Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Last Reviewed: January, 2025
Authors: Dr Amy Stanway, Dermatologist, NZ (2004); Hon A/Prof Amanda Oakley, Dermatologist, New Zealand (2016); Hon A/Prof Paul Jarrett, Dermatologist, Middlemore Hospital and UoA, New Zealand (2021); Dr Libby Whittaker, Medical Writer, NZ (2022)
Last reviewed by: Dr Ian Coulson, Dermatologist (2025)
Edited by the DermNet content department
Introduction
General measures
Topical treatments
OTC topical treatments
Prescription topical treatments
Systemic treatments
New and emerging treatments
Skin of colour
Treatment of infective complications
Atopic dermatitis (atopic eczema), the most common inflammatory skin disease worldwide, involves genetic and environmental factors. It is not yet possible to modify genetic factors and it can be difficult to effectively manipulate all relevant environmental factors. There is therefore no known cure for atopic dermatitis, however, treatment can control inflammatory dermatitis and help the skin feel healthy:
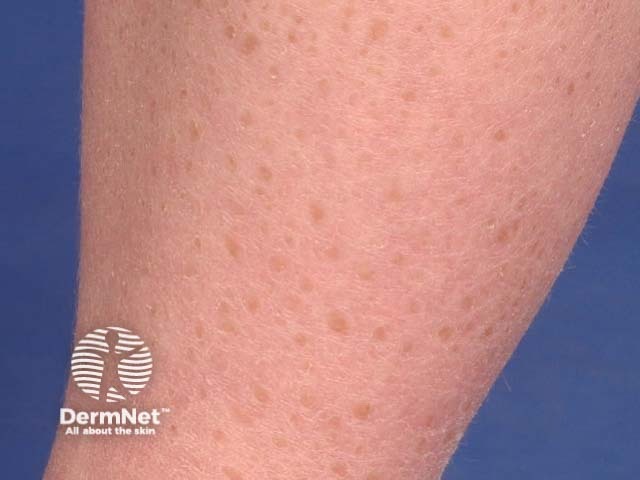
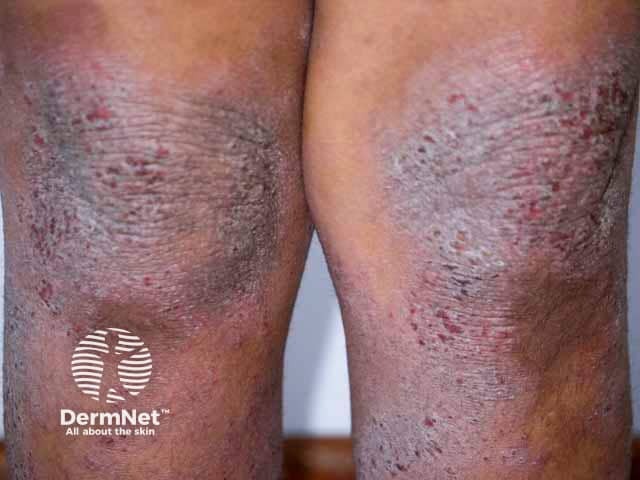
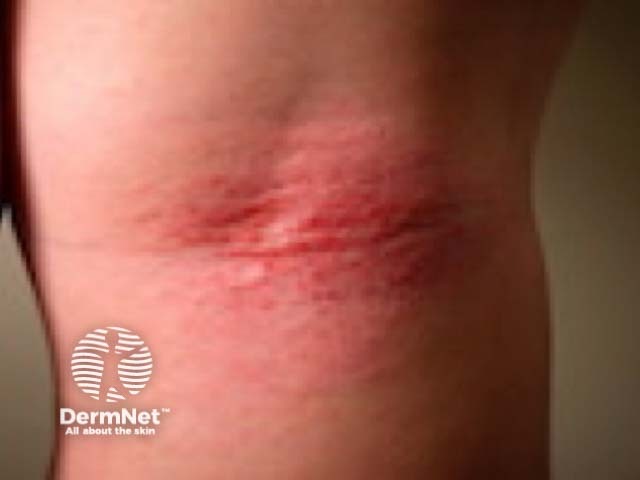
Topical treatments can come in many forms. It is important that the correct formulation is used for the different patterns and distributions of atopic dermatitis.

A selection of emollients from the light to the very greasy
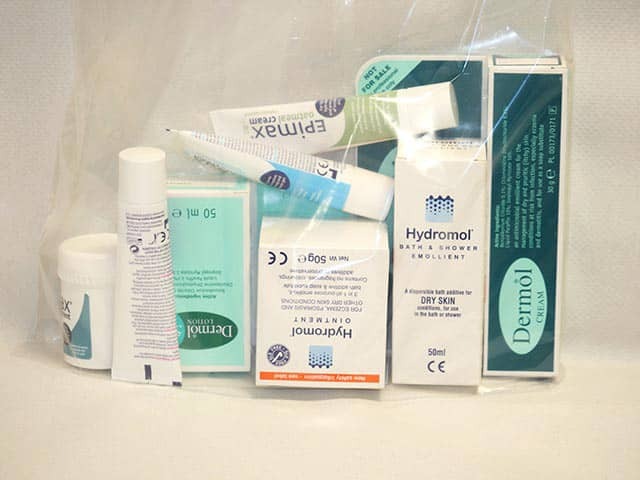
An emollient self selection bag which allows a home trial of a range of emollients, then ordering large amounts of the favoured product

A selection of topical steroids

UVB treatment
See also: Complications of atopic dermatitis.