Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Complications of atopic dermatitis — extra information
Complications of atopic dermatitis
Authors: Dr Amy Stanway, Department of Dermatology, Waikato (Feb 2004); Updated: Dr Aysha Rashid, Medical Registrar, Auckland; Associate Professor Paul Jarrett, Dermatologist, Middlemore Hospital and Department of Medicine, The University of Auckland, New Zealand (Aug 2021)
Infective complications of atopic dermatitis
Contact dermatitis and atopic dermatitis
Complications in skin colour
Other complications
Infective complications of atopic dermatitis
Skin infection is very common in atopic dermatitis due to an inherently abnormal skin barrier, cutaneous and systemic immune system abnormalities, and scratching the itch. Cutaneous colonisation by Staphylococcus aureus forms a bacterial biofilm and worsens the dermatitis by promoting the Th2 allergic inflammatory response. Infants are particularly at risk of severe skin infections.
Bacterial skin infections in atopic dermatitis
-
- Staph aureus causes impetiginisation of atopic dermatitis
-
- Strep pyogenes may cause impetigo, pustules, or punched out erosions with a scalloped border
Bacterial infection and atopic dermatitis
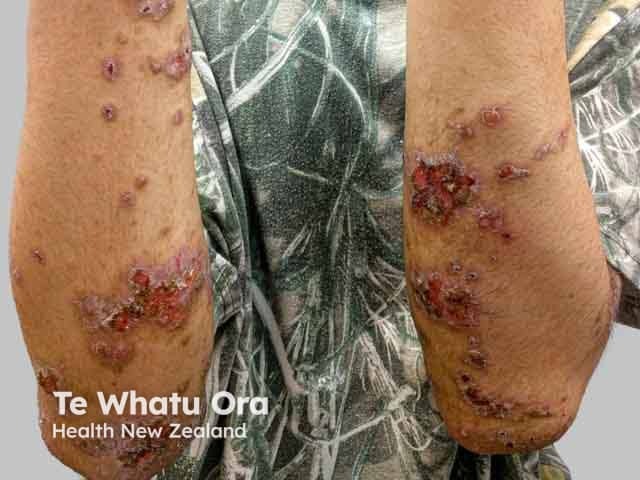
Impetiginised atopic eczema in teenager with skin of colour
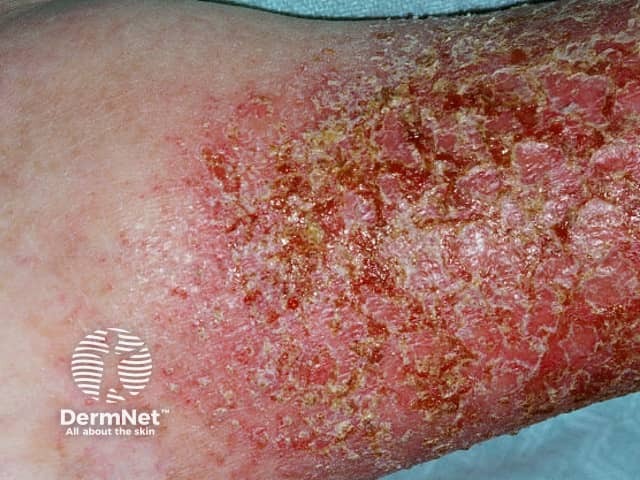
Infection eczema
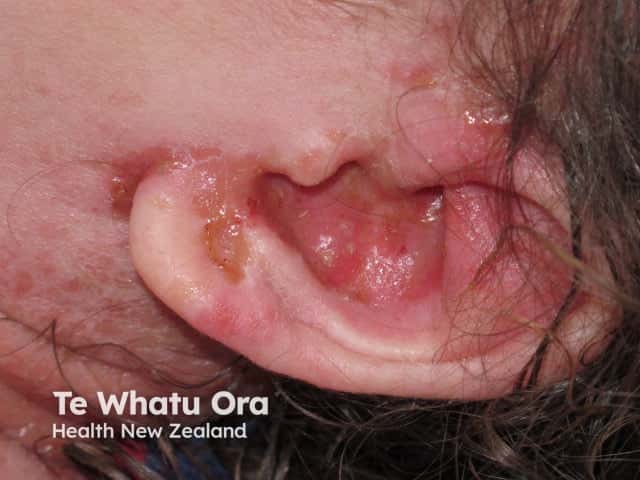
Infected eczema
Viral skin infections in atopic dermatitis
- Molluscum contagiosum
- Eczema herpeticum
- Eczema coxsackium
- Eczema vaccinatum
- Rare complication of smallpox vaccination
- Vesicular, pustular, or nodular rash after contact with vaccinia virus
Molluscum contagiosum infection and atopic dermatitis
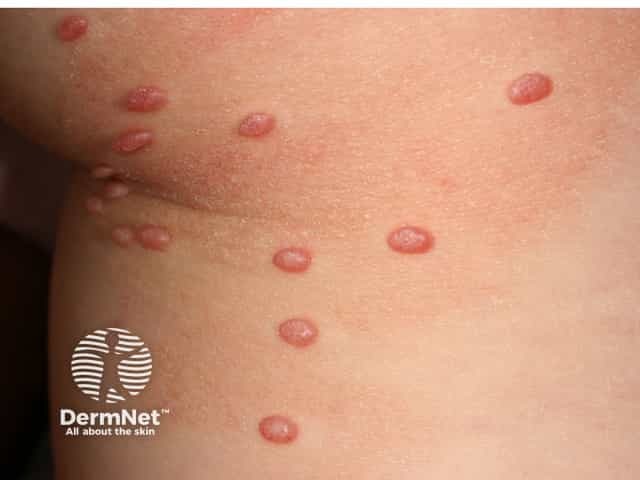
Molluscum contagiosum
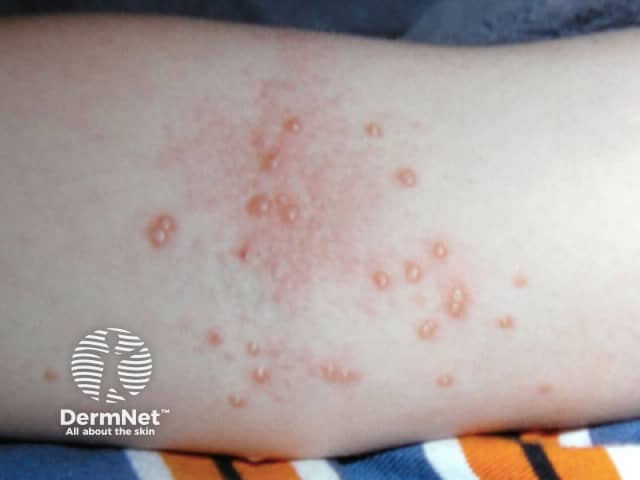
Molluscum contagiosum
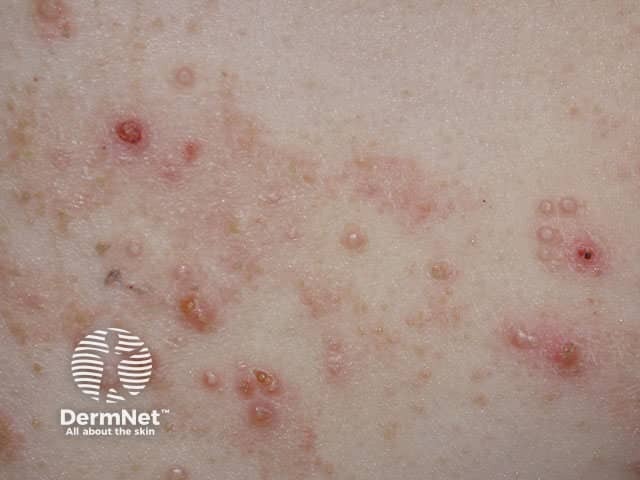
Molluscum contagiosum
Eczema herpeticum
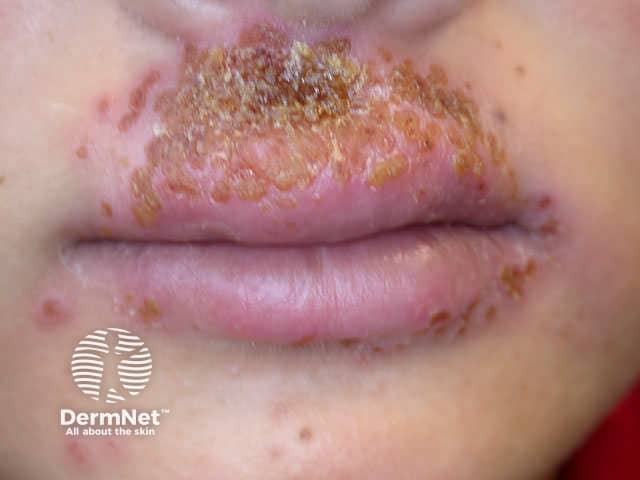
Eczema herpeticum
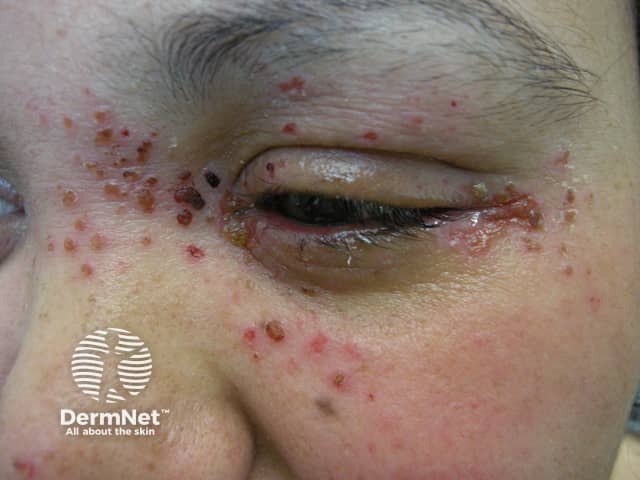
Eczema herpeticum
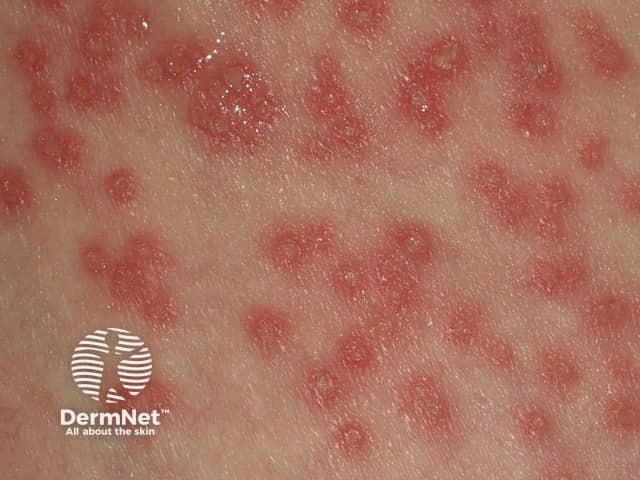
Eczema herpeticum
Fungal skin infections in atopic dermatitis
- Dermatophyte
- Trichophyton rubrum and Epidermophyton skin infection of the head and neck [see Tinea capitis, Tinea faciei]
- Yeast
- Malassezia furfur [see Skin conditions associated with Malassezia]
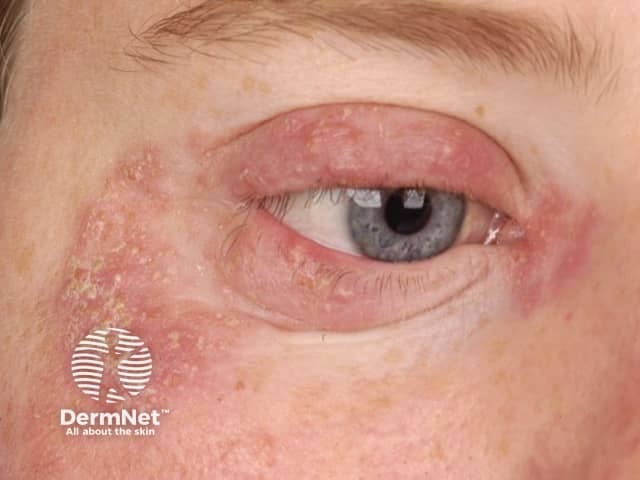
Tinea faciei
Complications of skin infections in atopic dermatitis
- Cutaneous abscess
- Septicaema/septic shock
- Osteomyelitis
- Septic arthritis/bursitis
- Bacterial endocarditis
- Herpes virus encephalitis
Contact dermatitis and atopic dermatitis
Contact dermatitis should be considered in the atopic patient with an otherwise unexplained dermatitis flare, particularly if in a patterned distribution.
Irritant contact dermatitis and atopic dermatitis
Irritant contact dermatitis is particularly common with atopic dermatitis due to the abnormal skin barrier function. Atopic hand dermatitis and occupational skin disease are frequent manifestations.
Allergic contact dermatitis and atopic dermatitis
The frequent use of multiple topical treatments for atopic dermatitis increases the risk of allergic contact dermatitis due to exposure to potential allergens. Aeroallergens also commonly aggravate other manifestations of atopy such as hay fever and asthma.
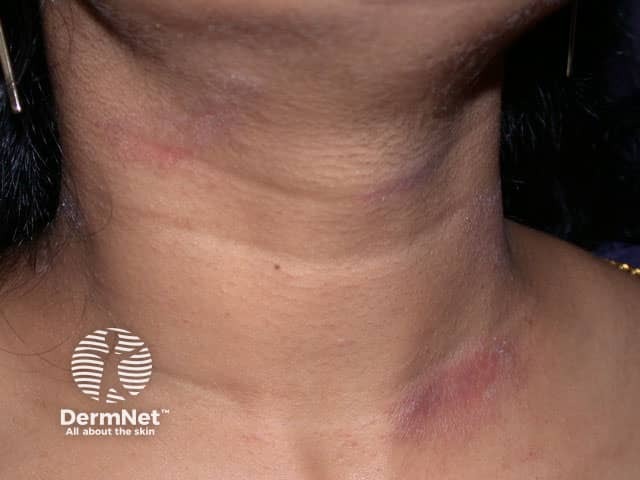
Contact dermatitis to ethylenediamine
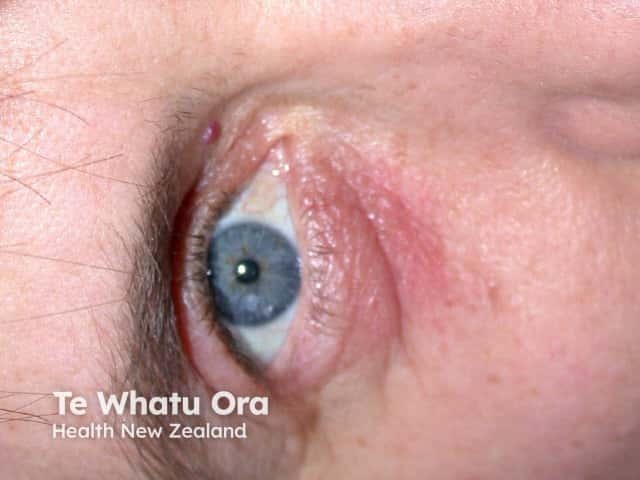
Airborne contact dermatitis eyelid
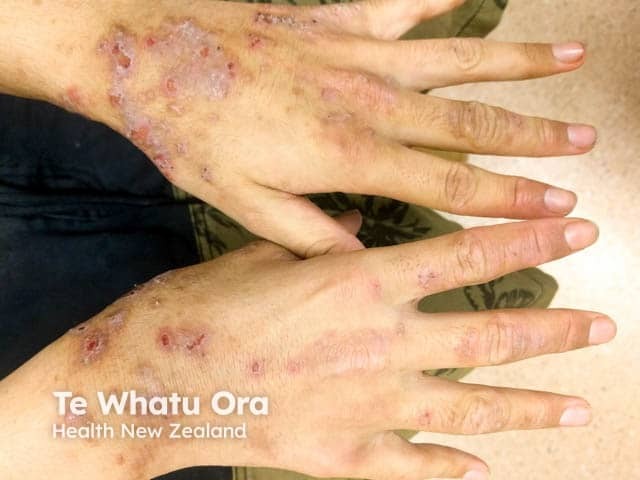
Atopic hand dermatitis
Complications of atopic dermatitis in skin of colour
- Postinflammatory hyperpigmentation
- Postinflammatory hypopigmentation and leukoderma
- Vitamin D deficiency due to covering involved skin especially if extensive
Dyspigmentation due to atopic dermatitis in skin of colour
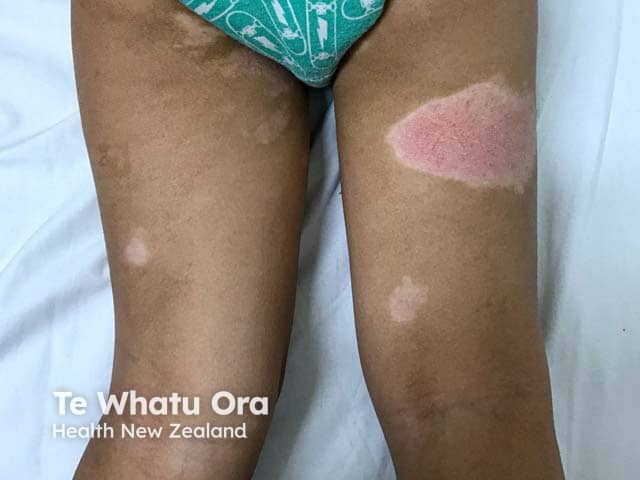
Atopic dermatitis with dyspigmentation in young child with skin of colour
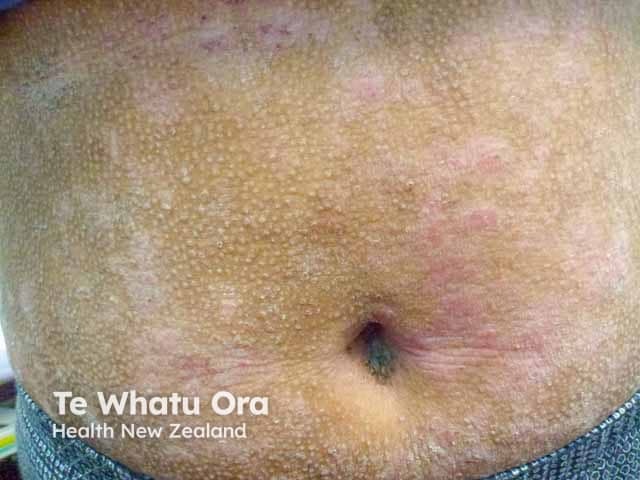
Papular atopic dermatitis with post-inflammatory hypopigmentation in teenager with skin of colour
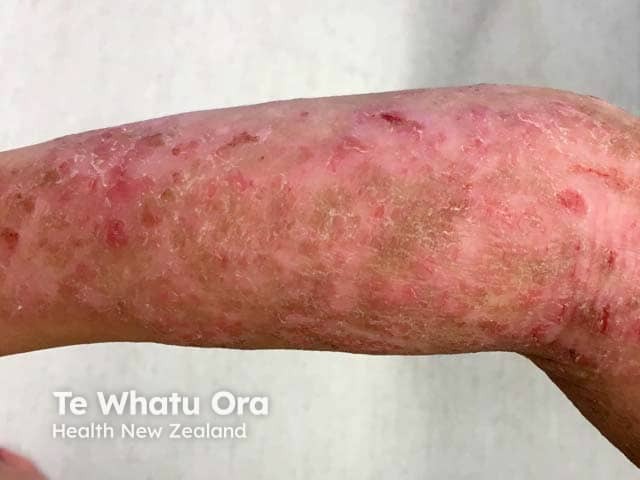
Atopic dermatitis with dyspigmentation in child with skin of colour
Other complications of atopic dermatitis
- Erythroderma and its complications in atopic dermatitis
- Psychological effects of atopic dermatitis
- Ophthalmological complications of atopic dermatitis
- Vernal keratoconjunctivitis in children
- Blepharitis, infectious keratitis, keratoconus
- Atopic keratoconjunctivitis in adults
- Corneal scarring, loss of vision
- Herpes keratoconjunctivitis in eczema herpeticum
- Cataracts
- Bilateral with characteristic appearance on eye examination
- Associated with severe atopic dermatitis
- Onset around age 15–25 years
- Vernal keratoconjunctivitis in children
- Growth
- Severe dermatitis may slow the growth rate of children
- Growth retardation can be due to the dermatitis itself and/or treatment such as systemic corticosteroids
- Dietary restrictions may affect growth and, in extreme cases, cause protein-energy malnutrition
Other complications of atopic dermatitis
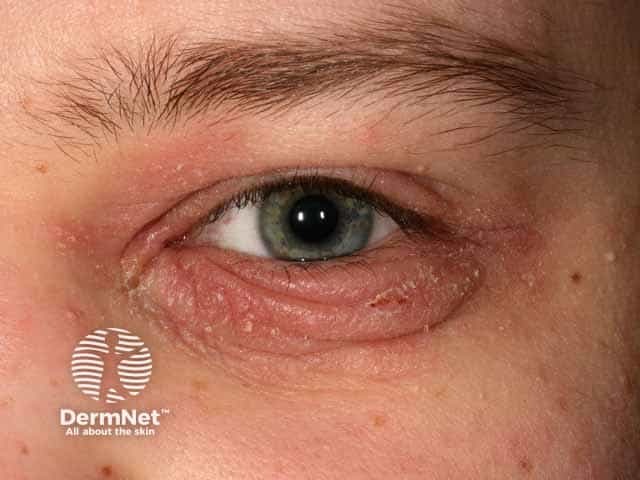
Blepharitis associated with atopic dermatitis
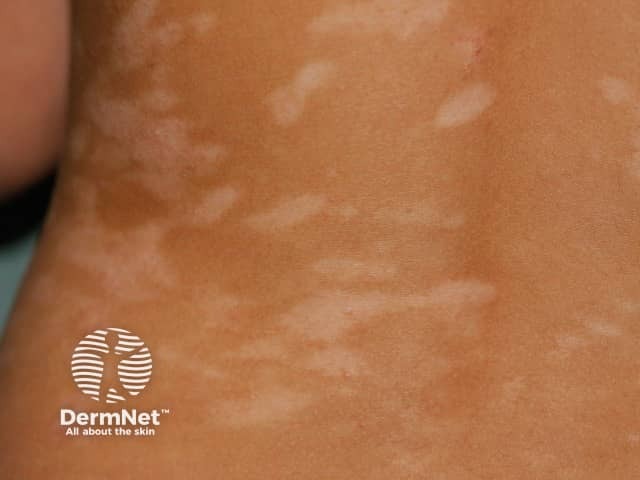
Postinflammatory hypopigmentation
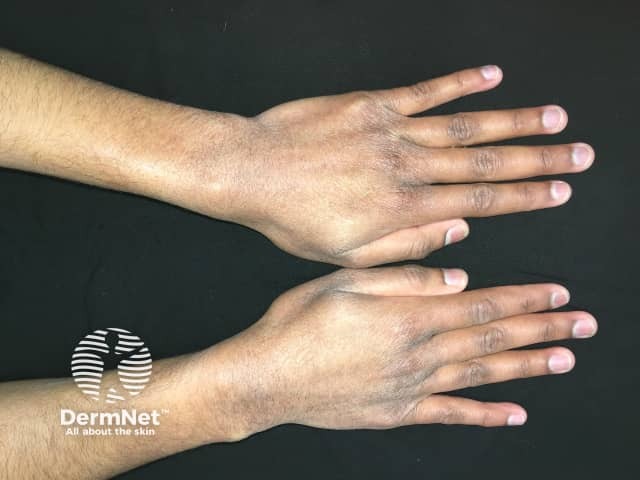
Atopic hand dermatitis
Bibliography
- Boonstra M, Rustemeyer T, Middelkamp-Hup MA. Both children and adult patients with difficult-to-treat atopic dermatitis have high prevalences of concomitant allergic contact dermatitis and are frequently polysensitized. J Eur Acad Dermatol Venereol. 2018;32(9):1554–61. doi:10.1111/jdv.14973. Journal
- Drucker AM. Atopic dermatitis: burden of illness, quality of life, and associated complications. Allergy Asthma Proc. 2017;38(1):3–8. doi:10.2500/aap.2017.38.4005. PubMed
- Hsu JI, Pflugfelder SC, Kim SJ. Ocular complications of atopic dermatitis. Cutis. 2019;104(3):189–93. Journal
- Jacob SE, McGowan M, Silverberg NB, et al. Pediatric Contact Dermatitis Registry data on contact allergy in children with atopic dermatitis. JAMA Dermatol. 2017;153(8):765–70. doi:10.1001/jamadermatol.2016.6136. PubMed Central
- Jeter J, Bowen C. Atopic dermatitis and implications for military service. Mil Med. 2019;184(5-6):e177–82. doi:10.1093/milmed/usy427. Journal
- Kim KH. Clinical pearls from atopic dermatitis and its infectious complications. Br J Dermatol. 2014;170 Suppl 1:25–30. doi:10.1111/bjd.12919. Journal
- Owen JL, Vakharia PP, Silverberg JI. The role and diagnosis of allergic contact dermatitis in patients with atopic dermatitis. Am J Clin Dermatol. 2018;19(3):293–302. doi:10.1007/s40257-017-0340-7. PubMed Central
- Silverberg JI. Comorbidities and the impact of atopic dermatitis. Ann Allergy Asthma Immunol. 2019;123(2):144–51. doi:10.1016/j.anai.2019.04.020. Journal
- Tamagawa-Mineoka R, Katoh N. Atopic dermatitis: identification and management of complicating factors. Int J Mol Sci. 2020;21(8):2671. doi:10.3390/ijms21082671. Journal
- Torres T, Ferreira EO, Gonçalo M, Mendes-Bastos P, Selores M, Filipe P. Update on atopic dermatitis. Acta Med Port. 2019;32(9):606–13. doi:10.20344/amp.11963. Journal
- Wang V, Boguniewicz J, Boguniewicz M, Ong PY. The infectious complications of atopic dermatitis. Ann Allergy Asthma Immunol. 2021;126(1):3–12. doi:10.1016/j.anai.2020.08.002. Journal
On DermNet
- Atopy
- Allergy to topical medication
- Atopic dermatitis
- Atopic hand dermatitis
- Barrier function in atopic dermatitis
- Causes of atopic dermatitis
- Psychological effects of atopic dermatitis
- Treatment of atopic dermatitis
Other websites
- AltogetherEczema: The Global Network for Eczema & Atopic Dermatitis
- Atopic dermatitis — Medscape
- Complications: atopic eczema — National Health Service UK
