Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Authors: Dr Senhong Lee, Clinical Trials Fellow, and Dr Anne Howard, Dermatologist, Skin and Cancer Foundation Inc, Carlton, Melbourne, VIC, Australia. DermNet Editor in Chief: Adjunct A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy edited by Gus Mitchell/Maria McGivern. April 2019.
Introduction Demographics Causes Clinical features Complications Diagnosis Differential diagnoses Treatment Outcome
Onychomatricoma is a rare, benign fibroepithelial tumour of the nail matrix [1].
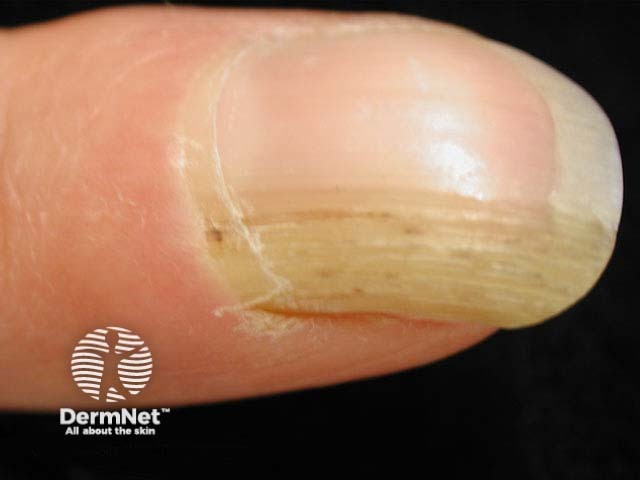
Onychomatricoma typically affects Caucasian women, with a peak incidence in the fifth decade of life. It is rarely observed in children [2].
The exact pathophysiology of onychomatricoma is unknown, although it could be precipitated by trauma [3,4].
Onychomatricoma more commonly affects the fingers than the toes. It could involve either a single digit or multiple digits simultaneously [2,5].
Onychomatricoma is typically slow-growing and painless. Its classic clinical features include [1,4,5]:
Rarer presentations of onychomatricoma include longitudinal melanonychia, [subungual haematoma]([sitetree_link,id=Loading, please wait...]>), and dorsal pterygium [4,6].
Dermoscopic features of onychomatricoma include perforations in the distal portion of the nail plate, haemorrhagic striae, as well as white longitudinal grooves corresponding to the nail plate channels [5].
Onychomatricoma may be complicated by onychomycosis, so both conditions can coexist [1,5]. Delayed diagnosis and treatment are not uncommon due to unfamiliarity with onychomatricoma [2].
Onychomatricoma is diagnosed based on its characteristic clinical features supplemented by dermoscopy, imaging, and histopathology [6].
Imaging may be considered to guide clinical decisions before excision if the presentation is non-specific or unclear [4]. Imaging modalities that could help with diagnosing onychomatricoma include [5,7]:
Histopathological evaluation could be performed on either nail clippings or a resected tumour, which is considered the gold standard [1,4–7]:
Immunohistochemistry although helpful, is not routinely required in typical cases [5].
Common differential diagnoses of onychomatricoma include:
The definitive treatment for onychomatricoma is complete surgical excision [5].
Onychomatricoma typically resolves without local recurrence with complete surgical excision [2,4].