Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Acquired dermal macular hyperpigmentation — extra information
Acquired dermal macular hyperpigmentation
Authors: Ko Jin Quek, Junior Medical Officer, South-Western Sydney Local Health District, Sydney, NSW, Australia; Dr Monisha Gupta, Dermatologist, Sydney, Australia. DermNet Editor in Chief: Adjunct A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy edited by Gus Mitchell. January 2020.
Introduction Demographics Causes Clinical features Complications Diagnosis Differential diagnoses Treatment Outcome
What is acquired dermal macular hyperpigmentation?
Acquired dermal macular hyperpigmentation, also called acquired macular pigmentation of unknown aetiology, comprises three conditions:
- Erythema dyschromicum perstans
- Lichen planus pigmentosus
- Idiopathic eruptive macular hyperpigmentation.
The term acquired dermal macular hyperpigmentation is useful because the three conditions overlap. The subtypes may manifest in the same patient, and they lack clear-cut clinical and histological differences.
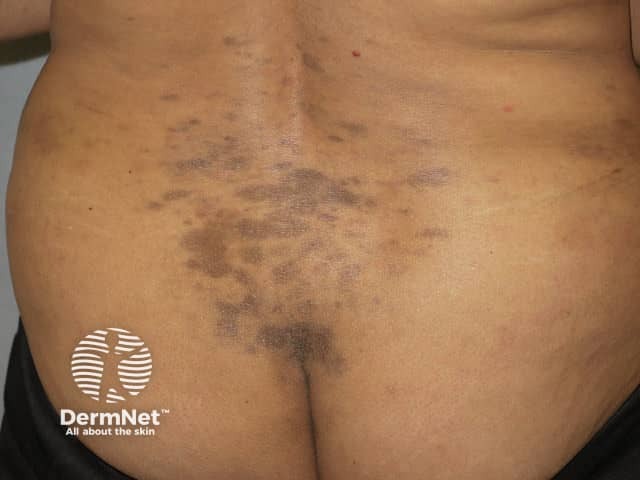
Lichen planus pigmentosus of lower back
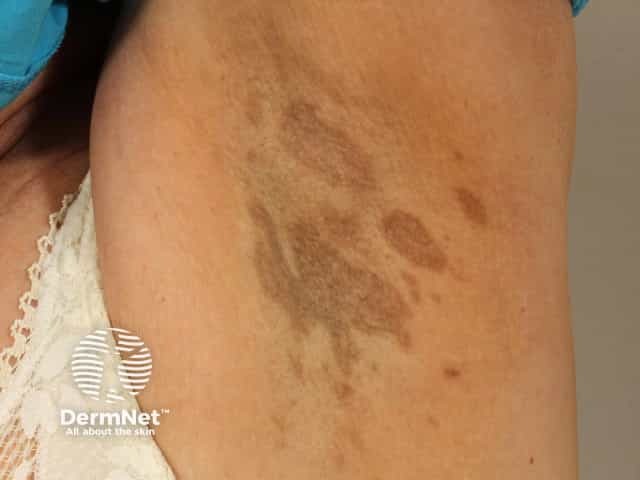
Acquired dermal macular hyperpigmentation
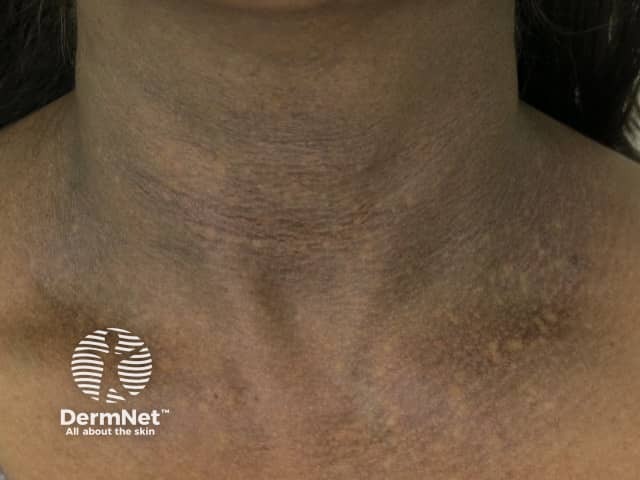
See more images of acquired macular hyperpigmentation.
Who gets acquired dermal macular hyperpigmentation?
The epidemiology of acquired dermal macular hyperpigmentation varies depending on the underlying condition.
Erythema dyschromicum perstans can affect any age, sex, and ethnicity, and tends to affect darker-skinned patients. Asian, Middle-Eastern, and Latin American women between the 2nd and 4th decades of life are the most frequently affected. Whereas idiopathic eruptive macular hyperpigmentation develops in the first two decades of life. Lichen planus pigmentosus affects middle-aged people of South Asian and African/Middle Eastern descent.
What causes acquired dermal macular hyperpigmentation?
The exact cause of acquired dermal macular hyperpigmentation is unknown.
Proposed theories for the pathogenesis of acquired dermal macular hyperpigmentation include:
- Genetic susceptibility
- Exposure to ultraviolet (UV) radiation
- Contact reaction to a chemical (up to 36% of patients were reported to have a positive patch test reaction to hair dye), although this would now be termed pigmented contact dermatitis
- Exposure to a drug such as hydroxychloroquine, however this would now be labeled as drug-induced hyperpigmentation
- A viral infection.
The pigmentation in acquired dermal macular hyperpigmentation is often due to persistent melanophages in the dermis. The reason the melanophages do not clear as usually occurs is unknown.
What are the clinical features of acquired dermal macular hyperpigmentation?
Acquired dermal macular hyperpigmentation presents with blue, brown, slate grey or brownish-black macules, which can change in size and morphology over time.
- Lichen planus pigmentosus and idiopathic eruptive macular hyperpigmentation affect the face, neck, and proximal extremities.
- Erythema dyschromicum perstans affects the trunk and sun-protected locations, typically with an erythematous margin initially.
- Large macules greater than 5 cm in diameter are seen in lichen planus pigmentosus and erythema dyschromicum perstans.
- Small macules 0.5—2 cm in size occur in idiopathic eruptive macular hyperpigmentation and lichen planus pigmentosus.
- Lichen planus pigmentosus is only rarely reported in patients with current or past classic lichen planus.
Acquired dermal macular hyperpigmentation is generally asymptomatic, although lichen planus pigmentosus is sometimes pruritic in its early phases.
What are the complications of acquired dermal macular hyperpigmentation?
No detrimental serious long-term medical complications arise from acquired dermal macular hyperpigmentation. However, it impacts on the quality of life in people with skin of colour due to cosmetic visibility and slow resolution.
How is acquired dermal macular hyperpigmentation diagnosed?
The diagnosis of acquired dermal macular hyperpigmentation and its subtypes are based on the cutaneous features and detailed history.
A detailed history is required to exclude medications, virus infection, and inflammatory skin conditions.
Patch testing may be indicated to exclude allergic contact dermatitis if there is a possible contact factor.
Dermoscopy is useful in the diagnosis and monitoring of acquired dermal macular hyperpigmentation. Findings may include:
- Pigmented dots, globules and diffuse areas that spare eccrine and hair follicle openings
- Prominent normal pseudoreticular pigmentary network
- Telangiectasia
- Owl's eye structures.
Histological features of acquired dermal macular hyperpigmentation on skin biopsy may include and help to determine the diagnosis:
- Melanin and melanophages in the dermis
- Lichenoid changes with an interface dermatitis.
What is the differential diagnosis for acquired dermal macular hyperpigmentation?
A variety of other skin conditions appear similar to acquired dermal macular hyperpigmentation, such as:
- Postinflammatory hyperpigmentation
- Drug-induced hyperpigmentation
- Multiple lesions of fixed drug eruption
- Macular amyloidosis
- Maculopapular cutaneous mastocytosis.
What is the treatment for acquired dermal macular hyperpigmentation?
The treatment of acquired dermal macular hyperpigmentation depends on the subtype and its duration, but many therapies have been tried with little or no benefit.
- Any identified contact allergen should be avoided.
- Colchicine has been used to improve macrophage activity and thus clear dermal pigmentation.
- In the acute inflammatory stage of lichen planus pigmentosus, topical steroid, a topical calcineurin inhibitor, and oral corticosteroid can be considered.
- In later stages or where there is no acute inflammation, treatment aims to reduce pigmentation; stringent sun protection is advised. Topical retinoids may reduce melanin that is retained within the epidermis.
- Suggested treatments for erythema dyschromicum perstans have included dapsone, clofazimine, corticosteroid and immunosuppressants without much evidence of efficacy.
- Idiopathic eruptive macular hyperpigmentation resolves spontaneously so does not usually require treatment.
What is the outcome for acquired dermal macular hyperpigmentation?
Idiopathic eruptive macular hyperpigmentation tends to resolve spontaneously within months to years. In contrast the pigmentation of lichen planus pigmentosus can persist for decades and erythema dyschromicum perstans tends to be chronic and progressive.
References
- Sasidharanpillai S, Govindan A, Ajithkumar KY, et al. Histological evaluation of acquired dermal macular hyperpigmentation. Indian Dermatol Online J 2019; 10: 542–6. doi: 10.4103/idoj.IDOJ_426_18. PubMed Central
- Udompanich S, Vachiramon V. Acquired macular pigmentation of unknown etiology. J Clin Aesthet Dermatol 2019; 12: 38–46. PubMed Central
- Rodrigues M, Pandya AG, Bekkenk M, Parsad D, Kumarasinghe SP. Current understanding of lichen planus pigmentosus, erythema dyschromicum perstans (ashy dermatosis), and idiopathic eruptive macular pigmentation. Pigment Int 2019; 6: 4–8. doi: 10.4103/Pigmentinternational.Pigmentinternational. Journal
- Chang SE, Kim HW, et al. Clinical and histological aspect of erythema dyschromicum perstans in Korea: a review of 68 cases. J Dermatol 2015; 42: 1053–7. doi: 10.1111/1346-8138.13002. PubMed
- Kumarasinghe SPW, Pandya A, Chandran V, et al. A global consensus statement on ashy dermatosis, erythema dyschromicum perstans, lichen planus pigmentosus, idiopathic eruptive macular pigmentation, and Riehl's melanosis. Int J Dermatol 2019; 58: 263–72. doi: 10.1111/ijd.14189. PubMed
- Bishnoi A, Vinay K, Arshdeep, et al. Contact sensitization to hair colours in acquired dermal macular hyperpigmentation: results from a patch and photo-patch test study of 108 patients. J Eur Acad Dermatol Venereol 2019; 33: 1349–57. doi: 10.1111/jdv.15576. PubMed
- Vinay K, Bishnoi A, Parsad D, Saikia UN, Sendhil Kumaran M. Dermatoscopic evaluation and histopathological correlation of acquired dermal macular hyperpigmentation. Int J Dermatol 2017; 56: 1395–9. doi: 10.1111/ijd.13782. PubMed
- Kanwar AJ, Parsad D. Colchicine in the treatment of Lichen Planus Pigmentosus, XXIst International Pigment Cell Conference, Bordeaux, France, 2011.
- Al-Mutairi N, El-Khalawany M. Clinicopathological characteristics of lichen planus pigmentosus and its response to tacrolimus ointment: an open label, non-randomized, prospective study. J Eur Acad Dermatol Venereol 2010; 24: 535–40. doi: 10.1111/j.1468-3083.2009.03460.x. PubMed
- Bahadir S, Cobanoglu U, Cimsit G, Yayli S, Alpay K. Erythema dyschromicum perstans: response to dapsone therapy. Int J Dermatol 2004; 43: 220-2. doi: 10.1111/j.1365-4632.2004.01984.x. PubMed
- Kontochristopoulos G, Stavropoulos P, Panteleos D, Aroni K. Erythema dyschromicum perstans: response to dapsone therapy. Int J Dermatol 1998; 37: 796–8. doi: 10.1046/j.1365-4362.1998.00522.x.
On DermNet
- Erythema dyschromicum perstans
- Lichen planus
- Idiopathic eruptive macular hyperpigmentation
- Acquired dermal macular hyperpigmentation images
- Macular amyloidosis
- Pigmentation disorders
