Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Daniel Yiu, Foundation Year Doctor, Department of Infectious Diseases, Wexham Park Hospital, Frimley Health NHS Trust, Slough, Berkshire, UK. DermNet Editor in Chief: Adjunct A/Prof. Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy edited by Gus Mitchell/Maria McGivern. January 2019.
Introduction
Demographics
Causes
Clinical features
Complications
Diagnosis
Differential diagnoses
Treatment
Outcome
Spindle cell melanoma is a rare histological variant of melanoma, characterised by the presence of spindle-shaped melanocytes [1]. On microscopy, it is often mistaken for other skin and soft tissue cancers with spindle cell morphologies.
Desmoplastic melanoma is a variant of spindle cell melanoma where there are varying proportions of spindle cells and desmoplastic cells present in the histology.
Further studies are needed to clarify the clinical manifestations, risk factors, treatment management, and prognosis of spindle cell melanoma.
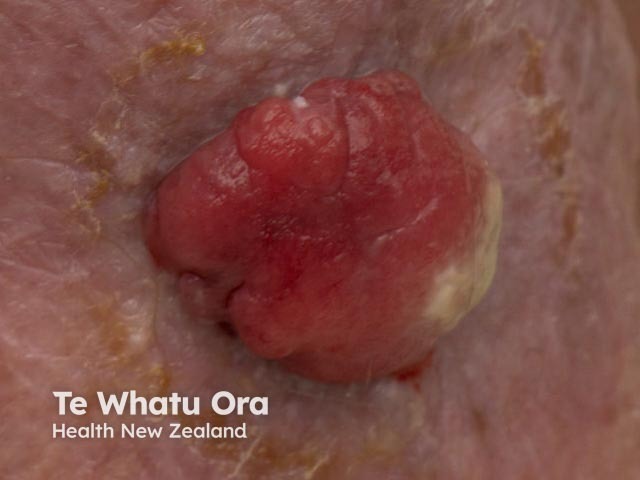
Spindle cell melanoma
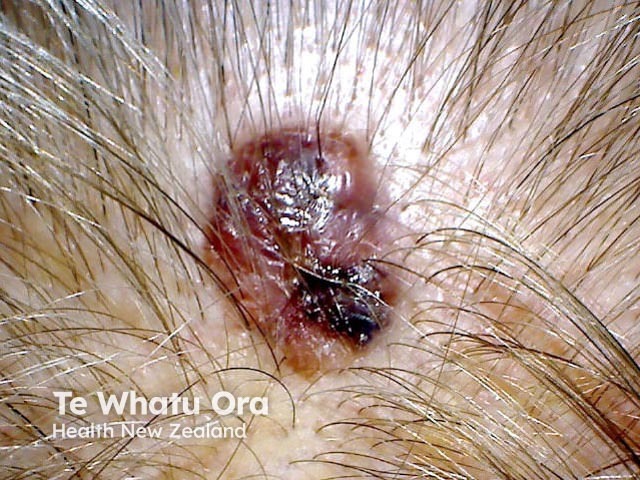
Spindle cell melanoma
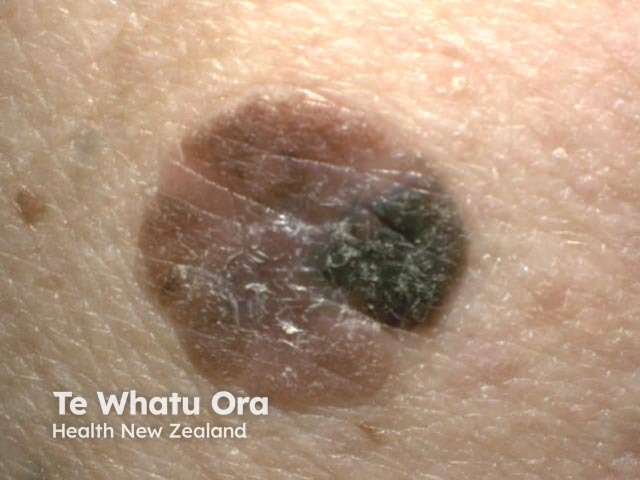
Spindle cell melanoma
The actual incidence of spindle cell melanoma is unknown. Studies have suggested that between 1% and 14% of melanomas are of the spindle cell variant (including desmoplastic melanoma) [2,3].
Spindle cell melanomas more commonly occur in Caucasian men, affecting men and women at a ratio of 1.6:1–1.9:1 respectively. The average age at diagnosis is 50–80 years [1,4].
The exact cause of spindle cell melanoma is unknown. Spindle cell melanoma shares some common mutations with conventional (epithelioid) melanoma.
An association between spindle cell melanoma (including desmoplastic melanoma) and lentigo maligna has been observed in sun-exposed areas [5].
Spindle cell melanoma frequently presents as a non-specific amelanotic (non-pigmented) nodule on the patient's trunk, head, or neck [1,3].
It may also first present as widespread melanoma metastases.
Metastasis is the major complication of spindle cell melanoma. Delays in diagnosis can occur due to its atypical presentation histologically [1–3].
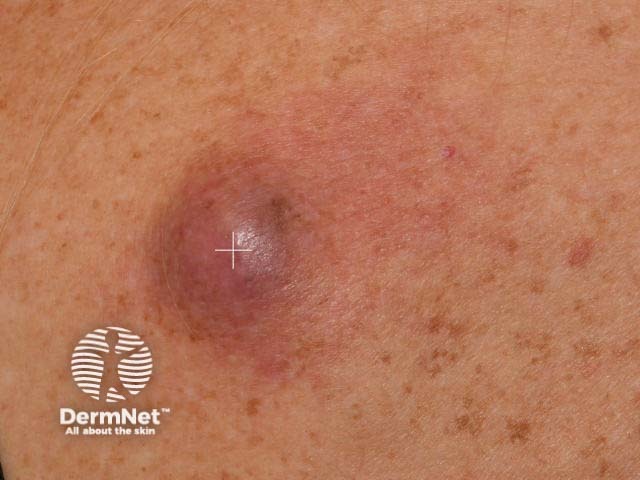
Spindle cell melanoma
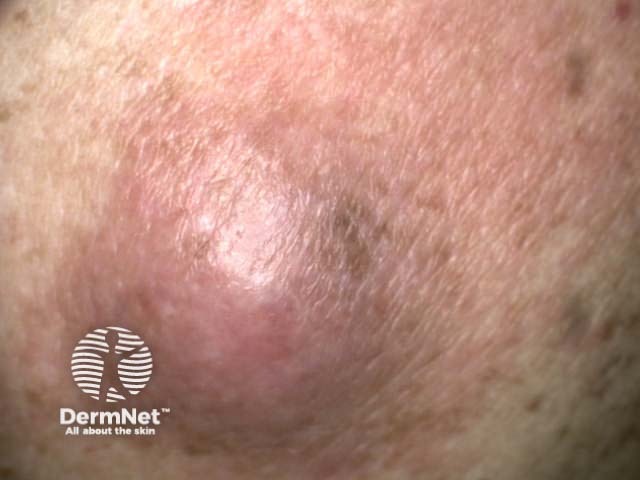
Spindle cell melanoma
Its non-specific features may lead to delays in the diagnosis of spindle cell melanoma, which is often not suspected clinically. The diagnosis is generally made on a biopsy of the lesion, but it can also be commonly mistaken for another tumour histologically [6].
A combination of histological clues and immunohistochemistry markers are required to diagnose spindle cell melanoma [3].
Features of spindle cell melanoma under microscopy include:
Special stains may be used to differentiate spindle cell melanoma from other spindle cell tumours.
Spindle cell melanoma can be easily confused with other spindle cell tumours. Others tumours it can be confused with are described below.
Desmoplastic melanoma was described as a variant of spindle cell melanoma in 1971 [6]. Recent studies now suggest that desmoplastic melanoma and spindle cell melanoma represent two distinct types of melanoma, as differences in staining, genetic mutations, and clinical manifestations have been found [3].
Reed naevus (also called a pigmented spindle-cell naevus) is a melanocytic naevus with a largely spindle-cell appearance under microscopy. The architecture is symmetrical with good lateral demarcation, epidermal hyperplasia, and uniform nests of cells [9].
The differentiation of cutaneous clear cell sarcoma from spindle cell melanoma is largely histological, as both may stain positively for the same indicators: S100, HMB-45, and Melan-A. Cutaneous clear-cell sarcoma tends to show uniform patterns of spindle-cell fascicles (bundles) under microscopy, which are present throughout an entire tumour and encased by fibrous septa. The stroma tends to be hyalinised, sclerotic, and reticulated [13].
Leiomyosarcoma pathology may be indistinguishable morphologically from melanoma.
The markers S100, p75, and HMB-45 are negative after staining in atypical fibroxanthoma [10].
The treatment for spindle cell melanoma is similar to that for other forms of melanoma. Surgical excision is the first step in management [1].
Although the tendency for nodal involvement is low, the majority of spindle cell melanomas present with advanced disease, with a worse prognosis being seen in Caucasian men aged over 66 years [3].
Advanced disease with nodal and distal metastasis is associated with worse outcomes in spindle cell melanoma, as are higher grades of tumours, which have been associated with poorer disease-specific survival and overall survival [1].