Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author(s): Dr Libby Whittaker, DermNet Medical Writer, New Zealand (2023)
Reviewing dermatologist: Dr Ian Coulson
Edited by the DermNet content department
Introduction
Demographics
Causes
Clinical features
Complications
Diagnosis
Differential diagnoses
Treatment
Prevention
Outcome
Shrimp nail is a curved nail plate that appears similar to the back of a shrimp, caused by repeated onychomadesis. This type of nail disorder may be acquired or congenital.
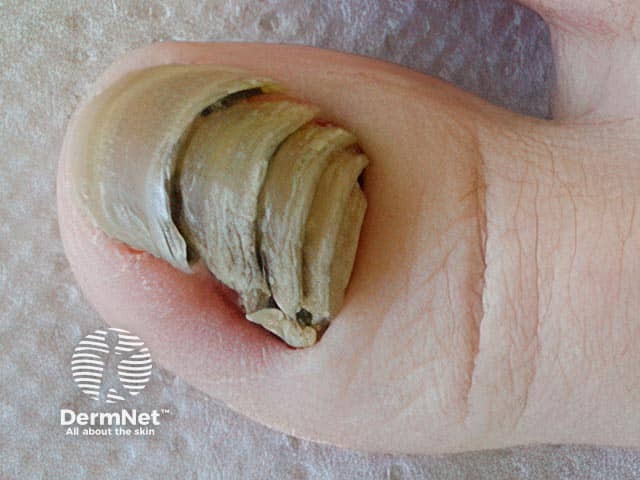
Shrimp nail affecting the great toe - sequential onychomadesis resembling a crustacean (SN-patient2)
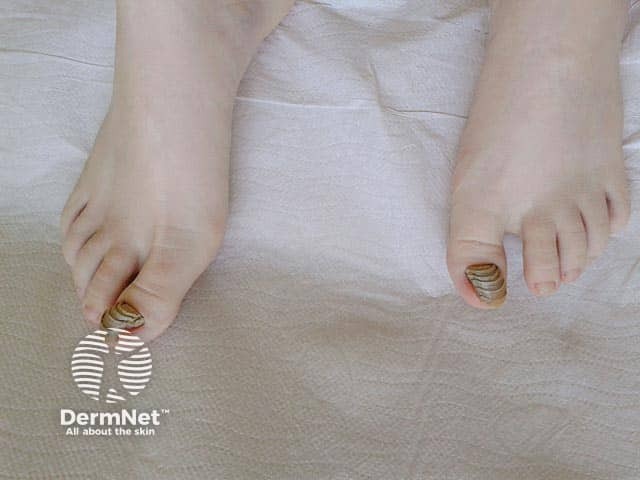
Bilateral shrimp great toenails (SN-patient2)
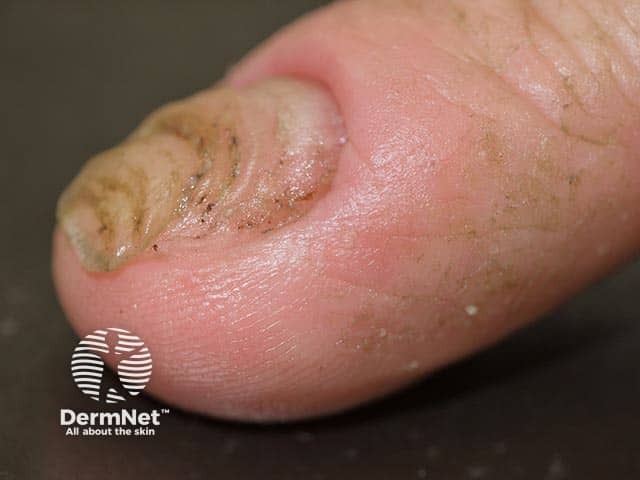
Lateral sequential ridges in early shrimp nail deformity (SN-patient1)
Onychomadesis can develop in both adults and children, including neonates.
There is limited information regarding the epidemiology of shrimp nail specifically. A 2015 Korean study of 21 patients with acquired great toenail dystrophy found that 17/21 had onychomadesis, and 3/17 (23.8%) of those with onychomadesis had shrimp nail.
Nail disorders can be congenital or acquired.
Shrimp nail is caused by repeated onychomadesis, leading to pronounced vertical curvature of the nail. Onychomadesis is related to arrested growth of the nail matrix.
Causes of onychomadesis include:
Shrimp nail may be diagnosed clinically based on its characteristic appearance. A full history and examination should be done to assess for potential causes or triggers.
Nail clippings can be useful in differentiating from other diagnoses such as fungal nail infection.
Minimisation of nail trauma, good nail care and hygiene, and well-fitting footwear may help to reduce nail disorders such as shrimp nail.
Onychomadesis and its specific forms, such as shrimp nail, are usually self-limited, although nail growth and healing can be a slow process. Spontaneous regrowth of a healthy nail will generally occur following resolution of any underlying condition or trigger such as infection or medication use.
Recurrence is possible, and minimisation of nail microtrauma through strategies such as wearing properly fitted shoes is important.