Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Authors: Matthew James Verheyden, Royal North Shore Hospital, Sydney, Australia; Dr Monisha Gupta, Senior Staff Specialist, The Skin Hospital, Australia. Technical Editor: Mary Elaine Luther, Ross University School of Medicine, Barbados. DermNet Editor in Chief: Adjunct A/Prof Amanda Oakley, Dermatologist, New Zealand. Copy edited by Gus Mitchell. February 2020.
Introduction Demographics Causes Clinical features Diagnosis Differential diagnoses Treatment Outcome
Macular amyloidosis is one of three forms of primary localised cutaneous amyloidosis. A proteinaceous material — amyloid — is deposited harmlessly in the skin, causing hyperpigmented patches.
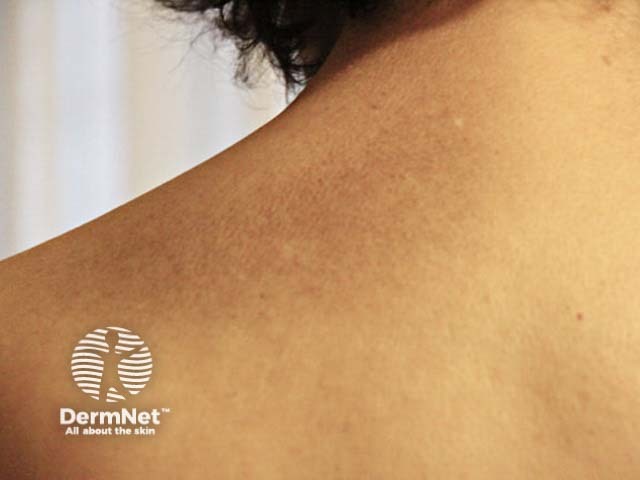
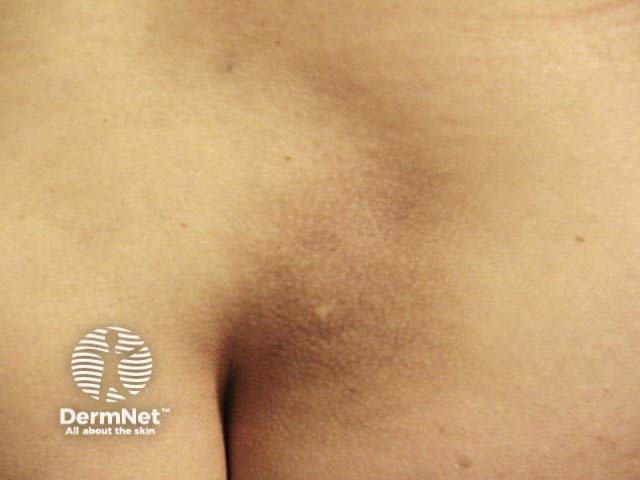
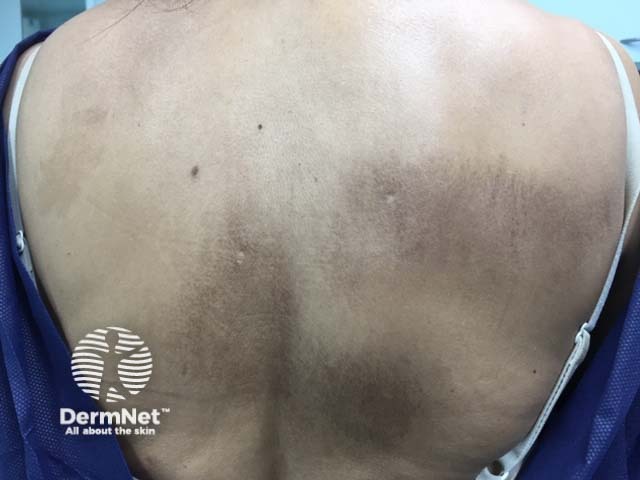
Macular amyloidosis
Most cases of macular amyloidosis arise in early adulthood. There is a higher incidence of macular amyloidosis in people of Asian, Middle Eastern, and South American descent than in people of European and North American descent [1]. Populations with darker skin (Fitzpatrick skin phototype IV and V) are more commonly affected.
Up to 10% of cases of macular amyloidosis are familial in origin.
Women present with macular amyloidosis more often than men; this may be due to women seeking medical attention earlier than men due to cosmetic concerns.
Associations with multiple endocrine neoplasia type 2A (MEN2A) and atopic dermatitis have been reported [4,5].
The precise cause of macular amyloidosis is uncertain, although there appears to be an interplay between genetic and environmental factors that is triggered by prolonged periods of friction, rubbing, or scratching of the affected region.
Two theories have been proposed to explain the aberrant deposition of amyloid: the fibrillar body theory [6,7] and the secretory theory [8].
Macular amyloidosis presents with small dusky-brown or blue-grey hyperpigmented macules.
Dermatoscopy reveals a central white or brown area surrounded by brown pigmentation as fine radiating streaks, dots, leaf-like projections, and bulbous projections [10].
The diagnosis of macular amyloidosis is based on the characteristic clinical presentation and histopathological findings of cutaneous amyloid deposits within a skin biopsy. See Primary cutaneous amyloidosis pathology.
Macular amyloidosis can be confused with other pigmentary disorders, including:
The primary goal of treatment is the relief of pruritus.
Emphasis should be placed on the importance of avoiding mechanical stressors such as friction, rubbing, or scratching the affected regions.
No standardised treatment regimen has been established [11]. In most cases, topical corticosteroids and emollients are used to reduce the itch.
Other local medications may include:
Systemic medications are rarely required; however, macular amyloidosis has been reported to have been successfully treated with the following drugs:
Physical therapies reported to be of benefit include:
Macular amyloidosis is persistent and may have a significant impact on the quality of life, due to cosmetic disfigurement and persistent pruritus. [17].