Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Vanessa Ngan, Staff Writer, 2003. Updated by Dr Ebtisam Elghblawi, Dermatologist, Tripoli, Libya. April 2017.
Introduction Causes Clinical features Diagnosis Differential diagnoses Treatment
Alopecia mucinosa, also known as follicular mucinosis, describes the appearance of mucin around hair follicles as seen under the microscope. It is characterised by bald patches of skin in which hair follicles are prominent.
Mucins look like stringy clear or whitish goo mainly composed of hyaluronic acid, a normal component of the ground substance surrounding collagen in the dermis. Several other forms of mucinosis are described and classified.
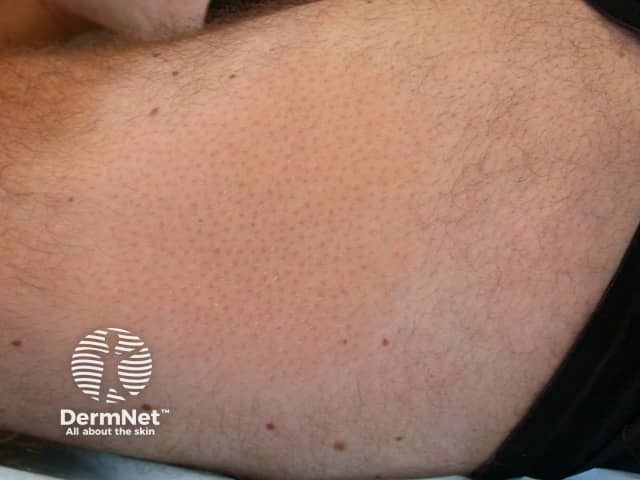
Alopecia mucinosa
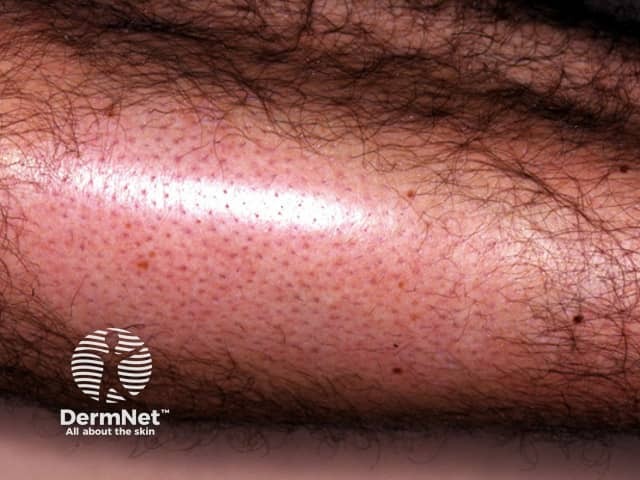
Alopecia mucinosa
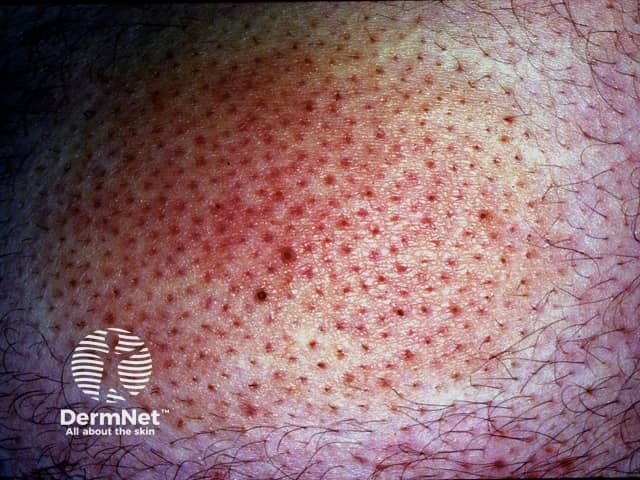
Alopecia mucinosa
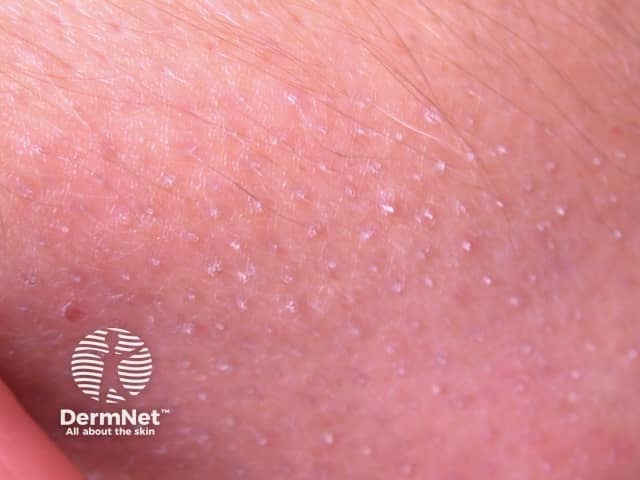
Alopecia mucinosa
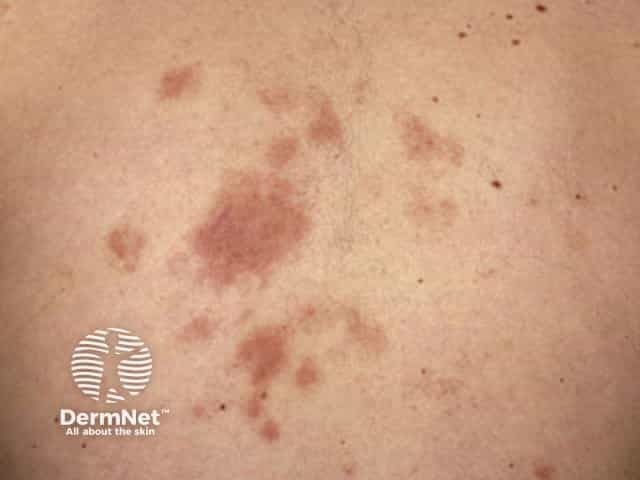
Alopecia mucinosa
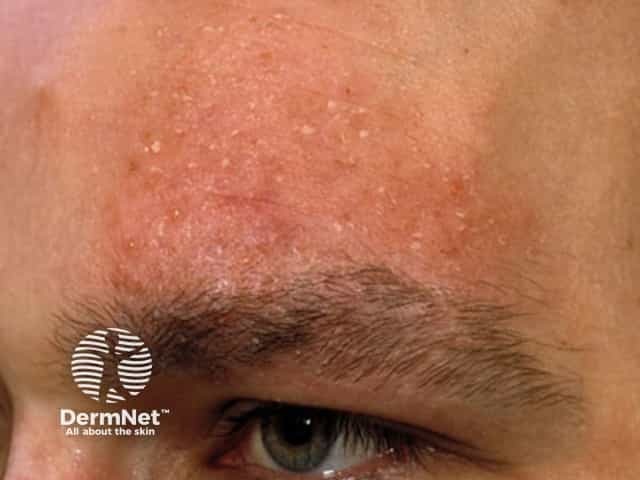
Alopecia mucinosa
The cause of alopecia mucinosa is unknown, but it may have something to do with circulating immune complexes and cell-mediated immunity. What is known is that mucinous material deposits and accumulates in hair follicles and sebaceous glands to create an inflammatory condition that subsequently breaks down the ability of the affected follicles to produce hair.
Alopecia mucinosa most commonly affects face, neck and scalp, but any part of the body may be affected.
Alopecia mucinosa is diagnosed by its clinical appearance and supported by histopathological findings on biopsy:
Histological features of the underlying disease are present in secondary alopecia mucinosa.
Secondary causes of alopecia mucinosa such as mycosis fungoides may not be diagnosed for some years, necessitating careful follow-up and biopsy. Other conditions that may need to be considered in the differential diagnosis include:
There is no proven effective treatment for alopecia mucinosa. Usually, primary and acute alopecia mucinosa occurring in children resolves spontaneously. Because there is a small chance of spontaneous resolution for other forms of the disease, the effect of treatment can be difficult to assess. Some treatments that have been tried with limited success include:
Secondary alopecia mucinosa should be treated appropriately for the underlying skin disease, particularly if it is cutaneous T-cell lymphoma.