Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Treatments Lesions (cancerous)
Author: Dr Matthew Howard, Clinic/Research Fellow, Victorian Melanoma Service, Melbourne, VIC, Australia. DermNet Editor in Chief: Adjunct A/Prof. Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy edited by Gus Mitchell. January 2020.
Introduction Demographics Contraindications More information Benefits Risks and disadvantages
There are two types of lymph node surgery for cutaneous melanoma:
A sentinel lymph node biopsy is used to identify and sample the ‘sentinel’ or first lymph node (or nodes) that potential metastatic melanoma would encounter if present in lymphatic vessels draining the site of the primary melanoma.
Sentinel lymph node biopsy is performed in people who do not have swollen lymph nodes at the time of re-excision of the biopsy site — known as wide local excision — and is usually under general anaesthetic [3].
A blue dye is injected into the initial biopsy scar prior to the wide local excision. This dye is carried by lymphatic channels to the sentinel lymph node or nodes [3].
Lymphoscintigraphy is also used to map the sentinel lymph nodes, using a specialised scanner to detect radiation from a radiotracer combined with the blue dye [7,8].
The sentinel lymph nodes are excised for examination by a pathologist who measures the dimensions of any melanoma found within the lymph nodes and whether it extends beyond the lymph node (which confers poorer prognosis) [9].
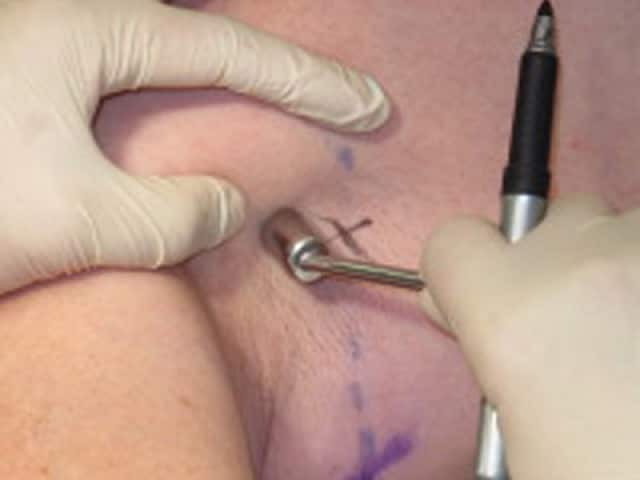
Looking for sentinel node
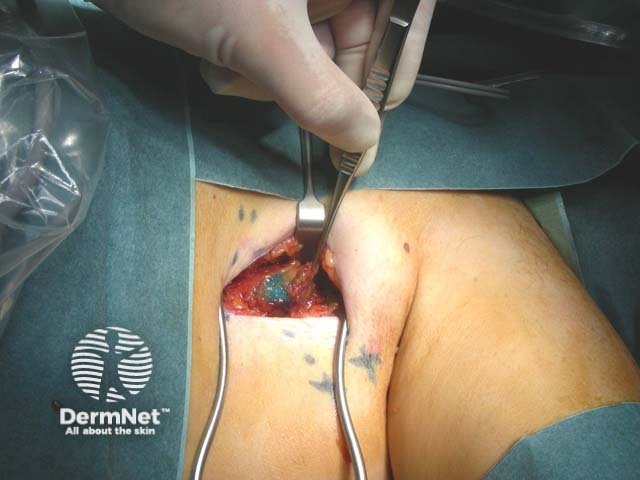
Dye seen in lymph node during sentinel node biopsy
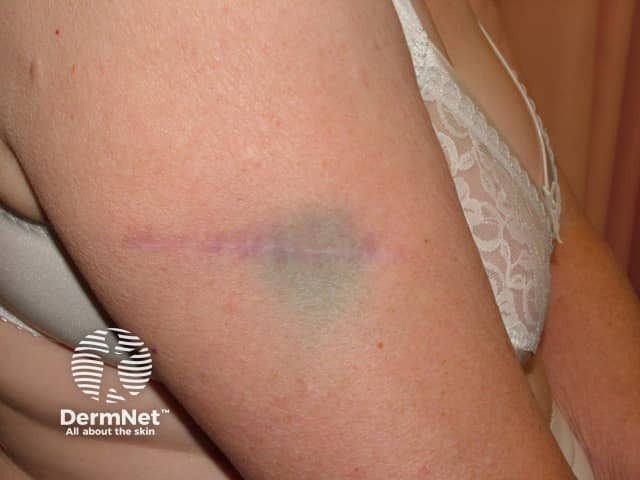
Sentinel node biopsy persistent tattoo
Lymph node dissection or completion lymphadenectomy is the removal of all lymph nodes in the nodal basin (eg, axilla, inguinal region, or head and neck) [2]. This is performed under general anaesthetic. The pathologist examines all the excised lymph nodes for metastatic melanoma [2].
Whether sentinel lymph node biopsy is performed depends on a melanoma patient’s risk for nodal metastasis. Opinions vary in which patients it should be performed; the key influence was the publication of the ‘MSLT-1’ study [10]. SLNB is currently considered for:
Lymph node dissection is currently considered in two settings:

Nodal metastatic melanoma
Contraindications mainly relate to sentinel node biopsy.
A positive sentinel lymph node biopsy gives prognostic information for risk stratification and staging; it does not have therapeutic benefit. Compared to those who underwent regular observation, those who underwent sentinel lymph node biopsy had no difference in 10-year melanoma-specific survival [10].
Prior to the publication of the results of two studies, ‘DeCOG-SLT’ and ‘MSLT-II’, completion lymph node dissection was recommended for patients with a positive sentinel lymph node biopsy [2,12].
Sentinel lymph node biopsy provides prognostic information.
Completion dissection offers immediate control of nodal metastatic melanoma.
Complication rates for sentinel lymph node biopsy occur in 6–14% of patients [19,20]. The risks of any lymph node surgery include:
Risks specific to sentinel node biopsy include:
The risks of complications from completion dissection are more common and serious than for sentinel lymph node biopsy, especially lymphoedema, secondary bacterial skin infection, delayed healing, nerve damage, and tight scar formation [22,23].
Lymphoedema is the swelling of the limb distal to the dissected nodal basin due to disruption of lymphatic fluid return. This can be very disabling for patients with only modest improvement achieved from wearing compression garments and massage/exercise [24]. The risk of developing lymphoedema is greater with inguinal completion dissection than with axillary dissection.
Completion dissection may not prevent the development of metastases elsewhere.