Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Macular amyloidosis — extra information
Macular amyloidosis
Authors: Matthew James Verheyden, Royal North Shore Hospital, Sydney, Australia; Dr Monisha Gupta, Senior Staff Specialist, The Skin Hospital, Australia. Technical Editor: Mary Elaine Luther, Ross University School of Medicine, Barbados. DermNet Editor in Chief: Adjunct A/Prof Amanda Oakley, Dermatologist, New Zealand. Copy edited by Gus Mitchell. February 2020.
Introduction Demographics Causes Clinical features Diagnosis Differential diagnoses Treatment Outcome
What is macular amyloidosis?
Macular amyloidosis is one of three forms of primary localised cutaneous amyloidosis. A proteinaceous material — amyloid — is deposited harmlessly in the skin, causing hyperpigmented patches.
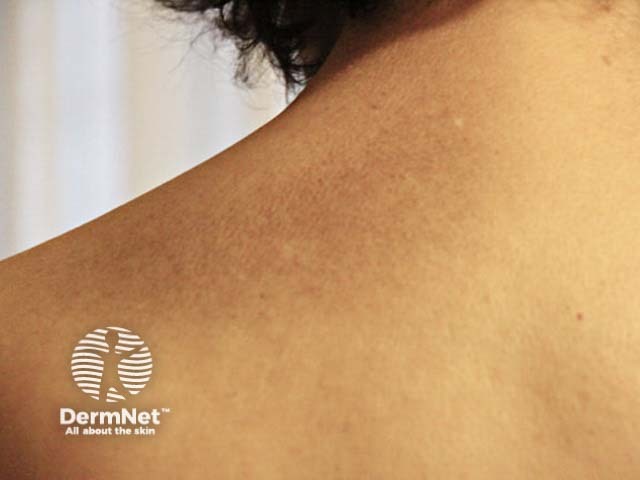
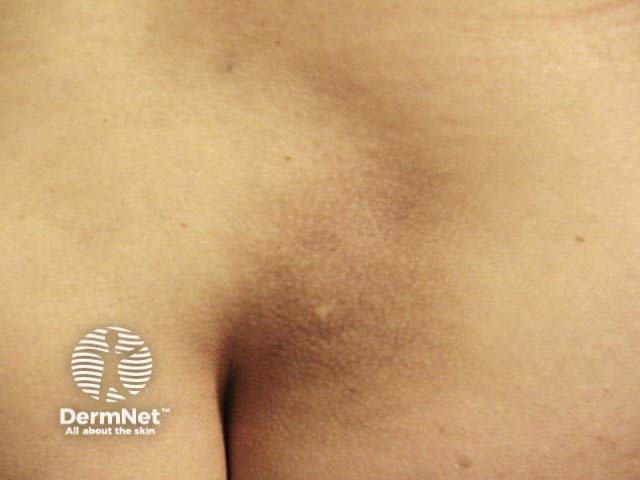
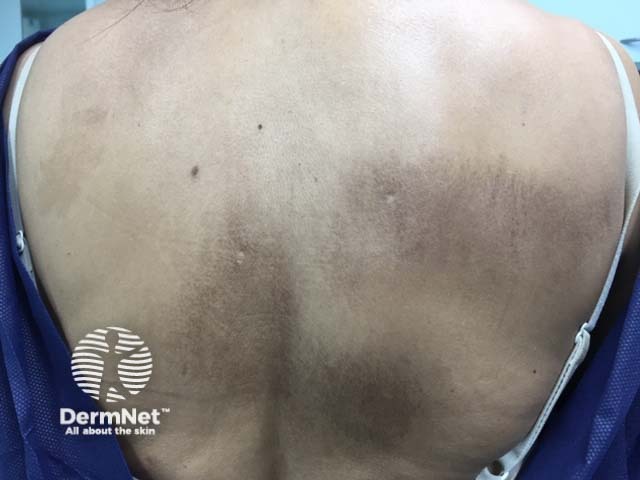
Macular amyloidosis
Who gets macular amyloidosis?
Most cases of macular amyloidosis arise in early adulthood. There is a higher incidence of macular amyloidosis in people of Asian, Middle Eastern, and South American descent than in people of European and North American descent [1]. Populations with darker skin (Fitzpatrick skin phototype IV and V) are more commonly affected.
Up to 10% of cases of macular amyloidosis are familial in origin.
- An autosomal dominant inherited form of primary localised cutaneous amyloidosis has been identified in Brazilian and Chinese families due to a mutation in the OSMR gene [2,3].
- An autosomal dominant primary localised cutaneous amyloidosis in Taiwanese families is related to a mutation in the IL-31RA gene which encodes the protein, interleukin-31 receptor A [2].
Women present with macular amyloidosis more often than men; this may be due to women seeking medical attention earlier than men due to cosmetic concerns.
Associations with multiple endocrine neoplasia type 2A (MEN2A) and atopic dermatitis have been reported [4,5].
What causes macular amyloidosis?
The precise cause of macular amyloidosis is uncertain, although there appears to be an interplay between genetic and environmental factors that is triggered by prolonged periods of friction, rubbing, or scratching of the affected region.
Two theories have been proposed to explain the aberrant deposition of amyloid: the fibrillar body theory [6,7] and the secretory theory [8].
What are the clinical features of macular amyloidosis?
Macular amyloidosis presents with small dusky-brown or blue-grey hyperpigmented macules.
- The macules are distributed symmetrically over the upper back (especially the interscapular area) and the extensor surfaces of the upper arms.
- Uncommonly, the face, neck, collarbones, breasts, and armpits are involved.
- Macular amyloidosis is generally pruritic, although the degree of pruritus varies from mild to severe.
- It can assume a subtle rippled or reticulated pattern, which resembles the ‘seafloor pattern’ seen in lichen amyloidosis.
- Macular amyloidosis may co-exist with lichen amyloidosis in up to 25% of affected patients [9].
Dermatoscopy reveals a central white or brown area surrounded by brown pigmentation as fine radiating streaks, dots, leaf-like projections, and bulbous projections [10].
How is macular amyloidosis diagnosed?
The diagnosis of macular amyloidosis is based on the characteristic clinical presentation and histopathological findings of cutaneous amyloid deposits within a skin biopsy. See Primary cutaneous amyloidosis pathology.
- Amorphous eosinophilic material is deposited extracellularly in the papillary dermis and is accompanied by dermal melanophages.
- Congo red staining can reveal positive apple-green birefringence under polarised light, which is characteristic of amyloid [9]. This birefringence is not observed in all cases [9].
- The distinction between lichen amyloidosis and macular amyloidosis is related to the amount, appearance, and location of the deposition.
- Histopathology might also demonstrate mild hyperkeratosis, hypergranulosis, and subepidermal clefting. Civatte bodies might be observed in the basal layer of the epidermis.
What is the differential diagnosis for macular amyloidosis?
Macular amyloidosis can be confused with other pigmentary disorders, including:
- Atrophic lichen planus
- Drug-induced hyperpigmentation
- Erythema dyschromicum perstans
- Notalgia paraesthetica
- Photocontact dermatitis
- Poikiloderma of Civatte
- Postinflammatory hyperpigmentation
- Pityriasis versicolor.
What is the treatment for macular amyloidosis?
The primary goal of treatment is the relief of pruritus.
Emphasis should be placed on the importance of avoiding mechanical stressors such as friction, rubbing, or scratching the affected regions.
No standardised treatment regimen has been established [11]. In most cases, topical corticosteroids and emollients are used to reduce the itch.
Other local medications may include:
Systemic medications are rarely required; however, macular amyloidosis has been reported to have been successfully treated with the following drugs:
Physical therapies reported to be of benefit include:
- Dermabrasion
- Occlusive dressings
- Transcutaneous electrical nerve stimulation (TENS) [12]
- PUVA (photochemotherapy)
- UVB phototherapy [13]
- Fractional laser treatment [14]
- Nd:YAG laser (532 nm and 1064 nm) [15]
- Pulsed dye laser treatment [16].
What is the outcome for macular amyloidosis?
Macular amyloidosis is persistent and may have a significant impact on the quality of life, due to cosmetic disfigurement and persistent pruritus. [17].
References
- Bandhlish A, Aggarwal A, Koranne RV. A clinico-epidemiological study of macular amyloidosis from north India. Indian J Dermatol. 2012;57(4):269-74. doi:10.4103/0019-5154.97662. PubMed Central
- Lin MW, Lee DD, Liu TT, et al. Novel IL31RA gene mutation and ancestral OSMR mutant allele in familial primary cutaneous amyloidosis. Eur J Hum Genet. 2010;18(1):26-32. doi:10.1038/ejhg.2009.135. PubMed Central
- Tanaka A, Arita K, Lai-Cheong JE, Palisson F, Hide M, McGrath JA. New insight into mechanisms of pruritus from molecular studies on familial primary localized cutaneous amyloidosis. Br J Dermatol. 2009;161(6):1217-24. doi:10.1111/j.1365-2133.2009.09311.x. PubMed
- Argila D, Ortiz‐Romero PL, Ortiz‐Frutos J, Rodriguez‐Peralto JL, Iglesias L. Cutaneous macular amyloidosis associated with multiple endocrine neoplasia 2A. Clin Exp Dermatol. 1996;21(4):313-14. doi:10.1111/j.1365-2230.1996.tb00106.x. PubMed
- Chia B, Tan A, Tey HL. Primary localized cutaneous amyloidosis: association with atopic dermatitis. J Eur Acad Dermatol Venereol. 2014;28(6):810-13. doi:10.1111/jdv.12144. PubMed
- Hashimoto K, Kobayashi H. Histogenesis of amyloid in the skin. Am J Dermatopathol. 1980;2(2):165-71. doi:10.1097/00000372-198000220-00014. PubMed
- Hashimoto K, Ito K, Kumakiri M, Headinton J. Nylon brush macular amyloidosis. Arch Dermatol. 1987; 123: 633–7. PubMed
- Yamagihira M, Kitajima Y, Yaoita H. Ultrastructural observation of the relationship between amyloid filaments and half desmosomes in macular amyloidosis [abstract]. J Cutan Pathol 1980; 7: 213.
- Mehrotra K, Dewan R, Kumar JV, Dewan A. Primary cutaneous amyloidosis: a clinical, histopathological and immunofluorescence study. J Clin Diagn Res. 2017;11(8):WC01-5. doi:10.7860/JCDR/2017/24273.10334. PubMed Central
- Errichetti E, Stinco G. Dermoscopy in general dermatology: a practical overview. Dermatol Ther (Heidelb). 2016;6(4):471-507. doi:10.1007/s13555-016-0141-6. PubMed
- Weidner T, Illing T, Elsner P. Primary localized cutaneous amyloidosis: a systematic treatment review. Am J Clin Dermatol. 2017;18(5):629-42. doi:10.1007/s40257-017-0278-9. PubMed
- Yüksek J, Sezer E, Aksu M, Erkokmaz Ü. Transcutaneous electrical nerve stimulation for reduction of pruritus in macular amyloidosis and lichen simplex. J Dermatol. 2011;38(6):546-52. doi:10.1111/j.1346-8138.2010.01081.x. PubMed
- Hudson LD. Macular amyloidosis: treatment with ultraviolet B. Cutis 1986; 38: 61–2. PubMed
- Esmat SM, Fawzi MM, Gawdar HI, Ali HS, Sayed SS. Efficacy of different modes of fractional CO2 laser in the treatment of primary cutaneous amyloidosis: A randomized clinical trial. Lasers Surg Med. 2015;47(5):388-95. doi:10.1002/lsm.22361. PubMed
- Ostovari N, Mohtasham N, Oadra MS, Maleksad F. 532-nm and 1064-nm Q-switched Nd:YAG laser therapy for reduction of pigmentation in macular amyloidosis patches. J Eur Acad Dermatol Venereol. 2008;22(4):442-6. doi:10.1111/j.1468-3083.2007.02473.x. PubMed
- Barsky M, Buka RL. Pulsed dye laser for the treatment of macular amyloidosis: a case report. Cutis. 2014: 93: 189–92. PubMed
- Fang S, Shen X, Chen AJ, Li S, Shan K. Health-related quality of life in patients with primary cutaneous amyloidosis. PLoS One. 2015;10(3):e0120623. Published 2015 Mar 23. doi:10.1371/journal.pone.0120623.
On DermNet
- Cutaneous amyloidosis
- Systemic amyloidosis: cutaneous features
- Dermatological conditions in skin of colour
- Lichen simplex
- Pigmentation disorders
- Primary cutaneous amyloidosis pathology
Other websites
- Cutaneous amyloidosis — The Australian College of Dermatologists
