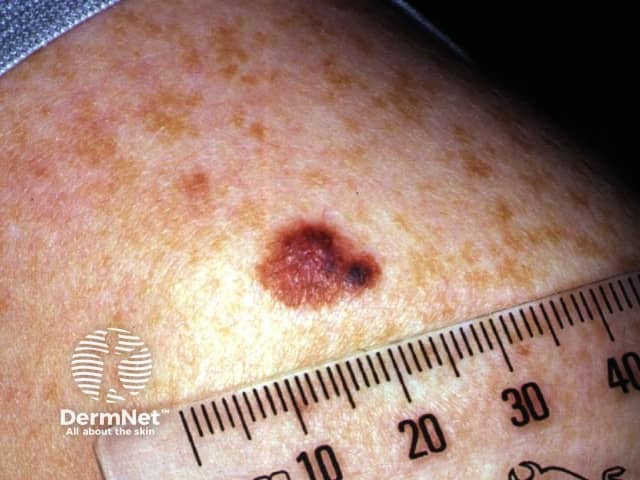
Superficial spreading melanoma in 14-year-old
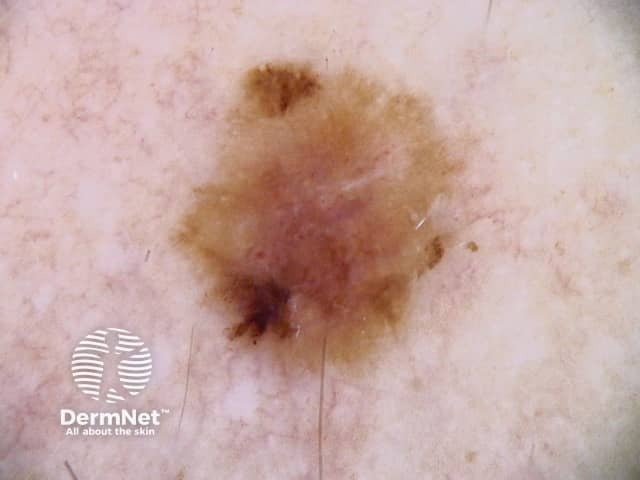
Dermoscopy of superficial spreading melanoma in 18-year-old
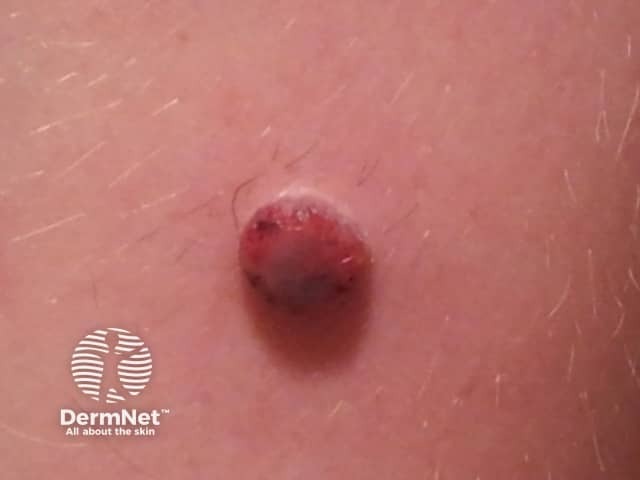
Spitzoid melanoma in 10-year-old
What are the clinical features of childhood melanoma?
Specific kinds of melanoma are described in detail elsewhere on DermNet: see melanoma resources. Some features notable in childhood melanoma are discussed here.
Melanoma in children aged 11 and older
Melanoma in older children appears similar to melanoma in adults; it presents as a growing lesion that looks different from the child's other lesions. Most are pigmented. About 60% have the ABCDE+EFG criteria.
Superficial early melanoma:
A: Asymmetry |
B: Border irregularity |
C: Colour variation |
D: Different |
E: Evolving |
Nodular melanoma:
E: Elevated |
F: Firm |
G: Growing |
Melanoma in children aged 10 or younger
Superficial spreading melanoma is less common in younger children and the melanoma has the ABCDE signs in 40% of cases.
Melanoma in young children is more commonly amelanotic (red coloured), nodular, and tends to be thicker at diagnosis than in older children and adults. Nodular melanoma has the EFG signs - Elevated, Firm, Growing.
Additional ABCD detection criteria for skin lesions in children have been suggested:
A: Amelanotic (the lesion is skin coloured or red) |
B: Bleeding, Bump |
C: Colour uniformity |
D: De novo, any Diameter |
Melanoma in a congenital melanocytic naevus
Small congenital naevi arise in 1 in 100 births. Melanoma is a rare complication of small to medium congenital naevi with a higher risk associated with large congenital naevi and overall risk for all CMN 1-2%. Melanoma is also associated with multiple congenital naevi even in the absence of a giant CMN. It tends to appear on the edge of the birthmark and is recognised by change within the melanocytic naevus (mole) and the ABCDE+EFG criteria described above.
Melanoma arises in up to 15% of children 10 years or younger with a giant congenital melanocytic naevus >40 cm in diameter (G3) particularly if associated with neurocutaneous melanocytosis. Such giant congenital melanocytic naevi are very rare, arising in 1 in 20,000 births. In giant congenital melanocytic naevi:
- Melanoma may arise within the centre of the melanoma
- It tends to arise within deeper dermal naevus cells rather than within superficial naevus cells
- The melanoma may also arise within the central nervous system due to neurocutaneous melanocytosis
- The risk of melanoma is greater in giant naevi that cross the midline of the spine and in children with satellite naevi
- Prophylactic removal of the naevi does not appear to reduce the risk of melanoma.
These melanomas can be difficult to detect early. Excision may also be difficult or impossible.
Differential diagnosis of childhood melanoma
Common moles are usually easy to recognise and are uniform in structure and colour. They remain fairly stable once they have reached their final size.
Red skin nodules that can be confused with melanoma in children include Spitz naevus and pyogenic granuloma. Both of these look different from the child's other skin spots and tend to progressively enlarge. Pyogenic granuloma is prone to bleed easily. Benign proliferative nodules can arise within congenital naevi.
Who gets childhood melanoma?
Cutaneous melanoma in children is rare, and extremely rare before puberty. It comprises 3% of all paediatric cancers. However, in New Zealand, melanoma is the second most common cancer registration in people aged 0–24 years.
Risk factors for childhood melanoma include:
- Giant congenital naevus
- Fitzpatrick skin phototypes I-II (ie, fair skin that burns easily and tans poorly, freckles)
- Immunodeficiency or immunosuppression
- History of retinoblastoma
- Familial atypical naevi (dysplastic naevus syndrome)
- Many moles
- Xeroderma pigmentosum (a very rare disorder with extreme sensitivity to sunlight).
Like the adult population, melanoma mainly affects Caucasian children and is associated with sun exposure. There is a slight female preponderance.
What is the treatment for childhood melanoma?
Treatment of childhood melanoma is the same as in adults. In New Zealand:
- Lesions that are suspicious for melanoma are completely removed by initial diagnostic excisional biopsy, usually with a 2-mm clinical margin.
- If melanoma is confirmed, a second surgical procedure is undertaken to remove a wider margin of normal skin. This is called wide local excision. The size of the margin depends on the Breslow thickness of the melanoma.
- If the melanoma has thickness >1 mm or other features of concern, sentinel node biopsy may be offered. However, its role in the paediatric population is not well established.
- Follow-up is arranged to look for recurrence and new lesions of concern.
Metastatic melanoma or advanced melanoma is melanoma that has spread to lymph nodes or elsewhere in the body. Treatment is individualised but may include surgery, radiotherapy, chemotherapy, or targeted therapy.
What is the outlook for patients with childhood melanoma?
Prognosis of melanoma depends on the stage of melanoma, ie, whether it has spread beyond its original site in the skin. Spread of melanoma to lymph nodes and elsewhere is more likely in thicker tumours (measured by Breslow thickness at the time of removal of a primary tumour).
Survival rates are similar in older children and adults. However, melanomas in children under 11 years of age appear to have a less aggressive behaviour than those detected in adults.
Bibliography
- Cordoro KM, Gupta D, Frieden IJ, McCalmont T, Kashani-Sabet M. Pediatric melanoma: results of a large cohort study and proposal for modified ABCD detection criteria for children. J Am Acad Dermatol. 2013;68(6):913-25. doi: 10.1016/j.jaad.2012.12.953. Epub 2013 Feb 8. PubMed
- Han D, Zager JS, Han G, Marzban SS, Puleo CA, Sarnaik AA, Reed D, Messina JL, Sondak VK. The unique clinical characteristics of melanoma diagnosed in children. Ann Surg Oncol. 2012;19(12):3888-95. doi: 10.1245/s10434-012-2554-5. PubMed
- Kinsler VA, O'Hare P, Bulstrode N, et al. Melanoma in congenital melanocytic naevi. Br J Dermatol. 2017;176(5):1131-43. doi:10.1111/bjd.15301 PubMed Central
- Krengel S, Hauschild A, Schäfer T. Melanoma risk in congenital melanocytic naevi: a systematic review. Br J Dermatol. 2006;155(1):1-8. doi:10.1111/j.1365-2133.2006.07218.x PubMed
- Mehregan AH, Mehregan DA. Malignant melanoma in childhood. Cancer. 1993;71(12):4096-103. doi:10.1002/1097-0142(19930615)71:12<4096::aid-cncr2820711248>3.0.co;2-z PubMed
- Paradela S, Fonseca E, Pita-Fernández S, Kantrow SM, Diwan AH, Herzog C, Prieto VG. Prognostic factors for melanoma in children and adolescents: a clinicopathologic, single-center study of 137 patients. Cancer. 2010;116(18):4334-44. doi: 10.1002/cncr.25222. PubMed
- Paradela S, Fonseca E, Prieto VG. Melanoma in children. Arch Pathol Lab Med. 2011;135(3):307-16. doi: 10.1043/2009-0503-RA.1. PubMed
- Rao BN, Hayes FA, Pratt CB, et al. Malignant melanoma in children: its management and prognosis. J Pediatr Surg. 1990;25(2):198-203. doi:10.1016/0022-3468(90)90402-u PubMed
- Ministry of Health. 2014. Cancer: New registrations and deaths 2011. Wellington: Ministry of Health. September 2014.
- Vourc'h-Jourdain M, Martin L, Barbarot S; aRED. Large congenital melanocytic nevi: therapeutic management and melanoma risk: a systematic review. J Am Acad Dermatol. 2013;68(3):493-8.e1-14. doi: 10.1016/j.jaad.2012.09.039. PubMed
On DermNet
- Melanoma — for patients
- Melanoma — for health professionals
- Melanoma in skin of colour
Other websites
- Rare childhood cancers: Melanoma National Cancer Institute
- Melanoma risk assessment tool — Melanoma Institute of Australia
- Melanoma education — Melanoma Institute of Australia
